UNITY NIPT
UNITY is the principal new concept of NIPT because it can screen not only for Down’s syndrome but also for severe genetic diseases. What sets UNITY apart is its exclusive molecular counting technology, which enhances the precision of the test and has a low no-call rate.
The basic UNITY Aneuploidy Screen is accurate for trisomies 21, 18 and 13. The advanced version of the test is called UNITY Complete and screens for various severe genetic disorders.
We are proud to be the first clinic in London to offer the UNITY test in the UK.
UNITY is a new and advanced NIPT from 10 weeks
At London Pregnancy Clinic, we offer only state-of-the-art technology and genetic tests. UNITY is a new participant in the NIPT market, offering a blend of cutting-edge genomic technology and competitive pricing.
Depending on the UNITY panel you choose it can screen for important single-gene disorders: cystic fibrosis (CF), spinal muscular atrophy (SMA). sickle cell disease (SCD), alpha- and beta-hemoglobinopathies (thalassemias).
UNITY is the best option for Rh-negative expectant mothers.
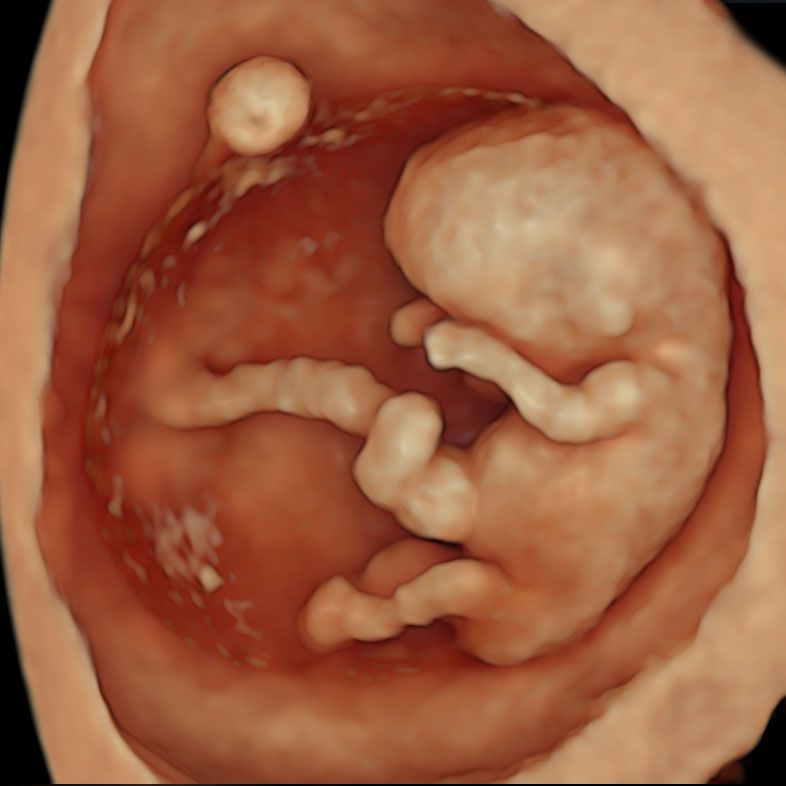
NIPT is best done in conjunction the 10 Week Scan
UNITY NIPT at London Pregnancy Clinic
-
UNITY Aneuploidy Screen is highly accurate in detecting Down’s (trisomy 21), Edwards (trisomy 18), and Patau (trisomy 13) syndromes
-
UNITY screening performance is similar to other advanced tests: PrenatalSafe and Panorama and is much better than the outdated Harmony Test
-
UNITY is the best cost-effective option for essential chromosomal screening
-
UNITY can determine the fetal Rh blood group for Rh-negative mothers, with only a small additional cost (+£50)
-
Optional Gender Reveal included in the price
-
The UNITY Aneuploidy Screen includes free accurate screening for sex chromosome anomalies like Turner syndrome and Klinefelter syndrome
-
Turnaround time of up to 10 working days (Lab is US based)
UNITY extended NIPT Explained
For expectant mothers with Rh-negative blood groups, UNITY Aneuploidy Screen offers a distinctive advantage by providing the capability to identify the fetal Rh blood group as early as 10 weeks into pregnancy, for a small additional charge. This information is highly significant because it helps determine whether the mother requires an Anti-D injection, which is a preventive treatment.
