Congenital Heart Defects
Congenital heart defects are structural abnormalities of the heart present from birth, affecting approximately 1 in 100 babies. Specialised cardiac screening and genetic counselling can help families understand these conditions and plan appropriate care.
Congenital Heart Defects: Key Information
Congenital heart defects are structural abnormalities of the heart that develop during fetal growth, affecting the heart’s chambers, valves, or major blood vessels. These conditions range from simple defects that may cause no symptoms to complex abnormalities requiring immediate surgical intervention. According to the NHS, congenital heart disease affects people aged 16 and over living with a heart defect acquired during fetal development.
During pregnancy, specialised cardiac screening can identify many heart defects before birth, allowing families to prepare for appropriate medical care. Fetal echocardiography provides detailed assessment of the developing heart, while anomaly scans can detect structural abnormalities. For families with a history of congenital heart defects, carrier screening tests and genetic counselling help assess recurrence risks and inform family planning decisions.
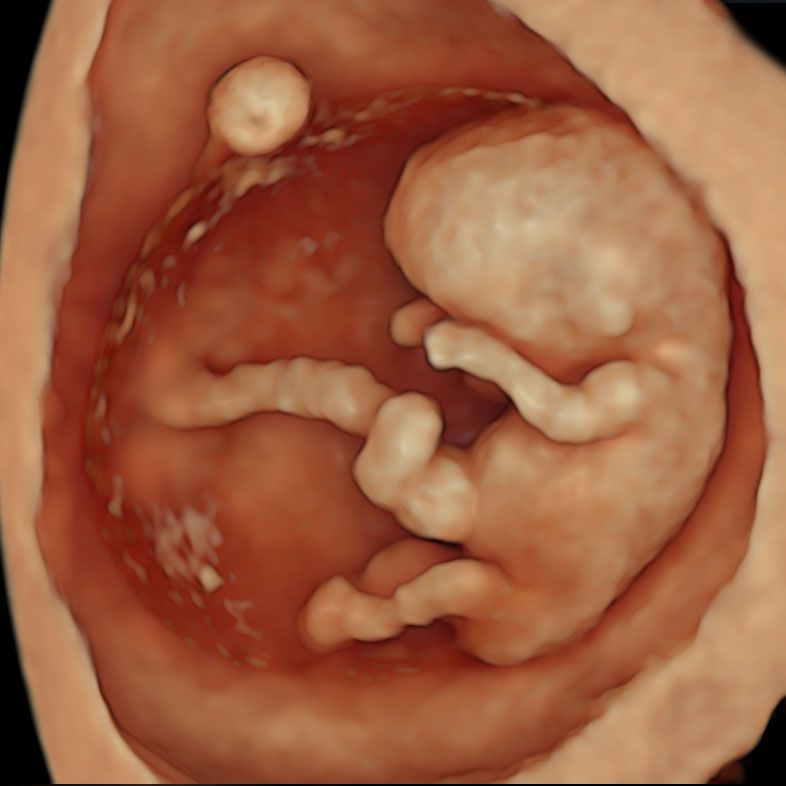
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Congenital Heart Defects statistics
-
Approximately 1 in 100 babies are born with a congenital heart defect in the UK
-
Risk is higher when the affected parent is the mother rather than the father
Investigations and support for congenital heart defects
Specialist fetal echocardiography provides detailed assessment of the developing heart using ultrasound technology. This specialised scan examines the heart’s structure, rhythm, and function in detail, allowing early detection of congenital heart defects. The investigation is particularly valuable for families with a history of heart defects or when routine scans suggest possible cardiac abnormalities.
Performed by specialists, fetal echocardiography can identify complex heart conditions and help families prepare for appropriate medical care after birth. Early detection allows for coordinated care planning with paediatric cardiology teams and ensures delivery at centres equipped for immediate specialist intervention if required.
Detailed anomaly scans include careful examination of the fetal heart as part of routine pregnancy screening. These scans can detect many structural heart defects and identify cases requiring further specialist cardiac assessment. Advanced ultrasound equipment ensures thorough evaluation of fetal development.
When cardiac abnormalities are suspected during routine scanning, immediate referral pathways for specialist fetal echocardiography are available, with coordination of care between appropriate medical teams. This approach ensures continuity of care and reduces anxiety through clear communication and guidance throughout the diagnostic process.
