Amniotic Band Syndrome
Amniotic band syndrome is a rare but serious condition that can affect fetal development during pregnancy. Advanced ultrasound technology can detect and monitor this condition, providing detailed assessment and support for informed decision-making throughout pregnancy.
Amniotic Band Syndrome: Key Information
Amniotic band syndrome (ABS) is a rare congenital condition where fibrous bands of tissue form within the amniotic sac and wrap around developing fetal body parts. These bands can restrict blood flow and normal development, leading to a spectrum of congenital anomalies ranging from minor limb defects to more severe structural abnormalities. The condition occurs when the inner membrane of the placenta, called the amnion, is damaged during pregnancy, creating thin strands of tissue that can entangle the developing fetus. Research indicates the condition is rare with variable presentations.
Early detection of amniotic band syndrome is crucial for appropriate pregnancy management and planning for specialised care after birth. Comprehensive anomaly scans can identify signs of ABS from as early as 10 weeks through the 10-week scan. Detailed cardiac assessment may be available through fetal echocardiography when needed. For expectant parents facing an ABS diagnosis, genetic counselling offers expert guidance on prognosis, treatment options, and family planning considerations through genetic counselling consultations.
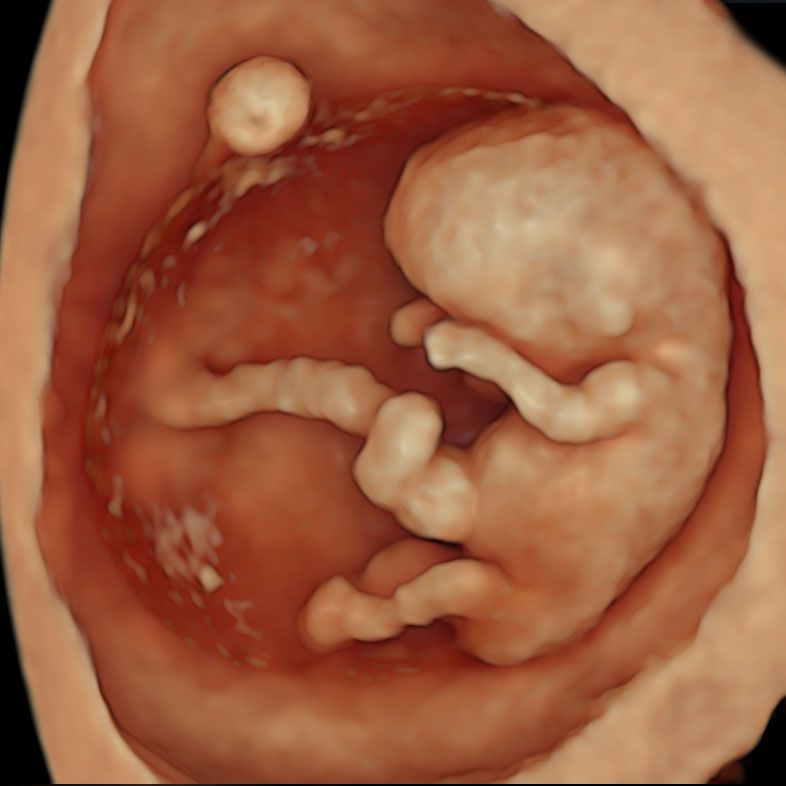
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Amniotic Band Syndrome statistics
-
The condition can cause various congenital limb defects
-
Limb defects are commonly observed, ranging from minor constriction rings to complete amputation
-
Facial clefts may be present in some affected cases
-
The condition affects males and females equally with no known genetic predisposition
-
Most cases can be detected during ultrasound examinations, with early detection possible from 10 weeks in some cases
Investigations and support for Amniotic Band Syndrome
Comprehensive anomaly scans utilise advanced ultrasound technology to detect signs of amniotic band syndrome and assess the extent of fetal involvement. Signs of ABS can be identified through detailed imaging, including limb constriction bands, digital amputations, and associated structural abnormalities. Early detection may be possible through the 10-week scan, which screens for major structural anomalies including amniotic band syndrome.
When amniotic bands are suspected, follow-up scans may be recommended to monitor fetal development and assess any progression of the condition. 3D/4D scanning capabilities can provide enhanced visualisation of limb defects and facial features, offering valuable information for surgical planning and parental counselling.
As amniotic band syndrome can occasionally affect cardiac development, fetal echocardiography services provide detailed assessment of fetal heart structure and function. This specialised scan is particularly important when other structural abnormalities are detected, as it helps identify any associated cardiac defects that may require immediate postnatal intervention.
Comprehensive cardiac evaluation can be coordinated with specialist paediatric cardiologists to ensure thorough assessment and appropriate referral pathways for complex cases. This collaborative approach ensures that families receive coordinated care planning for delivery and immediate postnatal management.
Although amniotic band syndrome is not a genetic condition, genetic counselling services provide essential support for families facing an ABS diagnosis. Information about the condition, prognosis based on specific findings, and implications for pregnancy and future family planning can be discussed.