In Rh-negative mothers carrying an Rh-positive fetus, there’s a risk that fetal blood cells can enter the mother’s bloodstream during pregnancy or childbirth, potentially leading to sensitization. This means that the mother’s immune system might produce antibodies against the Rh antigen. These antibodies could pose a risk to future pregnancies with Rh-positive babies, potentially causing hemolytic disease of the newborn (HDN), which can have serious consequences for the baby.
UNITY’s unique offering of early Rh blood group identification empowers Rh-negative mothers with timely knowledge. If the fetus is Rh-positive, the mother can receive the necessary Anti-D injection to prevent sensitization. This preventive measure is crucial for ensuring the health and well-being of both the current and future pregnancies, making UNITY a particularly valuable choice for Rh-negative mothers seeking to protect their baby’s health and their own.
UNITY Complete is an extended NIPT option that consists of an essential UNITY aneuploidy screen (T21, T18, T13) and UNITY Carrier Screen.
UNITY Carrier Screen looks for Important Inherited Genetic Disorders.
Screening for genetic disorders can be added to the advanced chromosomal screening provided by UNITY for an additional cost and called “UNITY Complete”. This comprehensive screening option combines the assessment of chromosomal abnormalities with the screening for genetic disorders.
You can book UNITY Complete with London Pregnancy Clinic for £990 (£730 for the NIPT + £260 for the scan). Note that you will not be able to do UNITY Complete without our ultrasound scan.
Chromosomal Anomalies:
- Down’s syndrome (trisomy 21)
- Edwards syndrome (trisomy 18)
- Patau syndrome (trisomy 13)
- Sex chromosome aneuploidies (SCA)
Inherited Genetic Diseases:
- Cystic fibrosis (CF)
- Spinal muscular atrophy (SMA)
- Sickle cell disease (SCD)
- Alpha thalassemia
- Beta thalassemia
Sex of the fetus (optional)
Fetal Rh blood group status
Cystic fibrosis (CF) is a genetic disorder primarily affecting the lungs and digestive system. It results from a faulty gene called the cystic fibrosis transmembrane conductance regulator (CFTR) gene. This gene mutation leads to the production of thick, sticky mucus that can clog the airways in the lungs and obstruct the pancreas, impairing digestion and nutrient absorption. CF can cause a range of severe symptoms, including chronic cough, lung infections, difficulty breathing, poor growth, and digestive problems.
While the National Health Service (NHS) offers a national screening program for CF, it typically occurs after birth, which means that a baby is already born with the genetic disease before it is diagnosed. On the other hand, UNITY provides an opportunity for prenatal screening, allowing parents to gain crucial insights into their baby’s health during pregnancy. This early detection can help parents and healthcare providers prepare for the baby’s arrival and provide specialized care and treatment if the screening indicates that the child may have CF. By offering prenatal screening for CF, UNITY empowers parents with valuable information that can be vital for the well-being of their child.
Fetal screening for Sickle Cell Disease (SCD) is crucial for early detection of this genetic condition. This early identification enables expectant parents to prepare for their child’s specific medical needs. Informed by this knowledge, families can make educated decisions about healthcare and management strategies from birth.
Recently, advancements in prenatal testing have introduced a significant development: the UNITY test. This non-invasive single-gene NIPT offers a safe method for assessing the probability of SCD in the fetus. It marks an important step forward in prenatal care, providing accurate screening results without the risks associated with invasive procedures like amniocentesis and chorionic villus sampling.
For healthcare professionals, this information is vital in planning and providing specialized care immediately after birth, reducing the risk of SCD-related complications. Moreover, understanding the genetic implications of fetal screening is invaluable for parents. It assists in understanding the hereditary nature of SCD and guides future family planning decisions, emphasizing the importance of genetic counselling.
In essence, fetal screening for Sickle Cell Disease, particularly with the advent of the UNITY test, is a proactive approach to ensuring the best possible care and support for the child and family. It highlights the significance of early intervention and ongoing care in managing genetic conditions.
For more details on fetal SCD screening and to discuss the most suitable options for your pregnancy, we recommend consulting with us before booking the UNITY test.
Screening for Thalassemias, a group of inherited blood disorders, is an essential part of prenatal care. Thalassemias affect haemoglobin production, leading to anaemia and other health issues. Early identification through fetal screening enables expectant parents to understand their child’s potential medical needs and plan for appropriate care and treatment.
The introduction of the UNITY test, a non-invasive single gene NIPT (Non-Invasive Prenatal Testing), marks a significant advancement in prenatal screening. While UNITY is not diagnostic, it provides accurate probabilities of the fetus being affected by Thalassemias. This information is crucial for expectant parents and healthcare providers, as it offers a safer alternative to invasive procedures like amniocentesis, minimising risks to both the mother and fetus.