For families with a history of congenital heart defects, genetic counselling provides comprehensive risk assessment and family planning guidance. Counsellors help families understand inheritance patterns, recurrence risks, and available screening options during pregnancy. Both in-person and online genetic counselling appointments are available.
Genetic counselling is particularly valuable for conditions with known genetic components, such as those associated with chromosomal abnormalities or inherited syndromes. Close working relationships with specialist genetics services enable appropriate genetic testing when indicated, including preconception carrier screening and prenatal diagnostic options.
NIPT services can detect chromosomal conditions that may be associated with congenital heart defects, such as Down syndrome, Edwards syndrome, and Patau syndrome. These conditions carry increased risks of cardiac abnormalities, making early screening particularly valuable for comprehensive care planning.
Several NIPT options are available including SMART Test NIPT and KNOVA NIPT by Fulgent, each providing screening from as early as 9-10 weeks of pregnancy. Early identification of chromosomal conditions allows for timely cardiac assessment and appropriate care coordination.
For pregnancies at increased risk of congenital heart defects, specialist consultation is available through fetal medicine specialists who can provide expert assessment and guidance. Early pregnancy scans help establish accurate dating and baseline measurements, essential for optimal timing of specialist cardiac screening.
Specialist consultation ensures that high-risk pregnancies receive appropriate surveillance and timely referral for cardiac assessment. Care can be coordinated with maternal-fetal medicine specialists and paediatric cardiology teams to provide comprehensive support throughout pregnancy and delivery planning.
When congenital heart defects are diagnosed, care coordination with specialist paediatric cardiology services, maternal-fetal medicine units, and appropriate delivery centres is available. Families can receive comprehensive information about their baby’s condition and connect with relevant support services and specialist care teams.
This coordinated approach includes liaison with NHS specialist centres, private paediatric cardiology services, and support organisations. Ongoing communication throughout pregnancy helps families prepare for delivery and postnatal care, ensuring smooth transitions between different aspects of specialist medical care.
Ultrasound scans can sometimes provide early clues
Ultrasound signs of congenital heart defects during pregnancy
Fetal cardiac anomalies encompass a wide range of structural abnormalities affecting the heart’s chambers, valves, and major vessels. These may be detected during routine anomaly scanning or require specialist fetal echocardiography for detailed assessment.
Cardiac markers and associated findings may include features affecting heart rhythm, size, or function. While some findings represent clear structural abnormalities, others may be soft markers suggesting increased risk requiring further evaluation.
When cardiac abnormalities are suspected, additional testing may be recommended. Investigations like fetal echocardiography, NIPT, or invasive diagnostic testing may be needed for comprehensive assessment.
Septal Defects
Holes in the walls separating the heart’s chambers, including ventricular septal defects (VSD) and atrial septal defects (ASD). These appear as breaks in the continuity of the septum and may be associated with abnormal blood flow patterns visible on Doppler ultrasound.
Valve Abnormalities
Malformed or poorly functioning heart valves, including pulmonary stenosis, aortic stenosis, or tricuspid atresia. These may cause abnormal blood flow patterns, valve regurgitation, or stenosis detectable through detailed cardiac assessment and Doppler studies.
Complex Cardiac Anomalies
Serious structural abnormalities such as hypoplastic left heart syndrome, tetralogy of Fallot, or transposition of great arteries. These conditions involve multiple cardiac structures and require immediate specialist assessment and coordinated postnatal care planning.
Cardiac Arrhythmias
Abnormal fetal heart rhythms including bradycardia (slow heart rate), tachycardia (fast heart rate), or irregular rhythms. These may indicate underlying structural problems or electrical conduction abnormalities requiring specialist cardiac evaluation.
Cardiomegaly
Enlarged fetal heart relative to body size, which may indicate underlying cardiac dysfunction, structural abnormalities, or other conditions affecting heart function. This finding typically requires detailed echocardiographic assessment and ongoing monitoring.
Great Vessel Abnormalities
Abnormalities of the major blood vessels including coarctation of aorta, interrupted aortic arch, or abnormal vessel connections. These may affect blood circulation and require specialist assessment to determine severity and treatment requirements.