Genetic counsellors can provide information about treatment options, facilitate connections with appropriate specialist teams, and offer emotional support throughout the pregnancy journey. Discussion of recurrence risks, which are typically very low for ABS, and addressing concerns about future pregnancies are also available.
Following an amniotic band syndrome diagnosis, regular monitoring throughout pregnancy may be recommended to assess fetal growth and wellbeing. Wellbeing scans can track fetal development, monitor amniotic fluid levels, and assess blood flow patterns to support optimal pregnancy management.
Coordination with maternal-fetal medicine specialists can be arranged to ensure appropriate timing of delivery. Monitoring protocols can help identify any complications early, allowing for timely intervention and optimal outcomes for both mother and baby.
Amniotic band syndrome often requires coordinated care from multiple specialists including plastic surgeons, orthopaedic surgeons, and paediatricians. Appropriate referrals to specialist centres can be facilitated and care plans for immediate postnatal management and long-term treatment can be coordinated.
Detailed reports and imaging studies can be provided to receiving teams, ensuring seamless transition of care. A comprehensive approach includes discussion of delivery planning, immediate postnatal care requirements, and long-term management strategies to optimise outcomes for affected children.
Ultrasound scans can sometimes provide early clues
Ultrasound signs of Amniotic Band Syndrome during pregnancy
Fetal anomalies linked to amniotic band syndrome may include limb defects, facial abnormalities, and body wall defects caused by constriction from fibrous amniotic bands. The severity and location of defects depend on which fetal parts become entangled and when during development this occurs.
Ultrasound detection of amniotic band syndrome relies on identifying characteristic patterns of constriction and associated structural abnormalities. The presence of visible amniotic bands on ultrasound, combined with typical fetal anomalies, helps establish the diagnosis.
When amniotic band syndrome is suspected, additional detailed scanning may be recommended. Comprehensive assessment helps determine the extent of involvement and guide appropriate management planning throughout the pregnancy.
Limb Constriction Bands
Visible bands of tissue wrapped around fetal limbs, causing constriction rings or grooves. These may appear as areas of swelling above and below the band, potentially leading to amputation if severe.
Digital Amputations
Missing or shortened fingers or toes, often with irregular patterns that distinguish ABS from genetic syndromes. The amputations typically occur at different levels and may affect multiple digits asymmetrically.
Facial Clefting
Atypical cleft lip and palate patterns that differ from isolated clefting, often extending beyond typical cleft patterns. These may be associated with other facial asymmetries or deformations.
Body Wall Defects
Defects in the abdominal or chest wall where organs may be outside the body cavity. These complex defects require immediate surgical intervention after birth and careful delivery planning.
Cranial Defects
Skull defects or brain malformations caused by amniotic band constriction. These may include encephaloceles or other neural tube-like defects with characteristic irregular patterns.
Spinal Abnormalities
Scoliosis or other spinal curvature abnormalities resulting from asymmetric constriction during development. These may be associated with other musculoskeletal abnormalities.
Amniotic band syndrome (ABS) is a rare congenital condition that occurs when fibrous bands of tissue form within the amniotic sac during pregnancy. These bands can wrap around developing fetal parts, restricting normal growth and development. The condition results from damage to the inner membrane of the placenta, called the amnion, which creates thin strands of tissue that can entangle the developing fetus.
The severity of ABS varies greatly depending on which body parts are affected and when during pregnancy the entanglement occurs. Some babies may have minor constriction rings around fingers or toes, whilst others may have more severe limb defects, facial abnormalities, or body wall defects requiring immediate postnatal surgical intervention.
The exact cause of amniotic band syndrome remains unknown, but it is believed to occur when the inner membrane of the placenta (amnion) ruptures or tears early in pregnancy, typically during the first trimester. This rupture creates floating strands of tissue within the amniotic fluid that can wrap around the developing fetus as it moves and grows.
ABS is not a genetic condition and does not run in families. It appears to be a random event during pregnancy with no known risk factors or preventable causes. The condition affects pregnancies equally regardless of maternal age, ethnicity, or previous pregnancy history.
Amniotic band syndrome can be diagnosed through detailed ultrasound examination, with detection possible from as early as 10 weeks through advanced scanning. The condition may be identified during routine anomaly scanning between 18-22 weeks of pregnancy, though earlier detection allows more time for management planning.
Diagnosis involves identifying typical features such as asymmetric limb defects, constriction rings, or facial clefting patterns that are characteristic of ABS. Comprehensive anomaly scans provide detailed assessment of fetal anatomy to determine the extent of involvement and guide appropriate management planning.
Amniotic band syndrome presents with various physical abnormalities that depend on which fetal parts become entangled in the amniotic bands. The most common features include limb defects such as constriction rings, missing or shortened fingers and toes, and in severe cases, complete limb amputations.
Other manifestations may include facial abnormalities such as atypical cleft lip and palate, body wall defects where internal organs may be outside the body cavity, and occasionally cranial or spinal defects. The pattern of abnormalities is typically asymmetric and irregular, which helps distinguish ABS from genetic syndromes.
