Expert Pelvic Scan Services in London | London Pregnancy Clinic
A pelvic scan is a non-invasive ultrasound procedure. It provides detailed images of pelvic organs including the uterus, ovaries, and bladder.

Expert Pelvic Scan: Gynaecological Transvaginal Ultrasound
A gynaecological pelvic scan is a crucial diagnostic tool for women’s health. It’s also known as a gynae pelvic ultrasound or baseline scan. This scan generates detailed images of the female reproductive organs – the uterus, cervix, fallopian tubes, and ovaries. It aids in diagnosing and monitoring conditions like ovarian cysts, uterine fibroids, endometriosis, and pelvic inflammatory disease, providing essential insights for fertility assessment and pregnancy monitoring.
At London Pregnancy Clinic, Pelvic Scans are performed by highly trained Gynaecology Speciality Sonographers on the latest ultrasound equipment. The images/videos and ultrasound report will be shared with you immediately post the scan and can be sent to your primary healthcare provider/GP.
Our advanced ultrasound equipment allows superior image and screening
Why Choose London Pregnancy Clinic for Your Pelvic Scan
-
We use the latest ultrasound equipment from GE – Voluson E10 at its BT20 configuration
-
Our pelvic ultrasound scans include Follicular Tracking, also known as Antral Follicle Count include a 3D assessment where appropriate
-
Scan with a specialist sonographer with a wealth of experience in gynaecology and fertility scans
-
Detailed ultrasound report and images promptly sent to you and to your referring consultant or clinic
-
At London Pregnancy Clinic we are specialists in Gynaecology and Reproductive health
-
Consultant Gynaecologist available for consultations to discuss the scan report for an additional fee.
-
Same day, evening and weekend appointments
-
5* rated service on Doctify, TrustPilot and Google
What to Expect from Your Pelvic Scan in London
A pelvic gynaecological scan is a detailed ultrasound designed to assess the health and functionality of the reproductive organs, including the uterus, ovaries, and cervix. It is often used in fertility treatments or for women experiencing gynaecological symptoms.
Purpose of the Pelvic Gynae Scan:
- Fertility Assessment: The scan helps evaluate fertility and suitability for assisted reproductive therapies, including IVF, egg freezing, or surrogacy.
- Treatment Planning for IVF: It provides critical information to plan fertility treatments, such as determining the best timing for conception or assessing ovarian reserve.
- Monitoring Progress: The scan is essential for tracking the effectiveness of ongoing fertility or gynaecological treatments.
What’s Included in a Pelvic Gynae Scan?
- Measures the thickness and structure of the uterine lining to evaluate its readiness for implantation. It detects any abnormalities, such as fibroids or polyps, which could impact fertility or overall uterine health.
-
Follicle Tracking (Antral Follicle Count – AFC):
Counts the number of follicles within the ovaries to estimate ovarian reserve, which is key for assessing fertility potential. It also helps track ovulation and timing for fertility treatments. -
Overall Uterine and Ovarian Health:
Identifies structural issues, cysts, or other abnormalities in the reproductive organs. It checks for signs of conditions like endometriosis or PCOS.
Why is a Pelvic Gynae Scan Important?
This comprehensive scan serves as a baseline assessment for women considering assisted reproductive therapies or fertility preservation. It not only guides treatment plans but also provides reassurance by offering a clear understanding of the reproductive health status.
If you are planning fertility treatment or have concerns about your reproductive health, the pelvic gynaecological scan is an essential diagnostic tool. Reach out to our clinic today to schedule your scan and take the next step in your journey.
A pelvic scan might be recommended if you are experiencing any of the following symptoms:
- Persistent pelvic pain
- Unusual menstrual cycles, including heavy bleeding or irregular periods
- Difficulty or discomfort during urination
- Frequent urination
- Lower back pain that cannot be attributed to other causes
- Abnormal vaginal bleeding or discharge
- Pain or discomfort during sexual intercourse
- Unexplained weight loss
- A palpable mass in the pelvic area
- Infertility issues or complications during pregnancy
- Symptoms suggesting pelvic inflammatory disease, endometriosis, or ovarian cysts
- Screening for uterine fibroids or polyps
Please note, this is not an exhaustive list, and the presence of these symptoms does not automatically indicate a serious health issue. However, any persistent or unusual symptoms should be discussed with your healthcare provider.