Early detection through screening methods like UNITY is vital. It informs parents about the likelihood of their child having Thalassemia, allowing them to prepare for treatments such as blood transfusions or bone marrow transplants if needed. This knowledge also aids in understanding the genetic risks and implications, guiding future family planning decisions and underscoring the importance of genetic counselling.
For healthcare professionals, screening results help create a comprehensive care plan tailored to the child’s needs. This could include managing symptoms of anaemia and preventive strategies for complications associated with Thalassemias, like iron overload from blood transfusions.
In essence, fetal screening for Thalassemias, particularly with methods like the UNITY test, is a proactive approach in prenatal care. It emphasises the significance of early detection, informed decision-making, and continuous care in managing genetic blood disorders.
Expectant parents seeking more information on fetal screening for Thalassemias, including the implications of UNITY test results, should consult their healthcare provider for the most suitable options and guidance.
10 weeks is the best time for your UNITY because:
- You prefer to be reassured regarding fetal genetic conditions as early as possible
- We perform your earliest fetal structural anomaly scan at 10 weeks, which will exclude severe not-chromosomal defects
- In case of no-call NIPT results of the test, you have plenty of time to retake the test
- In case of high-chance NIPT results, you can perform CVS (invasive test) to confirm or exclude the chromosomal problem at the earliest possibility
Our dedicated Fetal Medicine doctor or Specialist Sonographer will start by conducting a thorough anatomical examination of the baby to check for structural anomalies and gather essential measurements required for the UNITY test.
Once our clinician confirms that the baby’s structural examination is normal, they will proceed to discuss the UNITY test with you, addressing any questions or concerns you may have.
Following this consultation, our friendly phlebotomist will collect a blood sample, which typically involves three blood tubes, from the mother’s arm. This process is akin to any routine blood test you might have undergone elsewhere.
Our staff will then carefully process these blood samples and promptly send them to the lab, which is located in California US. After your appointment, all that remains is to await our call with the test results!
We provide complimentary pre-NIPT counselling during our viability scans because we understand that the array of NIPT options, especially advanced ones like UNITY Complete, can be overwhelming. It’s essential to make an informed choice, and we respect that you may need time to consider your options.
During your viability scan, once we confirm the normal development of your pregnancy, we’ll take the time to explain the workings of various non-invasive prenatal tests. This way, you can make a confident and well-informed decision about which test aligns best with your needs and preferences.
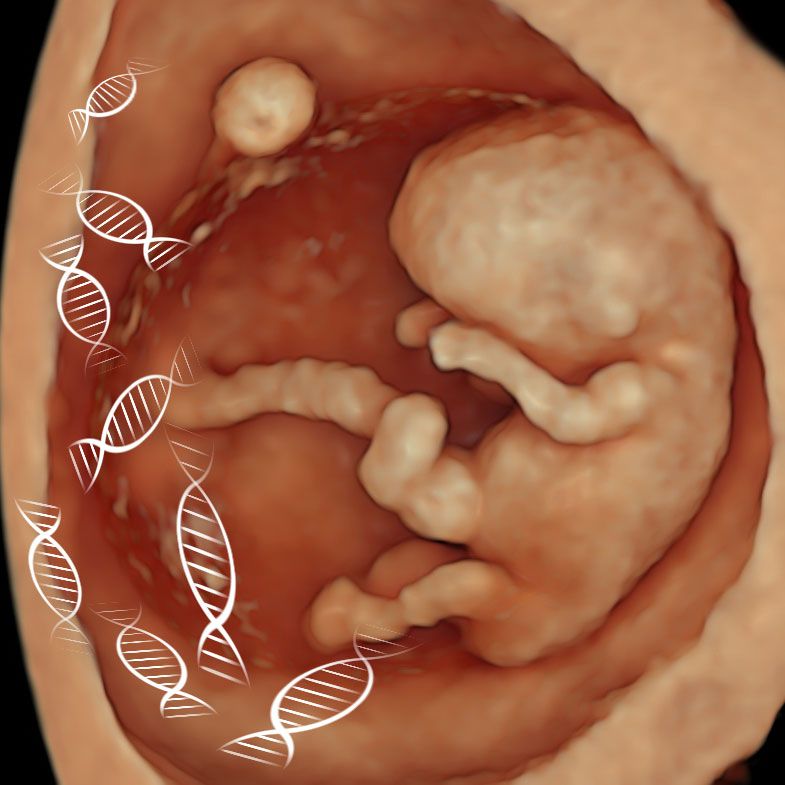
Our NIPT + Early Anomaly Scan always incorporates chromosomal anomaly and structural screening from as early as 10 weeks
Your NIPT options – Comparison Table
Cheapest NIPT
Cheapest NIPT
Unity NIPT
Basic Extended
Basic Extended
Panorama AI
Most Advanced NIPT
Comprehensive
Smart Test – Knova®
As early as…
Turnaround (working days)
Lab Location
No Call Results/Redraw Rates
Down, Edwards, & Patau Syndrome
Turner Syndrome (45x)
Sex Chromosomes Aneuploidies
Di George Syndrome (22q Del)
Triploidy
Additional Chromosomes
Microdeletions
De Novo Genetic Syndromes
Twin Pregnancies
Vanishing twin syndrome
Donor Eggs/Surrogacy
Early Anomaly Ultrasound Screening
Fetal Sex Reveal (Optional)
Scan & NIPT Price
General Notes:
The data taken from the clinical data published by EuroFins, Billion To One and Natera.
