Alobar Holoprosencephaly
Alobar holoprosencephaly is a serious fetal brain condition that can be detected during pregnancy screening. Detailed ultrasound examination and genetic counselling are available to support families through this challenging diagnosis.
Alobar Holoprosencephaly: Key Information
Alobar holoprosencephaly is the most severe form of holoprosencephaly, a structural brain abnormality resulting from a midline differentiation and cleavage defect in the prosencephalon during the third and fourth weeks of gestation. In this condition, the fetal brain fails to divide into two hemispheres at all, resulting in the loss of midline structures of the brain and face, as well as fusion of the brain cavities. This represents the most common malformation of the prosencephalon in humans, with many affected pregnancies not reaching term.
During pregnancy, alobar holoprosencephaly can be diagnosed through detailed ultrasound examination and specialist anomaly scanning, often as early as the first trimester when examining the face and falx cerebri. Advanced screening options such as NIPT can help identify associated chromosomal conditions like trisomy 13, whilst amniocentesis may be recommended for definitive genetic diagnosis. Early detection allows families to make informed decisions about their pregnancy with appropriate specialist support.
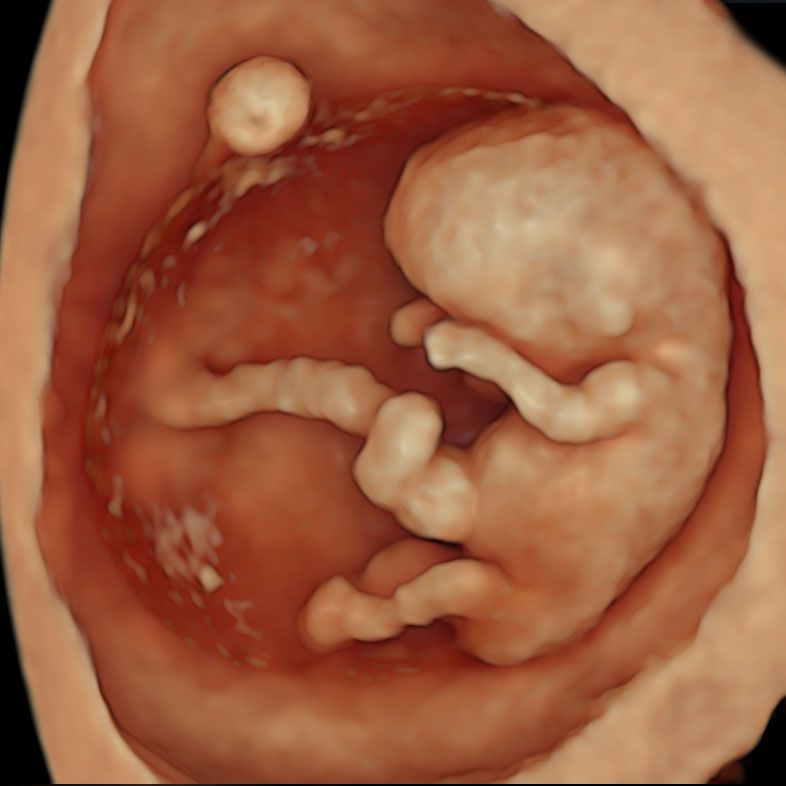
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Alobar Holoprosencephaly Statistics
-
Holoprosencephaly is the most common malformation of the prosencephalon in humans
-
Alobar and lobar holoprosencephaly are associated with microcephaly and midfacial defects in 80% of cases
-
The alobar variety is the most severe form of holoprosencephaly and incompatible with life
-
Extracerebral defects are particularly common in fetuses with trisomies 13 and 18
-
The NHS Fetal Anomaly Screening Programme aims for an 80% detection rate of all cases of HPE
Investigations and support for alobar holoprosencephaly
Detailed anomaly scans can identify alobar holoprosencephaly and associated brain malformations through comprehensive neurosonography assessment of brain development, midline structures, and facial features. Ultrasound examination can assess brain division patterns, ventricular structure, and the presence or absence of key brain structures such as the falx cerebri.