Our scans are performed by our specialist sonographer who will provide detailed ultrasound scan report as well as the images from your scan. These will be sent to you securely via our cloud sharing system Tricefy.
We can also arrange your results to be sent to your referring clinic for them to discuss and interpret the results for the continuation of your treatment.
The patient must discuss the results of the ultrasound and blood tests with their referring clinician/IVF consultant.
Our sonographers will not be able to interpret the results of the scan for you, and it is important for a qualified professional in fertility and reproductive medicine to explain the results to you.
If you require a consultation, please note that our consultant gynaecologist – Mr Prashant Purohit is available for a consultation for an additional fee. You can learn more about those services by following the link below.
A gynaecological pelvic scan can help diagnose a range of conditions related to female reproductive health. These include:
-
Uterine Fibroids: These are noncancerous growths in the uterus that often appear during childbearing years.
-
Ovarian Cysts: Fluid-filled sacs or pockets that form on or in an ovary.
-
Endometriosis: A disorder where the tissue that normally lines the inside of the uterus grows outside the uterus.
-
Pelvic Inflammatory Disease (PID): An infection of the female reproductive organs, usually caused by sexually transmitted bacteria.
-
Polycystic Ovary Syndrome (PCOS): A hormonal disorder common among women of reproductive age, where the ovaries may develop numerous small collections of fluid.
-
Ectopic Pregnancy: A pregnancy that occurs outside the uterus, typically in a fallopian tube.
-
Gynaecological Cancers: Including ovarian, uterine, cervical, and endometrial cancer.
-
Pregnancy Complications: Including miscarriage, molar pregnancy, and preterm labor.
-
Pelvic Prolapse: This happens when the muscles and tissues supporting the pelvic organs (uterus, bladder, or rectum) become weak or loose.
Remember, a gynae pelvic scan is a diagnostic tool that can help identify these conditions, but it’s just one part of the overall diagnostic process. Further tests may be required for a definitive diagnosis.
A transvaginal scan, also known as a transvaginal ultrasound, is a type of pelvic ultrasound used primarily in gynaecology and early obstetrics. It provides a detailed image of the female reproductive organs, including the uterus, cervix, fallopian tubes, ovaries, and the endometrium (the lining of the uterus).
Unlike a traditional ultrasound, where the transducer (ultrasound probe) is moved across the skin of the abdomen, in a transvaginal scan, a smaller transducer is gently inserted into the vagina. The close proximity of the transducer to these organs allows for more detailed images.
This scan is particularly useful in early pregnancy. It gives a clearer picture of the uterus. It can also detect pregnancy sooner than an abdominal scan. It is also commonly used to investigate gynaecological symptoms, such as unexplained pelvic pain, abnormal bleeding, or unusual discharge. It can also help in diagnosing conditions like ovarian cysts, uterine fibroids, and pelvic inflammatory disease.
The procedure is generally safe and should not be painful, though some women may experience minor discomfort. It’s important to remember that if you’re uncomfortable at any point during the scan, you can ask the sonographer to stop.
HyCoSy, short for Hysterosalpingo-Contrast-Sonography, is a specific type of ultrasound used to assess the fallopian tubes in women, particularly when investigating causes of infertility. It provides a detailed view of whether the fallopian tubes are open or blocked and can also show the inside of the uterus and the surrounding area.
During a HyCoSy, a sterile saline solution and a small quantity of air bubbles are injected into the uterus through a thin tube. The fluid helps to expand the uterine cavity, providing a better view of the uterine lining and the openings to the fallopian tubes. The progress of the fluid and air bubbles can then be followed with ultrasound to see if the fallopian tubes are open.