* Panorama AI for Di George Syndrome was validated in SMART, the largest prospective NIPT study (2022), combining artificial intelligence (AI) with Natera’s proprietary SNP-based methodology to improve both accuracy and the positive predictive value (PPV) for 22q deletions. The data from this study showed 83-99.9% sensitivity, 53% positive predictive value (PPV) and just 0.05% false positive rate.
** Triploidy, Turner Syndrome (45X) and sex chromosome aneuploidy NIPT screening has limited clinical validation data. It can have higher false positive rate and also inconclusive results. The positive or inconclusive results of the tests may be NOT covered by NHS and you may require private genetic counselling and possible private invasive test (CVS or amniocentesis) for your own expense.
*** Panorama Al with Microdeletion Panel add-on options. Please get in touch to enquire.
There are three compelling reasons to opt for UNITY over PrenatalSafe:
1. Cost Efficiency: UNITY Aneuploidy Screen comes at a significantly lower price point, saving you £50 compared to Prenatalsafe, all while delivering equally accurate results for detecting Down syndrome. This affordability is made possible by UNITY’s competitive pricing strategy as a newcomer in the market.
2. Comprehensive Information: For Rh-negative mothers, Unity Rh (available at an additional cost) offers the valuable capability to identify the Rh blood group of the fetus. This information is crucial in managing potential Rh sensitization issues during pregnancy.
3. Advanced Genetic Screening: UNITY Carrier Screen (also available at an additional cost) employs sgNIPT Reflex technology, a cutting-edge non-invasive prenatal testing method utilizing a unique molecular counting approach. What sets it apart is its ability to screen for a wide range of genetic disorders, including cystic fibrosis (CF), spinal muscular atrophy (SMA), sickle cell disease (SCD), and other fetal red cell genetic disorders. Detecting these conditions early can be vital, as some may offer treatment options after birth.
BillionToOne Inc., the biotechnology company that offers UNITY NIPT services, is headquartered in California, USA. As a result, there is a shipping period necessary when sending your blood sample internationally. Typically, you can anticipate a turnaround time of up to 2 weeks for UNITY Down’s syndrome NIPT results and an additional 2-week wait for UNITY Carrier Screen results.
We highly recommend undergoing the NIPT in conjunction with our comprehensive early anomaly scan, known as the 10 Weeks Scan, as early as possible, ideally just after the 10-week mark. Detecting chromosomal, genetic or structural anomalies at this early stage allows for more extensive options in terms of managing any identified conditions. In the event that your initial sample fails, this early timing ensures ample opportunity for a redraw without causing delays.
BillionToOne Inc, the provider of our UNITY NIPT services, is based in California, USA. Consequently, a shipping period is involved in sending your blood sample internationally. Typically, the turnaround time for UNITY Down’s syndrome NIPT results is up to 2 weeks, and for UNITY Carrier Screen results, you can expect an additional 2-week wait.
If you are uncertain about the precise gestational age of your pregnancy, we strongly recommend undergoing a Viability Scan with us at approximately 7-8 weeks into your pregnancy. This scan will accurately date your pregnancy, allowing us to arrange the earliest possible appointment for your NIPT. Any inquiries or concerns regarding UNITY or other NIPT options can be addressed after the Viability Scan.