When alobar holoprosencephaly is suspected, immediate specialist consultation may be arranged with coordination of care involving fetal medicine specialists. This ensures families receive clear explanations of findings and appropriate referrals for further assessment, including genetic counselling and additional diagnostic testing as needed.
Through early pregnancy scans and nuchal translucency screening, early signs of brain malformations and associated chromosomal conditions can be detected. First trimester screening allows for early identification of holoprosencephaly through assessment of facial structures and brain development patterns from as early as 10-14 weeks of pregnancy.
Early screening approaches enable timely diagnosis, allowing families more time to consider their options and access appropriate support services. Coordination with genetic specialists can ensure comprehensive assessment when early indicators of alobar holoprosencephaly are identified.
Given the association between alobar holoprosencephaly and chromosomal abnormalities such as trisomy 13, NIPT screening is available to assess genetic risk factors. Various NIPT options, including SMART Test and other screening panels, can identify chromosomal conditions that may be associated with holoprosencephaly.
NIPT provides valuable information about genetic risk factors early in pregnancy, helping to guide further diagnostic decisions. When combined with detailed ultrasound assessment, NIPT offers comprehensive screening for conditions associated with alobar holoprosencephaly.
Specialist genetic counselling is available for families facing a diagnosis of alobar holoprosencephaly through both 30-minute and 60-minute counselling sessions. These sessions can help families understand the condition, inheritance patterns, and recurrence risks for future pregnancies.
Counselling services include discussion of diagnostic options, pregnancy management decisions, and emotional support throughout the diagnostic process. Evidence-based information is provided to help families make informed choices whilst respecting their individual values and circumstances.
When alobar holoprosencephaly is suspected, access to definitive diagnostic testing through amniocentesis and detailed genetic analysis can be coordinated. This may involve working with fetal medicine centres to ensure comprehensive chromosomal and genetic testing when indicated.
Clear guidance about the benefits and limitations of different diagnostic approaches can be provided, helping families understand their options for confirming the diagnosis. Coordination ensures seamless care pathways and timely access to specialist services when diagnostic testing is recommended.
Fetal medicine consultant consultations are available to provide specialist assessment and guidance following diagnosis. These consultations can complement NHS care and provide additional expertise in managing complex fetal conditions and supporting family decision-making.
Specialist consultation can provide compassionate, individualised guidance throughout the pregnancy journey, respecting family decisions whilst offering medical expertise and emotional support. Assessment protocols can ensure optimal care coordination whilst acknowledging the complex nature of this diagnosis.
Ultrasound scans can sometimes provide early clues
Ultrasound signs of alobar holoprosencephaly during pregnancy
Fetal anomalies linked to alobar holoprosencephaly may include severe brain malformations affecting cerebral development and facial structures. These structural changes represent fundamental developmental disruptions occurring in early pregnancy.
Ultrasound findings in alobar holoprosencephaly are typically severe and distinctive, involving both brain and facial abnormalities. The condition presents with characteristic features that can be identified during detailed scanning.
When these findings are detected, specialist consultation may be recommended. Additional testing such as NIPT, detailed genetic analysis, or amniocentesis may be suggested to assess for associated chromosomal conditions.
Single Brain Ventricle
The most characteristic finding is the presence of a single, horseshoe-shaped cerebral ventricle rather than the normal two separate lateral ventricles. This represents the failure of the brain to divide into distinct hemispheres during early development.
Absent Falx Cerebri
The falx cerebri, the membrane that normally separates the two brain hemispheres, is absent in alobar holoprosencephaly. This absence is a key diagnostic feature visible on ultrasound examination of the fetal brain.
Fused Frontal Cortex
The frontal portions of the brain appear as a single mass rather than separate hemispheres. This fusion represents the fundamental failure of brain division that characterises the alobar form of holoprosencephaly.