In contrast, a standard pelvic scan or ultrasound, while it also uses ultrasound technology to create images of the pelvic area, doesn’t involve the injection of fluid or air into the uterus. A pelvic ultrasound can give a general view of the uterus, ovaries, and surrounding structures, but it cannot provide detailed information about the patency (openness) of the fallopian tubes like a HyCoSy can. Therefore, a HyCoSy is a more specialised procedure typically recommended when there’s a specific need to examine the fallopian tubes, such as in cases of unexplained infertility or prior to certain fertility treatments.
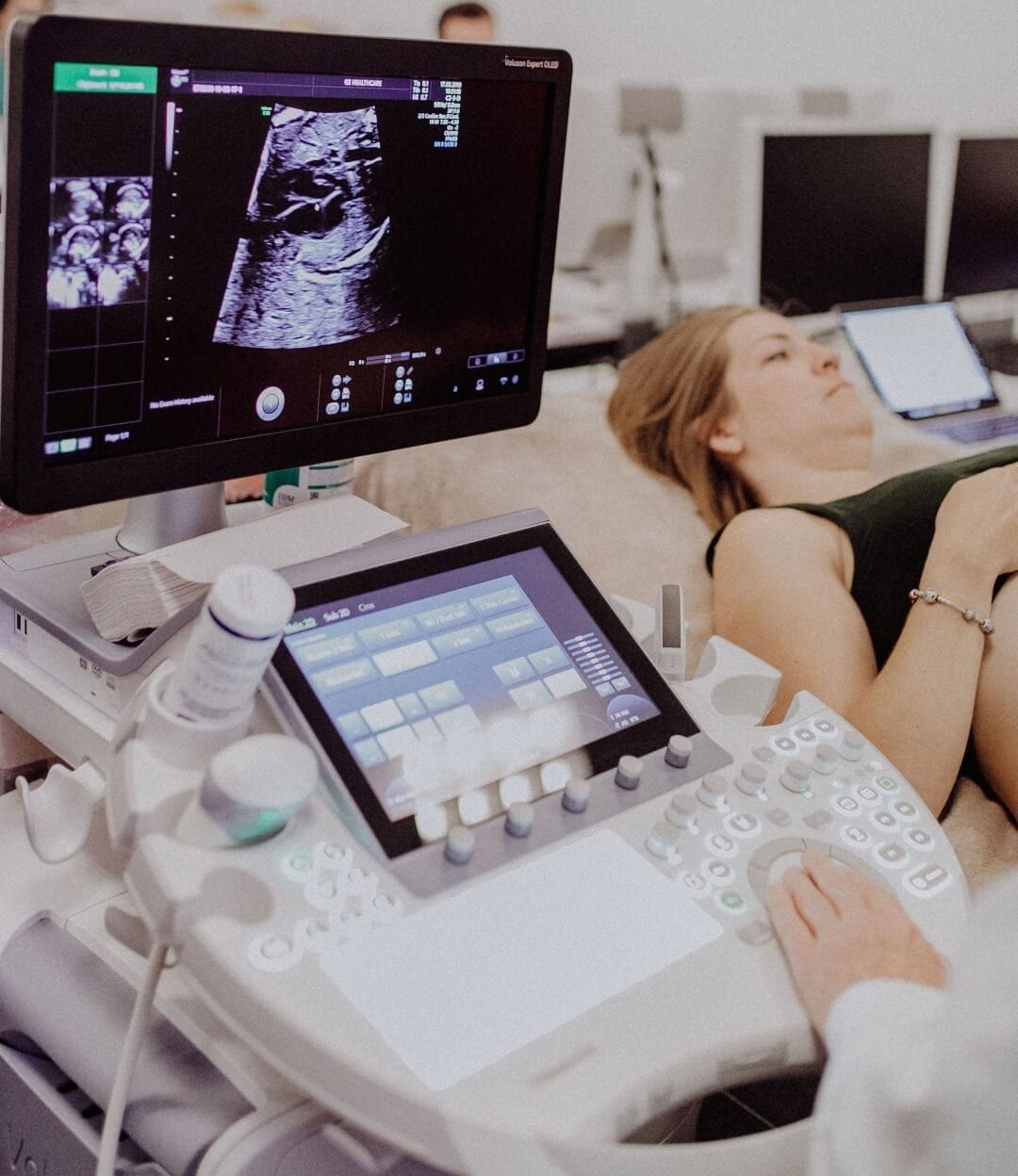
Pelvic Scan at London Pregnancy Clinic
We kindly advise our patients to arrive 10 minutes early for their appointments. Upon arrival, you will be greeted by our friendly admin team at the front desk. You will be asked to fill out a registration form if you have not done so already. We recommend this be completed before your appointment. You will be asked to use our facilities and have an empty bladder for your transvaginal ultrasound scan. During your appointment, you will be provided with a skirt cover to change into. There will be a private and separate area for you to get changed. If you have specific requirements, please ask, and our team will do their best to accommodate.