However, if you prefer not to have a Viability Scan, please allow a few days beyond the 10-week mark before scheduling your NIPT appointment. This will help avoid the need for repeat blood draws. It’s important to note that delaying beyond this timeframe may result in missing the advantages of the 10 Weeks Scan, as the baby may still be too young for a proper early anomaly scan.
In theory, UNITY NIPT is available from 10 to 40 weeks of pregnancy, but we strongly recommend taking the test in the first trimester. This is because pregnancy management options become significantly limited in the second trimester, making early detection and intervention crucial for informed decision-making.
UNITY Carrier Screen stands out from most other carrier screening tests by incorporating screening for certain single-gene conditions like cystic fibrosis, SMA (spinal muscular atrophy), and sickle cell disease. Here’s how it works:
1. Carrier Screening: UNITY Carrier Screen begins with carrier screening on the mother’s DNA. Carrier screening is a test that looks for specific genetic mutations associated with these conditions in the mother’s DNA. If the screening identifies a mutation in the mother’s genes, it means she is a carrier for that condition.
2. Testing the Fetal cfDNA: If the mother is found to be a carrier for one or more of these conditions, UNITY Carrier Screen then examines the fetal DNA to answer two key questions:
a. Does the Baby Have the Same Mutation as the Mother?: UNITY checks if the baby inherited the same genetic mutation from the mother, which is necessary for the condition to be present in the baby.
b. Does the Baby Have Another Mutation on the Other Copy of the Gene?: For these conditions to manifest, two copies of the mutated gene are usually required—one from each parent. UNITY Carrier Screen also checks if the baby has a mutation on the other copy of the gene (which would typically come from the father’s side).
UNITY Carrier Screen streamlines this process by conducting carrier screening directly on the mother’s DNA. This approach eliminates the need for the biological father to undergo carrier screening—a step that often gets missed in routine testing. If the mother’s UNITY Carrier Screen results are negative (meaning no mutations were found in her genes for these conditions), then the fetal DNA screening for these single-gene conditions is typically not performed. This is because the baby is at a lower risk for these conditions if the mother is not a carrier. In essence, UNITY Carrier Screen offers a comprehensive and efficient approach to screening for these single-gene conditions, ensuring that critical information is obtained even when the biological father’s participation in testing is uncertain or unavailable.
The UNITY Aneuploidy Screen for Down’s syndrome includes free accurate screening for sex chromosome anomalies like Turner syndrome and Klinefelter syndrome. Screening for those conditions is a common practice in the US and many other countries. However, it is important to know that the NHS screening program in the UK does not support routine check for these conditions and screening for sex chromosome anomalies outside of the NHS program may result in unexpected costs for private genetic counselling and diagnostic testing.
After your scan appointment, you will receive a comprehensive scan report from our team of doctors and sonographers. This report will be provided to you in both hard copy format and as a PDF document sent securely through our cloud-based system, Tricefy.
Once we have received the results of your UNITY NIPT test from the laboratory, our experienced clinician will review the findings and officially approve them. Subsequently, one of our warm and knowledgeable clinical staff members will reach out to you via phone to provide an interpretation of the test results. Following this discussion, we will promptly send you an electronic copy of the test results via the Tricefy platform for your convenience.
If your UNITY Carrier Screen NIPT result indicates a high chance for a genetic syndrome, such as cystic fibrosis, our medical team will promptly get in touch with you. During this communication, our doctor will provide detailed explanations of the next steps and recommendations for your specific situation.
In most cases, we will likely arrange a referral to a private geneticist. Please note that the consultation cost with the geneticist is not included in our service. The geneticist will offer expert guidance, counseling, and further evaluation options.
Additionally, we may recommend reaching out to your local NHS Fetal Medicine Unit for additional counseling and possible diagnostic tests like Chorionic Villus Sampling (CVS) or amniocentesis. These diagnostic procedures can provide more definitive information about the genetic condition in question.
Alternatively, we can assist in referring you to a private Fetal Medicine Consultant, though it’s important to note that the consultation cost with the consultant is also not included in our service. This approach allows you to explore alternative avenues for comprehensive assessment and guidance regarding the genetic syndrome. Our priority is to ensure you receive the necessary support and information to make informed decisions about your pregnancy and the health of your baby.
It’s crucial to recognize that extended NIPT screenings for rare genetic diseases, such as the one offered by UNITY, encounter specific challenges related to the validation of these conditions. The main challenge stems from the fact that these genetic disorders are exceptionally rare in the population. As a result, obtaining a large enough sample size for rigorous validation can be difficult.
