.el-element { padding:15px 15px 0 15px; }
What is Patau Syndrome? Key Information for Expecting Parents
Patau syndrome, also known as trisomy 13, is a rare chromosomal condition caused by an extra copy of chromosome 13. This additional genetic material disrupts normal fetal development. It leads to serious physical and intellectual disabilities. The condition affects multiple organ systems and unfortunately carries a poor prognosis. Most affected babies do not survive beyond their first year of life.
During pregnancy, Patau syndrome can be detected through routine NHS screening programmes and specialised diagnostic tests. Early detection through anomaly scans and non-invasive prenatal testing (NIPT) allows families to make informed decisions about their pregnancy. Genetic counselling services provide essential support and information about the condition, helping expectant parents understand their options and access appropriate screening tests throughout their pregnancy journey.
For more detailed information, visit our dedicated Patau Syndrome page.
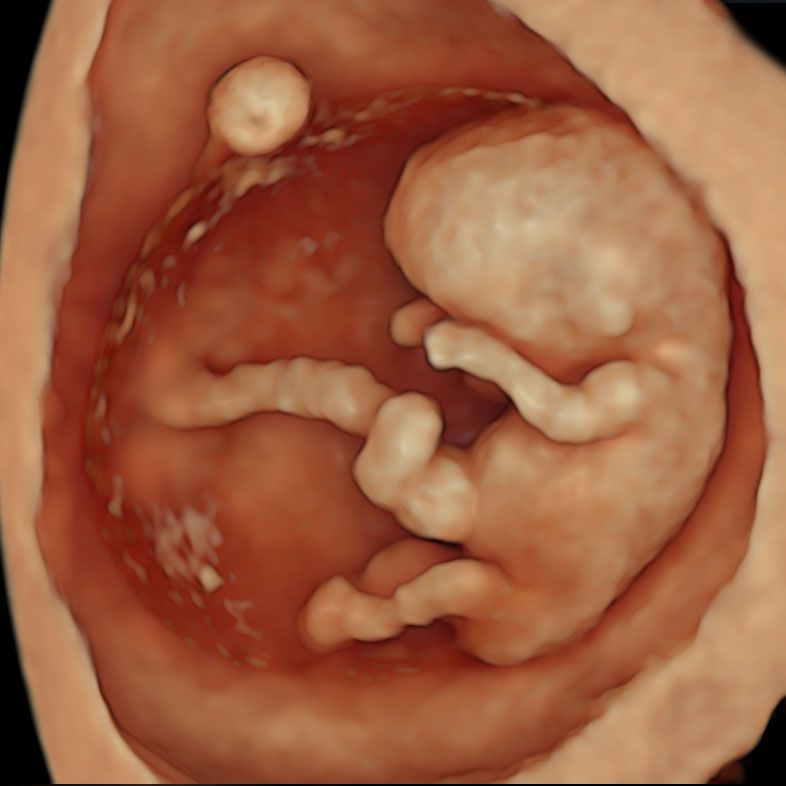
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Patau Syndrome: Key Statistics
- Patau syndrome occurs in approximately 1 in 5,000 live births, making it one of the more common chromosomal conditions (NCBI StatPearls)
- The condition occurs in approximately 1 in 5,000 live births, though many affected pregnancies result in miscarriage (NCBI StatPearls)
- The sex ratio at birth is slightly skewed towards females, presumably due to decreased survival amongst males
- Most cases (approximately 95%) result from random chromosomal changes in healthy parents and are not inherited
- Pregnancies with Patau syndrome are 14.1 times more likely to deliver before 37 weeks’ gestation
- The condition is caused by an extra copy of chromosome 13 (trisomy 13) in each cell
- NHS screening is offered to all pregnant women between 18+0 and 20+6 weeks as part of the Fetal Anomaly Screening Programme
- A cut-off risk of 1 in 150 is used by NHS trusts to identify higher-chance results requiring further investigation
Patau Syndrome Testing and Support Options
Advanced NIPT screening is available from as early as 10 weeks of pregnancy to assess the risk of Patau syndrome. This blood test analyses fetal DNA circulating in maternal blood to evaluate chromosomal conditions including trisomy 13. The test demonstrates high accuracy for detecting Patau syndrome, providing early information about pregnancy health.
Multiple NIPT options exist including SMART Test NIPT and PrenatalSAFE NIPT, allowing selection of the most appropriate screening approach. Results are typically available within 7-10 working days, and genetic counselling is available to discuss findings and potential next steps.
Comprehensive anomaly scans can identify physical features associated with Patau syndrome through detailed ultrasound examination. These assessments evaluate fetal development and structural abnormalities that may indicate chromosomal conditions. The heart, brain, kidneys, limbs, and facial features are examined with particular attention to markers associated with trisomy 13.
When concerning features are identified, immediate support is available and urgent referrals for further testing can be arranged. Specialised fetal echocardiography offers detailed heart scanning, as cardiac abnormalities are commonly associated with Patau syndrome and require expert evaluation.
Comprehensive genetic counselling is available for families facing a potential or confirmed Patau syndrome diagnosis. Pre-test counselling helps explain screening options, risk assessment, and implications of different test results. Following any positive screening results, detailed post-test counselling discusses diagnostic options, prognosis, and support resources.
Counselling sessions can be arranged in-person or through online genetic counselling services, ensuring accessible support when needed. Close coordination with NHS fetal medicine centres ensures comprehensive support throughout the pregnancy journey.
When screening tests indicate increased risk for Patau syndrome, diagnostic testing coordination includes amniocentesis and chorionic villus sampling (CVS). These definitive tests involve taking a small sample of fetal cells for chromosomal analysis, providing conclusive diagnosis. Collaboration with leading NHS and private laboratories ensures accurate, timely results.