Shortly after the ultrasound scan is performed, you will receive an email containing your detailed ultrasound report including the images for your referring consultant to review and advise. We can send a copy of your ultrasound report to your referring consultant upon request so that they can receive your results as early as possible. It is possible to share video-clips of your ultrasound scan with you and your consultant if requested in advance.
Transvaginal Ultrasound, also known as internal or endovaginal ultrasound scan, is a safe technique which is routinely performed in Gynaecology to assess the female reproductive organs. This technique is also beneficial in early pregnancy ultrasound examination. Transvaginal ultrasound scans are considered safe when performed by qualified professionals. This is a crucial scan as it provides your clinician with a detailed view of the reproductive organs ensuring the best possible outcome.
The scan is performed using a transvaginal transducer cleaned by using safe and approved medical disinfectant. The transducer is covered with a non-latex probe cover and sterilised gel. The transducer will be inserted into the vagina by your performing operator. There is a need to move the transducer side to side and up and down to obtain satisfactory images.
The procedure is safe and not painful. Please let the clinician know if you are experiencing any discomfort.
Yes, ultrasound is considered safe for medical examinations. Ultrasound uses high-frequency sound waves to produce images of the inside of the body, and it does not use ionising radiation, making it a safe and non-invasive option for many diagnostic tests.
Ultrasound has been widely used in medical practice for several decades and has a well-established safety record. There is no evidence that ultrasound causes any long-term harm to the body.
We will be able to accommodate a large variety of blood test which your referring clinic may as for. For example, a common blood test required in preparation for a fertility treatment is the AMH test, to test the level of anti-müllerian hormone in your blood.
AMH, and many other tests can be done during the same appointment for an additional fee. Visit the link below to find out more about our blood tests.
The best time to do a follicle tracking scan depends on the purpose of the scan.
If you are undergoing fertility treatment, such as in vitro fertilization (IVF), the timing of the scan will depend on your treatment protocol and the medication you are taking. Typically, follicle tracking scans are done starting around day 10-12 of your menstrual cycle and repeated every few days until ovulation is confirmed. This allows your doctor to monitor the growth of follicles in your ovaries and determine the best time for egg retrieval.
If you are using follicle tracking to monitor your menstrual cycle or to track ovulation, the best time to do the scan is around day 12-14 of your cycle. This is when the follicles are typically the largest, and ovulation is most likely to occur in the next 24-48 hours.
Ultimately, the timing of your follicle tracking scan should be determined in consultation with your healthcare provider, who can provide guidance based on your individual circumstances and goals.
Yes, ultrasound is generally considered safe for medical examinations. Ultrasound uses high-frequency sound waves to produce images of the inside of the body, and it does not use ionizing radiation, making it a safe and non-invasive option for many diagnostic tests.
Ultrasound has been widely used in medical practice for several decades and has a well-established safety record. There is no evidence that ultrasound causes any long-term harm to the body.