While UNITY’s test is undoubtedly advanced and utilizes cutting-edge technology, it’s important to acknowledge that it may not possess extensive validation data for all the rare genetic disorders it screens for. Validation data typically involves a substantial number of confirmed cases to establish the test’s accuracy and reliability in identifying these specific conditions. With rare disorders, there may simply not be a sufficient number of cases available for comprehensive validation.
In practical terms, this means that while the test can provide valuable insights and potentially detect a range of rare genetic disorders, it may not have the same level of certainty or accuracy as it does for more common conditions (Down’s syndrome).
An additional factor is the genetic variation of the mutations. For example, the current version of UNITY cannot detect 1-3% of cystic fibrosis (CF) cases due to the presence of rare unknown non-F508del mutations.
The performance data for the UNITY Carrier Screen NIPT can be interpreted based on the threshold used for the calculations. In this case, the threshold being discussed is set at 1 in 4 (high risk). Let’s break down what these performance metrics mean:
1. PPV (Positive Predictive Value): PPV indicates the probability that a positive test result accurately reflects the presence of the condition being tested for. In this context, with a threshold of 1 in 4 (high risk), the PPV is 79.3%. This means that if the test identifies a high-risk result (1 in 4 or higher), there is a 79.3% probability that the identified risk is genuine.
2. Specificity: Specificity measures the test’s ability to correctly identify individuals who do not have the condition (true negatives). At a threshold of 1 in 4, the specificity is 98.9%. This indicates that the test is very good at correctly identifying cases where the condition is not present.
3. NPV (Negative Predictive Value): NPV represents the probability that a negative test result accurately reflects the absence of the condition. With a threshold of 1 in 4 (high risk), the NPV is 99.6%. This means that if the test returns a negative result (below 1 in 4), there is a 99.6% probability that the absence of the condition is genuine.
4. Sensitivity: Sensitivity measures the test’s ability to correctly identify individuals who have the condition (true positives). At a threshold of 1 in 4, the sensitivity is 92.0%. This suggests that the test is effective at identifying cases where the condition is genuinely present.
In summary, when the UNITY Carrier Screen NIPT is evaluated with a high-risk threshold of 1 in 4, it demonstrates a reasonably high PPV, indicating that positive results are often accurate. The test also exhibits excellent specificity and NPV, meaning that it effectively rules out the condition when it is not present. Additionally, the sensitivity is at a good level, indicating its ability to detect cases with the condition.
It’s important to note that the choice of threshold can impact the performance metrics, and these values are specific to the selected threshold of 1 in 4. Different thresholds may yield different performance outcomes, and healthcare providers often consider the specific clinical context and risk factors when interpreting test results.
Reference:
Wynn J, Hoskovec J, Carter RD, Ross MJ, Perni SC. Performance of single‐gene noninvasive prenatal testing for autosomal recessive conditions in a general population setting. Prenat Diagn. 2023;1‐11
Vanishing twin is a situation with twin pregnancies when the embryo or fetus in one of the sacs fails to develop or dies at the early stages of pregnancy. Interpretation of NIPT in the case of the vanishing twin phenomenon is complicated due to contamination of the sample by DNA of non-developing twin pregnancy.
UNITY aneuploidy screen can be used in the cases of the vanishing twin phenomenon. Please get in touch to enquire.
Unity Carrier Screen can diagnose cystic fibrosis in the fetus as early as at 10 weeks.
Cystic fibrosis (CF) is a genetic disorder primarily affecting the respiratory, digestive, and reproductive systems. It is a hereditary condition caused by mutations in the CFTR gene, which encodes a protein responsible for regulating the movement of salt and water in and out of cells.
Here are critical points about cystic fibrosis:
- Incidence at birth: 1 in 5000 for the general population, 1 in 2500 for Northern Europeans.
- Carrier rate: 1 in 45 for the general population, 1 in 24 for Northern Europeans.
- Genetic Basis: CF is an autosomal recessive genetic disorder, meaning that a child must inherit two defective CFTR genes (one from each parent) to develop the condition. Individuals who inherit only one mutated gene are carriers but do not have CF.
- Respiratory System: CF primarily impacts the respiratory system by causing thick and sticky mucus to accumulate in the airways. This can lead to chronic lung infections, difficulty breathing, and progressive lung damage.
- Digestive System: CF can affect the digestive system by impairing the secretion of digestive enzymes, leading to malabsorption of nutrients and poor growth in children. It can also lead to problems like pancreatic insufficiency and liver disease.