Facial Midline Defects
Severe facial abnormalities including cyclopia (single central eye), proboscis (trunk-like nasal structure), or cleft lip and palate may be present. These facial features reflect the disruption of normal midline facial development.
Microcephaly
The fetal head circumference is typically significantly smaller than normal due to the severe underdevelopment of brain tissue. Microcephaly is present in approximately 80% of cases of alobar holoprosencephaly.
Hypotelorism
When both eyes are present, they are positioned abnormally close together due to the failure of normal facial midline development. This close-set eye appearance is a characteristic feature of the condition.
Alobar holoprosencephaly is the most severe form of holoprosencephaly, a brain malformation where the fetal brain fails to divide into two separate hemispheres during early pregnancy development. This condition occurs during the third and fourth weeks of gestation when normal brain division processes are disrupted. In alobar holoprosencephaly, the brain remains as a single structure with fused ventricles and absent midline brain structures.
The condition is incompatible with life and represents the most serious form of prosencephalic malformation. Associated facial abnormalities often accompany the brain malformation, including severe midline facial defects that can be detected during pregnancy screening.
Alobar holoprosencephaly results from a midline differentiation and cleavage defect in the prosencephalon during critical early weeks of fetal development. The exact cause can vary and may include chromosomal abnormalities (particularly trisomy 13), genetic mutations, or environmental factors affecting early brain development. In many cases, the condition occurs as part of genetic syndromes or chromosomal disorders.
Some cases are associated with inherited genetic conditions, whilst others occur spontaneously without a clear family history. Environmental factors such as maternal diabetes or certain medications during early pregnancy may also contribute to the risk of developing this condition.
Diagnosis typically occurs through detailed ultrasound examination during pregnancy, often as early as the first trimester when examining brain structures and facial features. Specialist anomaly scanning can identify the characteristic single brain ventricle, absent falx cerebri, and associated facial abnormalities that define this condition.
Additional testing may include genetic analysis through amniocentesis to identify associated chromosomal conditions such as trisomy 13. Imaging techniques and fetal MRI may provide additional diagnostic information about the extent of brain malformation.
During pregnancy, ultrasound findings reveal severe brain malformations including a single horseshoe-shaped ventricle, fused frontal brain tissue, and absent normal brain division structures. Facial abnormalities are common and may include cyclopia (single central eye), proboscis, severe cleft lip and palate, or hypotelorism (closely-spaced eyes).
Microcephaly (small head size) is present in approximately 80% of cases. Other associated findings may include growth restriction and additional structural abnormalities depending on any underlying genetic syndrome present.
The inheritance pattern varies depending on the underlying cause. Some cases occur as part of autosomal recessive or autosomal dominant genetic conditions, whilst others result from new chromosomal abnormalities such as trisomy 13. Many cases occur sporadically without a clear inheritance pattern.
Families with a history of holoprosencephaly may benefit from genetic counselling to understand recurrence risks for future pregnancies. The specific inheritance pattern depends on whether an underlying genetic cause can be identified through testing.
Alobar holoprosencephaly carries a very poor prognosis and is considered incompatible with life. The severe brain malformation prevents normal neurological development and function. Most pregnancies affected by this condition result in pregnancy loss or death shortly after birth.
The condition represents the most severe form of holoprosencephaly, unlike milder forms which may be compatible with survival. Early diagnosis allows families to make informed decisions about pregnancy management with appropriate specialist support and counselling.
Following diagnosis, pregnancy management focuses on supporting family decision-making and providing comprehensive information about the condition and its implications. Specialist fetal medicine consultation may be arranged to discuss the diagnosis, prognosis, and available options for pregnancy continuation or termination.
If families choose to continue the pregnancy, care focuses on maternal wellbeing and preparation for the likely outcomes. Palliative care planning and psychosocial support become important aspects of ongoing pregnancy management through NHS services.