A pelvic scan is a non-invasive procedure and is generally not painful. During the procedure, a sonographer will insert a small transvaginal ultrasound probe into the vagina to produce images of the ovaries. You may feel some mild discomfort or pressure during this part of the exam, but it should not be painful.
In some cases, you may experience mild cramping or discomfort during the exam, particularly if you have a full bladder. This can happen because a full bladder can push on the uterus, causing discomfort. However, this is usually temporary and subsides once the exam is complete.
If you experience pain during the procedure, it’s important to let the sonographer know right away so they can adjust the procedure or take other steps to minimize your discomfort. In rare cases, women with certain medical conditions or sensitivities may experience more discomfort during the exam, but this is not the norm.
At London Pregnancy Clinic, we are specialists in fertility and reproductive medicine. For a more round picture of your fertility profile, our gynaecologists could recommend other examinations such as AMH test, or our full fertility health assessment package.
A woman’s follicle count depends mainly on genetics and age. Medical conditions and lifestyle factors can also influence this number.
-
Genetics: The number of follicles a woman has is largely determined by her genetic makeup. Women are born with a finite number of follicles, and this number declines over time as follicles are released during ovulation.
-
Age: As women age, the number of follicles in their ovaries naturally decreases. This is because the pool of follicles a woman has at birth is gradually depleted over time. By the time a woman reaches her mid-30s, the number of follicles in her ovaries has typically declined significantly.
-
Medical conditions: Certain medical conditions, such as polycystic ovary syndrome (PCOS), can affect the number of follicles in a woman’s ovaries. Women with PCOS may have a larger number of small follicles in their ovaries, which can affect ovulation and fertility.
-
Lifestyle factors: Lifestyle factors such as smoking, obesity, and exposure to environmental toxins can also affect the number of follicles in a woman’s ovaries. For example, smoking has been linked to decreased ovarian reserve and early menopause.
It’s worth noting that the number of follicles present does not necessarily correlate with fertility or the ability to conceive. Other factors, such as the quality of the eggs and the health of the uterus, also play a role in fertility.
Uterine fibroids, also known as leiomyomas or myomas, are noncancerous growths that develop in or on the muscular walls of the uterus. They vary greatly in size, from tiny growths that are almost undetectable to large masses that can distort and enlarge the uterus. A woman may have a single fibroid or multiple ones.
While fibroids are common, their cause is not clearly understood. It’s believed that multiple factors, such as hormones and genetics, may influence their development. For instance, the hormones estrogen and progesterone, which stimulate the development of the uterine lining during each menstrual cycle, appear to promote the growth of fibroids.
Many women with fibroids don’t have any symptoms. However, those who do may experience symptoms such as heavy or prolonged menstrual periods, abnormal bleeding between periods, pelvic pain or pressure, frequent urination, difficulty emptying the bladder, constipation, or backache or leg pains.
The treatment for uterine fibroids varies depending on their size, location, the severity of symptoms, and whether or not a woman wants to become pregnant in the future. Treatment options can range from watchful waiting (if the fibroids aren’t causing any significant problems) to medication, non-invasive or minimally invasive procedures, or traditional surgical procedures. It’s important to discuss all treatment options with a healthcare provider to make the best decision for individual health needs.
An endometrial polyp, often simply referred to as a uterine polyp, is a tissue growth that develops on the inner lining of the uterus, known as the endometrium. These polyps can range in size from a few millimeters to several centimeters. Typically benign, or noncancerous, endometrial polyps can occasionally become precancerous or cancerous. Symptoms may include irregular menstrual bleeding, bleeding between periods, excessively heavy or long periods, and postmenopausal bleeding. Though they can occur in women of any age, they’re more common during or after menopause. An endometrial polyp can be accurately diagnosed using procedures like hysteroscopy, ultrasound, or a hysterosonography. Prompt diagnosis and treatment of uterine polyps are essential in maintaining optimal female reproductive health.