Congenital heart defects are structural abnormalities of the heart that develop during fetal development, affecting approximately 1 in 100 babies born in the UK. These conditions involve malformations of the heart’s chambers, valves, or major blood vessels that occur during the first eight weeks of pregnancy when the heart is forming. The severity ranges from simple defects that may never cause symptoms to complex abnormalities requiring immediate surgical intervention.
According to the NHS, some cases are simple and may not cause symptoms, while others can be life-threatening and require treatment in infancy. Healthcare providers can detect many heart defects early through prenatal screening, though sometimes diagnosis doesn’t occur until childhood or even adulthood.
Most congenital heart defects occur without a clear cause, developing during the critical period of heart formation in early pregnancy. Known risk factors include maternal infections such as rubella during pregnancy, certain medications, smoking or exposure to secondhand smoke, and maternal conditions like diabetes. Genetic factors also play a role, with some defects associated with chromosomal conditions like Down syndrome.
Family history increases risk, with studies showing that if one parent has a congenital heart defect, the risk for their children increases to between 3-6%. Environmental factors during pregnancy, including alcohol consumption and exposure to certain chemicals, may also contribute to the development of heart defects.
Prenatal diagnosis typically begins with routine anomaly scans around 18-22 weeks of pregnancy, which include examination of the fetal heart’s basic structure. When abnormalities are suspected or for high-risk pregnancies, specialist fetal echocardiography provides detailed assessment of heart structure and function using ultrasound techniques.
Additional testing may include NIPT screening to detect chromosomal conditions associated with heart defects, and in some cases, invasive diagnostic tests like amniocentesis may be recommended. Early diagnosis allows families to prepare for appropriate specialist care and delivery planning at centres equipped for immediate postnatal intervention if required.
Symptoms vary significantly depending on the type and severity of the heart defect. Some babies may show no symptoms initially, while others may experience cyanosis (bluish skin colour), difficulty feeding, poor weight gain, or rapid breathing. More severe defects may cause heart failure symptoms including excessive sweating, fatigue during feeding, or swelling.
The NHS recommends pulse oximetry testing as a potential screening tool for detecting congenital heart disease in newborns. Some defects only become apparent as children grow and their activity levels increase, while others require immediate medical attention from birth.
Most congenital heart defects are not directly inherited, but genetic factors do influence risk. Research published in medical journals shows that if one parent has a congenital heart defect, the risk for their children increases to 3-6% compared to the general population risk of 0.8%. The risk is higher when the affected parent is the mother.
Some heart defects are associated with genetic syndromes that follow inheritance patterns, such as Marfan syndrome which has a 50% recurrence risk. For families with a history of heart defects, genetic counselling can help assess individual risks and discuss available screening options during pregnancy.
Treatment varies widely depending on the type and severity of the defect. Some simple defects may require only monitoring, while others need immediate surgical intervention in the newborn period. Medications may be prescribed to strengthen heart function, improve oxygen levels in the blood, or manage symptoms like heart failure.
Many defects can be successfully repaired through surgical procedures, though some complex conditions require multiple operations throughout childhood and adulthood. Modern cardiac surgery has excellent outcomes for most congenital heart defects, allowing many individuals to lead normal, active lives with appropriate ongoing medical care.
Many women with congenital heart defects can have successful pregnancies, though pregnancy does place additional strain on the heart. According to the NHS, if you have heart disease you may be able to have a successful pregnancy, but careful medical supervision is essential throughout pregnancy and delivery.
Pre-pregnancy counselling is crucial to assess individual risks and optimise maternal health before conception. Some medications may need to be reviewed for safety during pregnancy, and delivery planning often involves specialist obstetric and cardiac teams. Enhanced monitoring throughout pregnancy helps ensure both maternal and fetal wellbeing.
The prognosis varies significantly depending on the specific type of defect and whether treatment is available. Many simple defects have excellent long-term outcomes with normal life expectancy and activity levels. More complex defects may require ongoing medical care and repeated interventions, but modern treatments have dramatically improved outcomes.
Adults with congenital heart disease require specialised follow-up care, as the NHS provides Adult Congenital Heart Disease services for people aged 16 and over. Many individuals with successfully treated heart defects can participate in normal activities, pursue education and careers, and have families of their own with appropriate medical guidance.