Detailed ultrasound scanning is the primary method for detecting alobar holoprosencephaly, with diagnosis possible as early as the first trimester through examination of brain structures and facial features. First trimester screening may identify early signs, whilst detailed anomaly scanning provides definitive diagnosis.
NIPT screening can identify associated chromosomal conditions such as trisomy 13, which is frequently associated with holoprosencephaly. Additional diagnostic testing through amniocentesis may be recommended to confirm genetic causes of the condition.
Holoprosencephaly is classified into several types based on severity. Alobar holoprosencephaly is the most severe form with complete failure of brain division. Semilobar and lobar forms represent less severe variations where some brain division has occurred, though significant malformations remain present.
A microform variant represents the mildest form, sometimes with minimal brain involvement but facial midline abnormalities. Each type carries different implications for development and survival, with alobar being the most severe and incompatible with life.
Comprehensive support includes genetic counselling to help families understand the condition, its causes, and implications for future pregnancies. Specialist fetal medicine teams can provide detailed information about the diagnosis and coordinate appropriate care pathways throughout the pregnancy journey.
Psychological support and bereavement counselling are available as essential components of care, helping families process this difficult diagnosis. Support groups and charitable organisations can provide additional resources and connection with other families who have experienced similar diagnoses.
Prevention strategies focus on managing known risk factors where possible. For women with diabetes, optimal blood sugar control before and during early pregnancy may reduce risk. Avoiding potentially harmful medications and substances during early pregnancy when brain development occurs is important.
For families with known genetic risk factors, preconception genetic counselling can provide information about reproductive options including preimplantation genetic diagnosis. However, many cases occur spontaneously and cannot be prevented through current medical interventions.
Screening tests such as ultrasound examination and NIPT assess the likelihood of alobar holoprosencephaly or associated conditions, but cannot provide definitive diagnosis. Ultrasound findings may strongly suggest the diagnosis, whilst NIPT can identify chromosomal risk factors such as trisomy 13.
Diagnostic tests such as amniocentesis with genetic analysis provide definitive confirmation of chromosomal or genetic causes of the condition. These tests carry small procedural risks but offer certainty about genetic diagnosis when this information is needed for decision-making.
Prenatal diagnosis of alobar holoprosencephaly through detailed ultrasound examination is highly accurate when performed by experienced practitioners. The severe brain malformations characteristic of this condition are typically readily identifiable on ultrasound, particularly when examining brain structure division and facial features.
The NHS Fetal Anomaly Screening Programme targets an 80% detection rate for holoprosencephaly cases. Accuracy is highest when combining detailed neurosonography with assessment of facial structures and genetic testing when indicated.
Genetic counselling provides comprehensive information about alobar holoprosencephaly, including its causes, inheritance patterns, and implications for the current pregnancy and future reproductive planning. Counsellors help families understand complex genetic information and make informed decisions about testing and pregnancy management.
Sessions include discussion of recurrence risks for future pregnancies, available reproductive options, and emotional support throughout the diagnostic process. Counsellors work with families to ensure they have the information and support needed to make decisions aligned with their values and circumstances.
There are no curative treatments for alobar holoprosencephaly, as the condition represents a fundamental developmental malformation that cannot be corrected. The severe nature of the brain malformation makes therapeutic intervention ineffective in improving outcome or survival.
Management focuses on supportive care and family support rather than treatment of the condition itself. This includes appropriate pregnancy counselling, psychosocial support, and palliative care planning when families choose to continue the pregnancy despite the poor prognosis.
Alobar holoprosencephaly can potentially be detected as early as the first trimester of pregnancy through detailed ultrasound examination of brain structures and facial features. Ultrasound techniques allow assessment of brain division and midline structures from approximately 10-14 weeks of pregnancy.
However, definitive diagnosis is often confirmed during the second trimester anomaly scan when fetal structures are larger and more clearly visualised. Early pregnancy scanning by specialist practitioners may identify suspicious findings that warrant further detailed assessment.