Comprehensive pre-procedure counselling explains the benefits and risks of diagnostic testing. Following procedures, ongoing support is available and immediate follow-up appointments can be arranged to discuss results and coordinate any necessary specialist referrals or additional care requirements.
Nuchal translucency scans performed between 11-14 weeks can identify increased risk for chromosomal conditions including Patau syndrome. This early assessment measures fluid collection at the back of the baby’s neck and evaluates other early markers. Combined with maternal blood screening, this provides valuable risk assessment information.
Early pregnancy scans are available to establish accurate dating and monitor early development. Accurate pregnancy dating is essential for optimal timing of screening tests and ensures results are interpreted correctly within appropriate gestational age parameters.
When Patau syndrome is diagnosed, coordination with NHS fetal medicine centres and specialist paediatric teams provides comprehensive care. This includes arranging specialist consultations with neonatologists, paediatric cardiologists, and palliative care teams as appropriate. Seamless communication between all healthcare providers involved in care is facilitated.
Strong relationships with support organisations enable provision of information about local and national resources for families affected by Patau syndrome. Both medical and emotional support needs are addressed throughout the pregnancy and beyond, recognising the significant impact of this diagnosis.
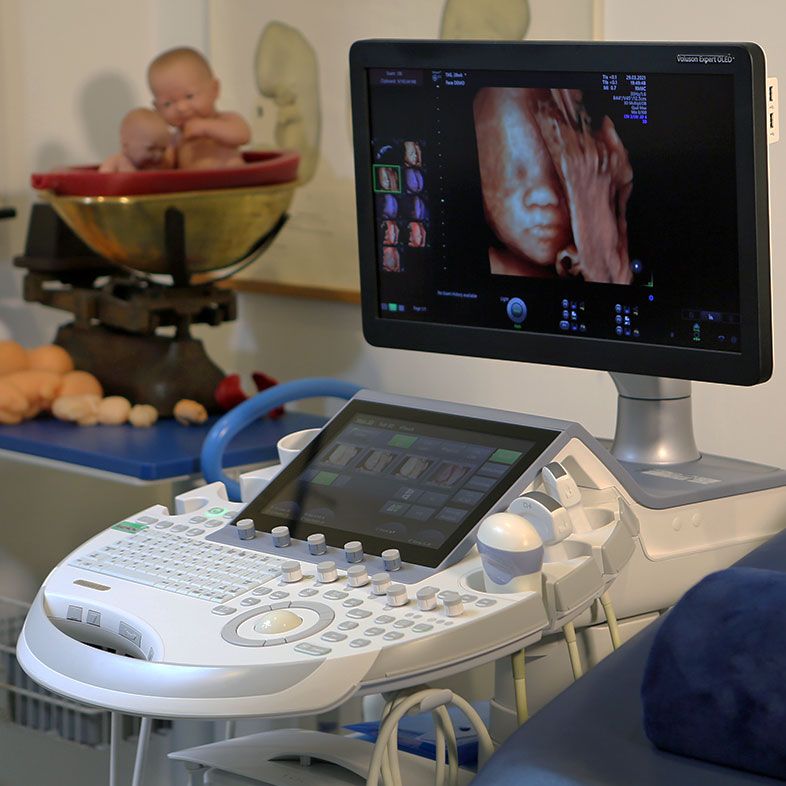
Ultrasound scans can sometimes provide early clues
Ultrasound signs of Patau Syndrome during pregnancy
Fetal anomalies linked to Patau syndrome may include physical features affecting different organs and systems. These structural abnormalities often involve the central nervous system, heart, kidneys, and facial development, and can be detected during routine pregnancy scans.
Fetal signs of Patau syndrome called soft markers or anatomical variants, are minor physical features occasionally detected during prenatal scans. While they are not structural anomalies, their presence might slightly raise the statistical likelihood of chromosomal conditions like trisomy 13.
When healthcare providers assess these findings they may consider additional testing. Tests like chorionic villus sampling (CVS) or amniocentesis may be needed for chromosomal analysis, while detailed ultrasound and maternal serum AFP screening are used for neural tube defects.
Holoprosencephaly
A severe brain malformation where the cerebral hemispheres fail to separate properly during early development. This appears on ultrasound as abnormal brain structure with absent or incomplete division between the left and right sides of the brain.
Cardiac defects
Complex congenital heart defects are commonly present in babies with Patau syndrome. These may include septal defects, hypoplastic left heart syndrome, or other structural heart abnormalities visible during fetal echocardiography.
Cleft lip and palate
Bilateral cleft lip and palate are commonly associated with Patau syndrome and can be detected during routine anomaly scans. The facial profile may show characteristic features including a small head (microcephaly) and low-set ears.
Polydactyly
Extra fingers or toes are frequently seen in Patau syndrome, particularly involving the hands. This can be detected during detailed ultrasound examination of the fetal limbs and digits during the second trimester anomaly scan.
Renal abnormalities
Kidney defects including polycystic kidneys or absent kidneys may be detected during pregnancy scans. These abnormalities can affect amniotic fluid levels and may be associated with growth restriction.
Omphalocele
A condition where abdominal organs protrude outside the body through the umbilical cord. This abdominal wall defect appears on ultrasound as organs located outside the normal abdominal cavity.
Growth restriction
Intrauterine growth restriction (IUGR) is commonly associated with Patau syndrome, where the baby measures smaller than expected for gestational age. This may be detected through serial growth scans and estimated fetal weight calculations.
Neural tube defects
Spinal abnormalities including spina bifida may occur in association with Patau syndrome. These defects in neural tube closure can be detected during detailed spinal examination on anomaly scanning.


