NUCHAL (NT) SCAN: DIAGNOSTIC ULTRASOUNDS IN LONDON
Nuchal translucency (NT) is assessed during our Early Fetal Scans from 10-14 Weeks. We also offer a private Nuchal Scan in London as a second opinion scan.
We have vast experience in measuring NT – our YouTube training videos have millions of views worldwide.
Our Nuchal Scan in London Offers You Much More
The NT Scan screening method was developed more than 30 years ago. While it is an important marker that we pay special attention attention to it in scans from 10 weeks, ultrasound technology and expertise have improved a lot since the 1990’s allowing us to screen for many more anomalies.
Traditionally, Nuchal Translucency is measured from 11-13 weeks. Recent research shows that there is merit for identifying increased measurements from as early as 10 weeks, when you may want to opt in for NIPT.
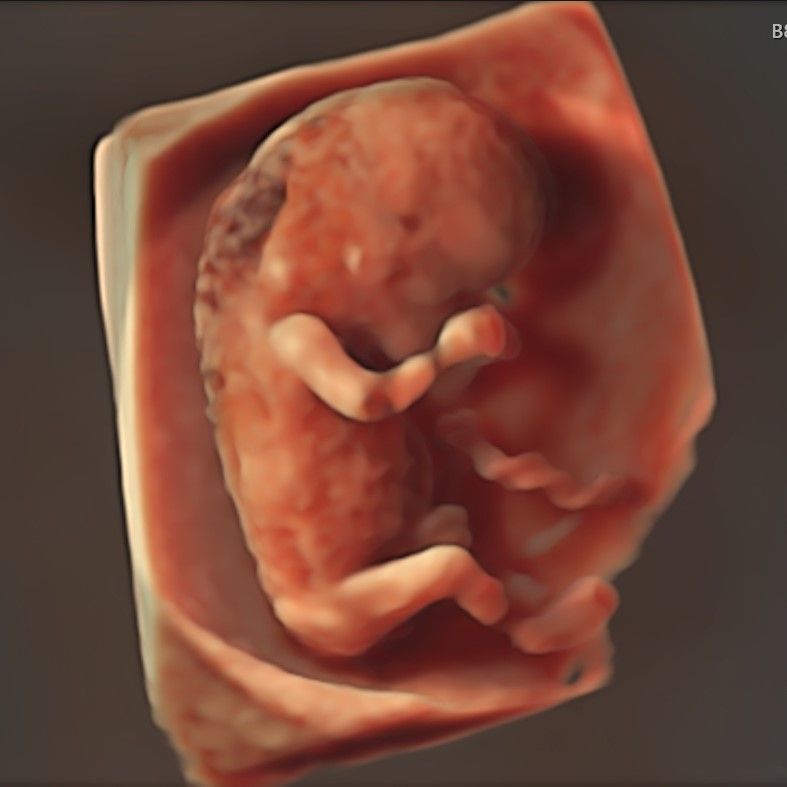
Baby with Increased NT visualised in 3d at 10-11 Week Scan
Nuchal Translucency at London Pregnancy Clinic
-
Worried about increased NT? – second opinion scans available with Fetal Medicine Doctors.
-
Our Nuchal Translucency measurement comes with a wider range of anomaly screening using ultrasound available at the point of scan.
-
We consider NT from the earliest stage at our 10 Week Scan.
-
10-week anomaly scan – our revolutionary scan to exclude 10 severe structural anomalies at 10 weeks. This scan is designed to complement NIPT screening as a comprehensive structural and chromosomal anomaly screening solution.
-
Private early pregnancy scan at 12-16 weeks to exclude >100 different structural anomalies
-
Anomaly scan + NIPT options – harmony or panorama NIPT from 9 weeks (from £490)
-
Scans and NIPT appointment with our fetal medicine specialist doctors and specialist sonographers with extensive NHS and international experience.
-
Same day, evening, and weekend appointments
-
NIPT results in 2-4 working days as early as 9 weeks
-
Latest 3D/4D ultrasound technology
-
5* rated service on Google, Trustpilot & Doctify
NT Scan in London Explained
The nuchal translucency (NT) scan is a sonographic (imaging) phenomena, which measures the amount of fluid in the filled area under the skin and at the back of the baby’s neck. NT is a non-specific (surrogate) marker of fetal well-being that may be increased in the case of trisomy 21 (Down’s syndrome), Edward’s syndrome, Patau’s syndrome, fetal heart defects, or other structural anomalies. This means that even babies with normal development may experience increased nuchal translucency – higher NT does not automatically indicate a fetal abnormality.