An ovarian cyst is a fluid-filled sac or pocket that develops in or on an ovary, a part of a woman’s reproductive system. Most ovarian cysts are harmless, often forming during the menstrual cycle, known as functional cysts, and typically disappearing on their own without treatment. However, some cysts can grow large, cause discomfort, and potentially lead to serious complications, such as ovarian torsion or rupture, which requires immediate medical attention. Symptoms of an ovarian cyst can include bloating, abdominal pain, changes in menstrual patterns, or pain during intercourse. Early detection via pelvic examinations and ultrasounds is key to managing ovarian cysts and maintaining optimal reproductive health. Various treatment options, ranging from watchful waiting to surgical removal, are available depending on the size and type of the cyst, symptoms, and the woman’s age.
Pelvic organ prolapse (POP) is a common, often distressing condition where a woman’s pelvic organs – such as the bladder, uterus, or rectum – descend into or protrude out of the vagina due to weakened or stretched pelvic floor muscles and ligaments. Factors contributing to pelvic prolapse can include childbirth, menopause, aging, chronic constipation, and heavy lifting. Symptoms vary but can encompass a feeling of pressure or fullness in the pelvic area, discomfort or pain during sexual intercourse, urinary or bowel issues, and visible bulging from the vagina. While not life-threatening, pelvic organ prolapse can significantly impact a woman’s quality of life. Various treatments are available, ranging from pelvic floor exercises and pessary devices to surgical intervention, ensuring tailored management for each individual’s needs. Early diagnosis, achievable through routine gynecological exams, can aid in managing symptoms and potentially prevent progression.
Endometriosis is a prevalent and often painful disorder where tissue similar to the endometrium, the lining of the uterus, grows outside the uterine cavity, typically affecting the ovaries, fallopian tubes, and the tissue lining the pelvis. This misplaced tissue continues to act as it would inside the uterus – thickening, breaking down, and bleeding with each menstrual cycle. With no exit path for this displaced tissue, it becomes trapped, leading to symptoms like pelvic pain, heavy periods, and potential fertility issues. Though a challenging condition to diagnose due to its wide array of symptoms, methods such as pelvic exams, ultrasounds, or laparoscopy can help confirm endometriosis. Treatment options vary from hormonal therapies and pain management to surgical intervention. Understanding endometriosis is crucial to improving the quality of life for many women of reproductive age worldwide.
Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder among women of reproductive age, characterised by prolonged or infrequent menstrual periods and higher levels of male hormones (androgens). Women with PCOS may develop numerous small collections of fluid (follicles) in their ovaries, potentially leading to failure in regularly releasing eggs. Symptoms can include menstrual irregularities, excess hair growth, acne, weight gain, and difficulties with fertility. While the exact cause remains unknown, factors like insulin resistance and inflammation appear to play key roles. Early diagnosis through ultrasound imaging and blood tests can aid in managing symptoms and preventing long-term health issues, like type 2 diabetes and heart disease. Treatment strategies for PCOS often focus on lifestyle modifications, hormonal therapies, and fertility treatments, as needed. Raising awareness about PCOS is crucial to ensure early detection and improved health outcomes for affected women.
Pelvic Inflammatory Disease (PID) is an infection of a woman’s reproductive organs, typically caused by sexually transmitted bacteria. It often affects the uterus, fallopian tubes, and ovaries, causing inflammation and potential fertility complications. Early symptoms can be subtle, but can escalate to pelvic pain, fever, irregular menstrual bleeding, and painful urination. If left untreated, PID can lead to long-term problems like chronic pelvic pain, ectopic pregnancy, and infertility. PID is often preventable through safe sexual practices and regular screenings for sexually transmitted infections. Early detection through clinical examinations and tests is crucial for effective treatment, which typically involves antibiotics. Understanding and spreading awareness about Pelvic Inflammatory Disease is essential in promoting women’s reproductive health and preventing serious complications.
DO YOU WANT TO KNOW MORE ABOUT OUR FOLLICLCE TRACKING SCAN?