- Sweat Glands: People with CF often have elevated levels of salt in their sweat, which is used as a diagnostic test for the condition.
- Symptoms: CF symptoms can vary in severity but may include persistent coughing, wheezing, salty-tasting skin, poor growth, frequent lung infections, digestive problems, and infertility in males.
- Treatment: CF is a chronic condition, and there is no cure. However, advances in medical care have greatly improved the quality of life and life expectancy for individuals with CF. Treatment typically involves a combination of therapies, including airway clearance techniques, medications, nutritional support, and lung transplantation in severe cases.
- Life Expectancy: The life expectancy of individuals with CF has increased significantly over the years, and many individuals with CF now live into adulthood. The median predicted survival age in some countries is in the 40s or even higher.
Unity Carrier Screen provides an opportunity for early diagnosis, crucial for managing CF effectively and improving outcomes. Carrier screening and genetic counselling can help identify individuals at risk of passing on CF to their children and provide information for family planning decisions.
Unity Carrier Screen can diagnose spinal muscular atrophy in the fetus as early as 10 weeks in pregnancy.
Spinal muscular atrophy (SMA) is a genetic disorder that affects the motor neurons in the spinal cord and leads to muscle weakness and atrophy (wasting). SMA is primarily caused by mutations in the SMN1 gene, which plays a crucial role in the survival of motor neurons. This condition can vary in severity, with different types of SMA affecting individuals in different ways.
Here are critical points about spinal muscular atrophy (SMA):
- Incidence at birth: 1 in 6000-10000 for the general population.
- Carrier rate: 1 in 54 for the general population.
- Genetic Basis: SMA is an autosomal recessive genetic disorder, meaning that a child must inherit two defective SMN1 genes (one from each parent) to develop the condition. Individuals with one normal and one mutated SMN1 gene are carriers and do not have SMA.
- Motor Neuron Degeneration: SMA primarily affects motor neurons, the nerve cells responsible for controlling muscle movement. The loss of motor neurons leads to muscle weakness and atrophy over time.
- Types of SMA: SMA is classified into different types based on the age of onset and severity of symptoms. The most severe form, known as infantile-onset SMA (Type 1), typically presents in infancy and can lead to significant motor impairment. Types 2, 3, and 4 have later onset and varying degrees of motor weakness.
- Symptoms: Symptoms of SMA may include muscle weakness, difficulty with motor tasks like crawling or walking, respiratory difficulties, and, in severe cases, problems with swallowing and breathing.
- Treatment: Although there is no cure for SMA, there are treatment options available that can help manage the condition. These may include physical therapy, occupational therapy, assistive devices, and, in recent years, disease-modifying therapies like gene therapy and medications.
- Genetic Testing: Early diagnosis of SMA through genetic testing is essential for initiating treatment and supportive care as early as possible. Genetic testing can identify carriers and individuals affected by SMA.
- Life Expectancy: The life expectancy and prognosis for individuals with SMA can vary widely depending on the type and severity of the condition. Advances in medical care and therapies have led to improved outcomes, and some individuals with SMA are now able to live longer and more fulfilling lives.
- Family Planning: Carrier screening and genetic counselling are essential for individuals at risk of carrying the SMA gene mutation. This information can inform family planning decisions and help individuals understand their risk of passing on SMA to their children.
SMA is a genetic disorder affecting muscle function due to the loss of motor neurons. Early diagnosis, supportive care, and emerging treatments have improved the outlook for individuals with SMA, highlighting the importance of genetic testing and counselling for at-risk individuals and families.
Unity Carrier Screen can diagnose sickle cell anaemia in the fetus as early as at 10 weeks of pregnancy.
Sickle cell anaemia (SCA) is a genetic disorder characterized by the abnormal shape of red blood cells. This condition is caused by HBB gene mutations, which provide instructions for making a protein called haemoglobin. Haemoglobin is responsible for carrying oxygen in the blood.
Here are critical points about sickle cell anaemia:
- Incidence at birth: Sickle cell disease occurs predominantly in people of African and African-Caribbean origin, with incidence at birth 1 in 256. Generally, sickle cell disease is estimated to affect 1 in every 2000 live births in England.
- Carrier rate: 1 in 8 in people of African and African-Caribbean origin.
- Genetic Basis: Sickle cell anaemia is an autosomal recessive genetic disorder. To develop the condition, a person must inherit two mutated HBB genes, one from each parent. Individuals who inherit only one mutated gene are carriers, often referred to as having sickle cell trait, and typically do not display symptoms of the disease.