No, amniotic band syndrome is not a genetic condition and does not run in families. It is considered a sporadic developmental accident that occurs randomly during pregnancy. The condition is not caused by genetic mutations or chromosomal abnormalities, and parents with one affected pregnancy do not have an increased risk of ABS in future pregnancies.
Because ABS is not genetic, genetic screening tests such as NIPT cannot detect this condition. Diagnosis relies entirely on detailed ultrasound examination to identify the characteristic physical abnormalities caused by amniotic band constriction.
Treatment for amniotic band syndrome focuses on surgical correction of the physical abnormalities after birth. The specific treatments required depend on which body parts are affected and the severity of the defects. Treatment may involve plastic surgery, orthopaedic procedures, or complex reconstructive surgery.
In rare cases, fetal surgery may be considered if life-threatening constriction is identified during pregnancy, though this is only performed in highly specialised centres. Most treatment occurs after birth with a coordinated approach involving multiple specialist teams to address limb reconstruction, facial repair, or correction of body wall defects.
The prognosis for amniotic band syndrome varies significantly depending on which body parts are affected and the severity of the abnormalities. Many children with minor limb defects or digital amputations have excellent long-term outcomes and can lead completely normal lives with appropriate surgical intervention and rehabilitation.
More complex cases involving multiple body systems or severe body wall defects may require extensive surgical procedures and long-term medical care. Early identification during pregnancy allows for appropriate planning and coordination with specialist teams to optimise outcomes and ensure the best possible care for affected children.
Most pregnancies affected by amniotic band syndrome can continue normally with regular monitoring to assess fetal growth and wellbeing. The presence of ABS does not typically affect the pregnancy process itself, though delivery planning may need special consideration depending on the specific abnormalities present.
Caesarean delivery may be recommended in cases with severe body wall defects or when immediate surgical intervention is required after birth. Coordination with maternal-fetal medicine specialists and paediatric surgical teams can ensure appropriate care planning and optimal delivery timing for the best outcomes.
Currently, there is no known way to prevent amniotic band syndrome as it appears to be a random developmental event during pregnancy. The condition is not associated with any modifiable risk factors or maternal behaviours, and maintaining good general pregnancy health does not reduce the risk of ABS.
Because the cause remains unknown and no risk factors have been identified, prevention strategies are not available. Focus instead remains on early detection through comprehensive ultrasound examination and appropriate management planning when the condition is diagnosed.
Pregnancies affected by amniotic band syndrome may require regular monitoring to assess fetal growth, wellbeing, and any progression of the condition. This typically involves serial ultrasound examinations to track development and monitor for any complications such as growth restriction or changes in amniotic fluid levels.
Wellbeing scans can provide comprehensive assessment throughout pregnancy, whilst coordination with specialist teams ensures appropriate delivery planning. Regular monitoring can help identify any complications early and allows for timely intervention to optimise outcomes for both mother and baby.
Limb defects are the most common manifestation of amniotic band syndrome, occurring in many affected cases. These defects can range from minor constriction rings around fingers or toes to more severe abnormalities including digital amputations or complete limb defects.
The pattern of limb involvement in ABS is typically asymmetric and irregular, which helps distinguish it from genetic causes of limb defects. Early detection through detailed scanning allows families to prepare for appropriate surgical planning and coordination with specialist orthopaedic and plastic surgery teams.
Comprehensive support services are available for families facing an amniotic band syndrome diagnosis. Genetic counselling services can provide guidance on the condition, discuss prognosis and treatment options, and offer emotional support throughout the pregnancy journey.
Appropriate referrals to specialist teams can be facilitated and care planning for delivery and postnatal management coordinated. Support groups and patient organisations also provide valuable resources for families to connect with others who have experience with ABS and access practical advice about managing the condition long-term.
Amniotic band syndrome does not increase the risk of complications in future pregnancies. Because ABS is not a genetic condition and appears to be a random developmental event, parents who have had one affected pregnancy do not have an increased risk of recurrence in subsequent pregnancies.
Future pregnancies can be managed normally with routine antenatal care, though some parents may choose to have additional reassurance scanning. The recurrence risk is extremely low, and previous experience with ABS does not require any special precautions or modified management in future pregnancies.
Treatment of amniotic band syndrome typically involves a multidisciplinary team of specialists depending on which body systems are affected. This may include plastic surgeons for limb reconstruction, orthopaedic surgeons for complex limb defects, maxillofacial surgeons for facial abnormalities, and paediatric surgeons for body wall defects.
Coordination between these specialists begins during pregnancy with appropriate referrals and delivery planning. Detailed imaging and reports can be provided to receiving teams to ensure seamless transition of care and optimal outcomes for affected children requiring complex surgical intervention.
Amniotic band syndrome can be distinguished from other congenital conditions by its characteristic pattern of asymmetric, irregular abnormalities caused by external constriction rather than genetic or developmental causes. Unlike genetic syndromes, ABS does not follow typical inheritance patterns or affect multiple family members.
The random, disruptive nature of ABS abnormalities contrasts with the more predictable patterns seen in genetic conditions. This distinction is important for prognosis, family counselling, and management planning, as ABS does not carry risks for future pregnancies or other family members.