During the screening test, if the baby is found to have only an increased NT without any other genetic or chromosomal anomalies, it is believed that the nuchal fluid will resolve on its own and the child will be completely healthy. A small proportion of babies with an isolated increase in NT have genetic syndromes or anomalies, which are undetectable before birth.
The NHS consider any NT thickness measurement below 3.5 mm to be normal. However, normal measurements do not rule out all anomalies for your baby but do indicate a lower chance of having a chromosomal problem. More than 50% of babies with severe heart defects, 25% of babies with Down’s syndrome, and the majority of babies with other anomalies will have had a completely normal nuchal dating scan.
In order to gain a better understanding of your baby’s well-being, we use advanced technology to perform an early fetal scan, which is a thorough top-to-toe examination of the fetal anatomy. This allows us to exclude many fetal anomalies by having a closer look at the heart, spine, and brain, among other organs. Additionally, we use a nuchal translucency scan to assess the chance of trisomy 21 (Down’s syndrome). The combination of these approaches is a much more effective way to exclude anomalies than NT measurements alone.
With our expertise and technology, we are able to screen for structural anomalies from 10 weeks (approximate prevalence in the first trimester):
- Acrania (1:1,000)
- Alobar Holoprosencephaly (1:1,300)
- Spina Bifida (1:2,000)
- Absence of arms, hands, legs or feet (1:2,000)
- Encephalocele (1:5,000)
- Exomphalos (Omphalocele) with liver (1:3,500)
- Amniotic Band Anomaly (1:7,000)
- Body Stalk Anomaly (1:7,500)
- Sirenomelia (1:60,000)
- Conjoined Twins (1% of monochorionic twins)
In comparison, the prevalence of the chromosomal conditions screened for by NIPT:
- Down’s Syndrome (1:700)
- Edward’s Syndrome (1:1400)
- Patau’s Syndrome (1:5000)
If you take the pregnancy test at 12+ weeks we are able to screen for >200 structural fetal anomalies.
NT is an important non-specific marker of your baby’s well-being, where babies with an increased NT measurement require further evaluation.
We routinely measure NT thickness during the early fetal scan; however, we do not use this to calculate your baby’s chances of having Trisomy 21 (Down’s syndrome). Instead, we use NIPT, which has a much higher detection rate and a lower false positive rate compared to NT measurement.
Alternatively, we use 3.5 mm (NT thickness) as a cut-off for the referral of expecting mothers to a fetal medicine unit for further counselling in accordance with NHS guidelines.
Early fetal echocardiography or early echo is a special detailed scan for the baby’s heart, which we can perform as early as from 12 weeks.
We highly recommend this scan for all babies with increased nuchal translucency (NT) measurements, fetal anomalies, or other unusual findings detected at the 11-13 weeks scan.
NT thickness measurements are included in the early fetal scan and can be done for free during the advanced early fetal assessment.
Please book the Early Fetal Scan or our all-inclusive early fetal reassurance package: ultrasound scanning and NIPT working together, which is an optimal combination for excluding fetal anomalies in the first trimester (done at 10-13 weeks).
Get in touch with our team to learn more about our Nuchal Scan in London done at 12 weeks.
10-week scan and NIPT is the best option for early first trimester screening. It is an advanced test that checks for both the most severe structural defects and most common chromosomal abnormalities.
This test is optimal together with the early fetal scan at 16 weeks as a part of our EARLY FETAL REASSURANCE PACKAGE.
Prior to the invention of NIPT (non-invasive prenatal testing), NT thickness was the most effective screening method for trisomy 21 (Down’s syndrome).
About 8-10 years ago, we were actively involved training medical professionals (doctors and sonographers) in performing the NT assessment. As a part of this program, we had created training videos that have been uploaded to YouTube. Overtime, these videos have become one of the most popular NT videos with nearly 700,000 views.
If you click the link below, you will be able to watch these videos, although we would like you to be aware that they are old and have not been updated, because when they were created, 10 years ago, before the era of NIPT, they represented the most advanced information we had about NT measurements.