- Red Blood Cell Abnormalities: In sickle cell anaemia, the haemoglobin protein is altered, causing red blood cells to take on a rigid, sickle-like shape when they lose oxygen. These abnormal cells can become trapped in blood vessels, leading to pain, organ damage, and decreased oxygen delivery to tissues.
- Symptoms: Common symptoms of sickle cell anaemia include chronic pain, fatigue, jaundice (yellowing of the skin and eyes), anemia (a shortage of red blood cells), and an increased risk of infections.
- Complications: Sickle cell anaemia can result in a range of complications, including acute pain crises, organ damage (especially to the spleen, lungs, and kidneys), stroke, acute chest syndrome, and delayed growth in children.
- Treatment: While there is no cure for sickle cell anaemia, various treatments are available to manage symptoms and prevent complications. These treatments may include pain management, blood transfusions, medications to reduce the frequency of pain crises, and hydroxyurea, which can help increase the production of fetal haemoglobin.
- Lifespan: The lifespan of individuals with sickle cell anaemia has improved significantly over the years due to medical care and treatment advances. With appropriate management and care, many individuals with the condition can lead relatively normal lives.
- Genetic Counseling: Carrier screening and genetic counselling are essential for individuals at risk of having children with sickle cell anaemia. Knowing one’s carrier status and genetic risk is crucial for family planning decisions.
Early diagnosis, proactive medical care, and a supportive healthcare team can help individuals with sickle cell anaemia manage their condition effectively and enjoy a good quality of life.
UNITY Carrier Screen:
Pros:
- Efficiency: UNITY Carrier Screen offers efficient carrier screening by initially checking the mother’s DNA. It eliminates the need for the biological father’s participation in testing, which can sometimes be challenging to arrange.
- Convenience: This approach simplifies the screening process for couples, as it doesn’t require additional testing from the father. It can save time and resources.
- Comprehensive: UNITY Carrier Screen incorporates screening for various single-gene conditions like cystic fibrosis, spinal muscular atrophy (SMA), and sickle cell disease. This broadens the scope of carrier screening.
- Early Information: It provides information about the baby’s risk for these conditions during pregnancy, allowing parents to make informed decisions and plan accordingly.
Cons:
- Not Diagnostic: UNITY Carrier Screen is a screening test, not a diagnostic test. While it assesses the risk, it cannot guarantee that the baby will have or not have the condition.
- It can include additional costs. You may need to have private genetic counselling if the results are a high chance.
NHS Carrier Screening:
Pros:
- Targeted: Government-sponsored carrier screening programs in the UK focus on specific genetic conditions that are prevalent among certain ethnic groups. This targeted approach aims to reduce the impact of these conditions on public health.
- Genetic Counseling: These programs often include genetic counselling, which provides individuals and couples with comprehensive information and support regarding their risks and family planning decisions.
- Population-Wide: In the UK, carrier screening programs can reach a wide population, ensuring that those at higher risk due to ethnicity or family history receive appropriate testing and guidance.
Cons:
- Postnatal: In many cases, the results of government-sponsored carrier screening are available postnatally, meaning the baby is already born when the diagnosis is made.
- Dependent on Risk Factors: UK government-based screening programs primarily target high-risk populations. If you do not belong to these high-risk groups or have specific risk factors, you may not receive comprehensive carrier screening.
- May Require Father’s Participation: In some cases, government-based programs may require the biological father to undergo testing, which can be logistically challenging if he is unavailable or unwilling to participate.
- Limited Scope: These programs may not cover as broad a range of genetic conditions as UNITY Carrier Screen. Coverage varies based on the condition’s prevalence in specific ethnic groups.
In summary, UNITY Carrier Screen offers an efficient and comprehensive approach to carrier screening by initially testing the mother’s DNA. This can be advantageous when the biological father’s participation is uncertain. On the other hand, NHS screening programs target high-risk populations and often include genetic counselling.
At London Pregnancy Clinic, we require a scan before any NIPT test. This is to confirm that your pregnancy is viable, progressing normally, and at the correct gestational age. We believe this step provides vital reassurance before proceeding with testing.
With our partner Jeen Health, you do not need to have a scan at the same appointment. However, you will need to provide proof of a recent pregnancy scan within the last 7 days before the blood sample is taken. This ensures accuracy and safety while still offering flexibility for patients across the UK.