Chromosomal conditions significantly increase the risk of congenital heart defects. Down syndrome (trisomy 21) is associated with heart defects in approximately 40-50% of cases, while Edwards syndrome and Patau syndrome also carry high risks of cardiac abnormalities.
This is why detailed cardiac assessment is recommended when chromosomal conditions are diagnosed prenatally. Early screening through NIPT can identify pregnancies at increased risk, allowing for appropriate specialist cardiac evaluation and care planning.
Genetic counselling is recommended for families with a personal or family history of congenital heart defects, particularly when planning pregnancy. Counselling is especially valuable for those with aortic disease, multiple affected family members, or when other non-cardiac congenital abnormalities might be present.
For couples with known genetic defects, preimplantation genetic testing has become available as an option. Genetic counselling helps families understand recurrence risks, available screening and diagnostic options, and supports informed decision-making about family planning and pregnancy management.
Enhanced screening protocols are recommended for pregnancies at increased risk of congenital heart defects. This typically includes detailed anomaly scanning with particular attention to cardiac structures, and specialist fetal echocardiography performed by experienced practitioners using ultrasound equipment.
The timing of screening is important, with detailed cardiac assessment usually performed between 18-22 weeks of pregnancy when heart structures are sufficiently developed for comprehensive evaluation. For very high-risk cases, earlier screening may be considered, and some centres offer specialised early cardiac scanning.
Detection rates vary depending on the type of defect and the expertise of the scanning centre. Complex defects are generally easier to detect than simple defects, and some subtle abnormalities may not be visible on prenatal ultrasound. Specialist fetal echocardiography performed at experienced centres achieves higher detection rates than routine screening.
Even with the best available technology and expertise, not all heart defects can be detected prenatally. This is why postnatal screening, including the recommended pulse oximetry testing for newborns, remains an important component of comprehensive cardiac care.
Comprehensive support services are available through NHS specialist centres, charitable organisations, and support groups connecting families with similar experiences. Many hospitals provide specialist nurses and counsellors who support families through diagnosis, treatment, and ongoing care.
Educational resources help families understand their child’s condition and treatment options, while peer support groups provide valuable emotional support and practical advice. Transition services help young people move from paediatric to adult cardiac services, ensuring continuity of specialist care throughout life.
While most heart defects cannot be prevented, some risk factors can be modified to reduce the likelihood of occurrence. This includes ensuring adequate folic acid intake before conception, avoiding alcohol and smoking during pregnancy, managing diabetes effectively, and avoiding exposure to infections like rubella.
For women taking medications that may affect fetal heart development, pre-pregnancy counselling allows for medication review and optimisation of treatment regimens. Genetic counselling helps identify families at higher risk and provides information about available screening and preventive options.
The impact on daily life varies tremendously depending on the type and severity of the defect and the success of any treatments received. Many individuals with successfully treated heart defects lead completely normal lives with no activity restrictions, while others may need to modify their activities or take regular medications.
Regular follow-up with specialist cardiac services helps monitor heart function and adjust treatment as needed. Most children with heart defects can attend regular school and participate in age-appropriate activities, though some may require individual assessment for sports participation or other physical activities.
When a heart defect is diagnosed prenatally, families receive detailed counselling about the specific condition, treatment options, and long-term outlook. The medical team coordinates care with paediatric cardiology specialists and plans for delivery at a centre equipped for immediate specialist intervention if required.
Families have time to prepare emotionally and practically for their baby’s arrival, including understanding what treatments may be needed and connecting with support services. Some families may consider additional diagnostic testing to clarify the diagnosis or assess for associated conditions, while others focus on preparation for postnatal care and treatment.
This page was created using information from the following trusted medical sources:
- Congenital Heart Disease | Congenital Heart Defects | MedlinePlus
- Pregnancy and congenital heart disease – PMC
- Pregnancy in congenital heart disease: risk prediction and counselling | Heart
- Congenital heart disease – Diagnosis – NHS
- Classification: Official 1 Congenital Heart Disease Standards & Specifications
- Classification: Official 1 Paediatric Congenital Heart Disease Specification
- Clinical Guidelines and Useful information – Northwest, North Wales, Isle of Man Congenital Heart Network
- Management Guidelines for Adults with Congenital Heart …
- Congenital heart disease – NHS
- Congenital Heart Disease: Symptoms & Treatment