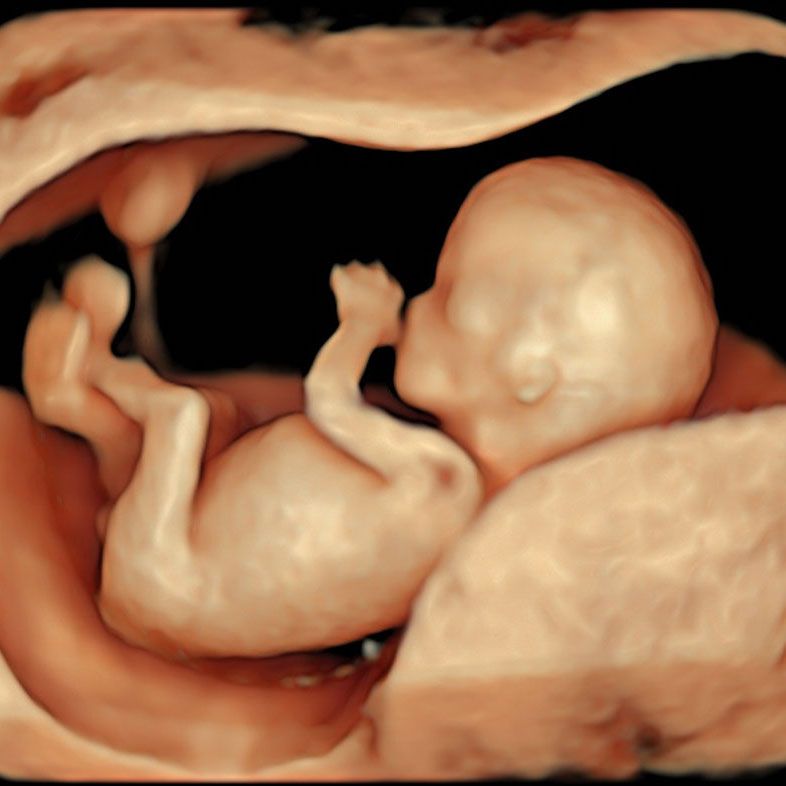
3D ultrasound of a fetus at 12 weeks captured on our Early Fetal Scan
The best EARLY PREGNANCY scans and tests schedule would be:
Location of the pregnancy
Viability of the baby (babies)
Number of babies
Dating of pregnancy (EDD – estimated delivery date)
Screening for 10 most severe structural anomalies
Screening for Down’s syndrome and other chromosomal defects
Optional gender reveal by NIPT
Screening for more than 100 different serious structural anomalies
Optional gender reveal by scan
We have created a special EARLY FETAL REASSURANCE PACKAGE to address our patients need for early support.
Early echo is our special scan to confirm normal development of the baby’s heart. From 12 weeks we can exclude up to 80% prenatally detectable severe fetal heart defects.
This scan is highly recommended if you baby has increased nuchal translucency (NT), or other unusual findings or anomalies on your 1st trimester scan.
Early echocardiography includes a comprehensive check of all other fetal structures and organs like we do at the early fetal scan.
Read more about early fetal echocardiography here:
Early fetal echocardiography is the most advanced scan you can perform in the first trimester from 12 weeks.
This special scan includes:
- expert examination of the fetal heart and great vessels
- early fetal neurosonography: special examination of the brain
- comprehensive top-to-toe examination of all baby’s structures
- measurements of nuchal translucency NT thickness (at 12-13 weeks) or nuchal fold afterwards
To learn more about early fetal echocardiography, click here.
Nuchal translucency (NT) is a collection of fluid under the skin of the baby’s neck. It considered as an indirect marker for fetal anomalies (chromosomal and structural). The nuchal translucency (NT) scan was developed in the 1990s when it was impossible to perform a proper check of the fetal structures due to low resolution of old ultrasound scanners.
On the early fetal scan or early fetal echocardiography we perform state-of-the-art checks for all fetal anatomy and especially for the brain, spine and the heart. Those scans are superior to the NT scan, because they look for all of the baby instead of measuring the fluid in the back of the fetal neck. Saying that, we still offer measurements of NT for all our patients (at 11-13 weeks). If the measurement is 3.5 mm or above, we will perform the early fetal echocardiography for free.
We do not use NT for calculation of the chances for Down’s syndrome because of it false-negative and false positive results. For Down’s syndrome screening we use NIPT, which is much more accurate test.
We recommend taking the NIPT along with our comprehensive early anomaly scan as soon as possible – 10 weeks. Early detection of either chromosomal or structural anomalies allows more time in terms of pregnancy management for those conditions.
If you’re unsure about the age of your pregnancy, please allow a couple of days after the 10-week mark to avoid repeat appointments for drawing the bloods.
In theory, NIPT is available from 10-40 weeks, but it is strongly recommended to take the test in the first trimester, as the pregnancy management options in the second trimester are very limited.
In case the NIPT results in a high chance for Down’s/Edward’s/Patau’s syndromes our doctor will contact you and explain the further steps we advise to take. We will most likely arrange a referral to your NHS fetal medicine unit for further counselling and possible diagnostic tests such as CVS or amniocentesis.
Alternatively, we can refer you to a private fetal medicine consultant (consultation cost is not included in our service.)
We will also offer you our early fetal echocardiography for free, in the case you wish to know the condition of your baby’s heart (if it has a congenital heart defect).
The combined test is a screening test during pregnancy that looks for three specific chromosomal anomalies – Down syndrome, trisomy 18, and trisomy 13. It involves a combination of two blood tests and an ultrasound.
Specifically, the combined test includes:
- Blood test for pregnancy-associated plasma protein A (PAPP-A) – Measures protein levels associated with Down syndrome risk. Done in first trimester.
- Blood test for human chorionic gonadotropin (hCG) – Measures hormone levels associated with Down syndrome risk. Done in first trimester.
- Ultrasound – Measures nuchal translucency thickness at the back of the fetus’s neck. Increased thickness indicates higher risk. Done at 11-14 weeks.
The results of the blood tests and ultrasound are put into a mathematical equation that calculates the individualized risk for each chromosomal anomaly. The combined test can detect around 80% of Down syndrome pregnancies and around 77% of trisomy 18 cases.
If the calculated risk is high, further diagnostic testing may be recommended, such as amniocentesis or chorionic villus sampling. The combined test provides an effective way to noninvasively screen for major chromosomal abnormalities early in pregnancy.
There are a few key reasons that non-invasive prenatal testing (NIPT) is being favoured over the traditional combined test for prenatal screening of chromosomal abnormalities:
- Accuracy – NIPT is far more accurate than the combined test. NIPT has detection rates of around 99% for Down syndrome compared to 80-90% with the combined test. This means fewer false positives and false negatives.
- Earlier screening – NIPT can be done as early as 10 weeks into pregnancy versus 11-14 weeks for the combined test’s ultrasound component. This gives families more time to consider options.
- Less invasive – The combined test requires a blood draw. NIPT only requires a blood sample from the mother’s arm. No risk of miscarriage as with amniocentesis.
- Screens for more – NIPT screens for Down syndrome, trisomy 18, and trisomy 13. It can also test for sex chromosome anomalies and microdeletions. The combined test only looks for the main trisomies.
- Cost – While NIPT costs more than the combined test, the prices have dropped significantly in recent years making it more affordable. Insurers are increasingly covering NIPT due to its superiority.
- Patient preference – Women often prefer the ease and accuracy of NIPT over the combined test.
In summary, NIPT is becoming the dominant choice for prenatal screening due to its accuracy, minimal invasiveness, additional chromosomal coverage, and patient satisfaction. However, the combined test may still be used in some cases when NIPT is unavailable.
The quadruple test (also called the quad screen) is another type of prenatal screening test for chromosomal abnormalities like Down syndrome. It involves:
- Blood test for alpha-fetoprotein (AFP) – Made by the fetus, low levels associated with Down syndrome risk
- Blood test for estriol (uE3) – A placental hormone, low levels indicate risk
- Blood test for inhibin-A – Made by the placenta, abnormal levels indicate risk
- Blood test for hCG – Made by placenta, abnormal levels indicate risk
The quadruple test is done between 15-20 weeks of pregnancy. The blood results give a risk assessment for Down syndrome and neural tube defects.
Some key reasons NIPT is considered superior to the quadruple screen:
- NIPT is more accurate – over 99% detection rate for major trisomies versus about 80% for quadruple
- NIPT screening can be done earlier, as early as 10 weeks
- NIPT is non-invasive, only requires a blood sample from the mother
- Lower false positive rate with NIPT
- NIPT tests directly for fetal DNA versus indirect markers in quadruple
- NIPT provides risk assessment for a broader range of chromosomal abnormalities
- NIPT is becoming more affordable and accessible
Overall, NIPT is advantageous over the quadruple test due to its greater accuracy, wider range of screening, ability to be performed earlier in pregnancy, and non-invasive nature.


