Hydrocephalus
Hydrocephalus is a condition characterised by accumulation of cerebrospinal fluid within the brain’s ventricles. This condition can be detected through detailed ultrasound scanning and may be associated with other fetal abnormalities requiring comprehensive assessment and support.
Hydrocephalus: Key Information
Hydrocephalus is a medical condition characterised by the accumulation of cerebrospinal fluid (CSF) within the brain’s ventricles, causing them to enlarge. This fluid buildup increases pressure inside the skull, which can lead to brain damage if left untreated. The condition can be present from birth (congenital hydrocephalus) or develop later in life (acquired hydrocephalus). Hydrocephalus can be detected during pregnancy, with congenital hydrocephalus accounting for most cases diagnosed during pregnancy.
During pregnancy, hydrocephalus can be detected through ultrasound examinations from as early as the first trimester with advanced scanning techniques. The 10-week scan can identify severe brain abnormalities, whilst the anomaly scan at 20-22 weeks provides detailed assessment of brain structure. Third trimester scans can monitor progression of the condition, and genetic counselling is available to help families understand inheritance patterns and recurrence risks.
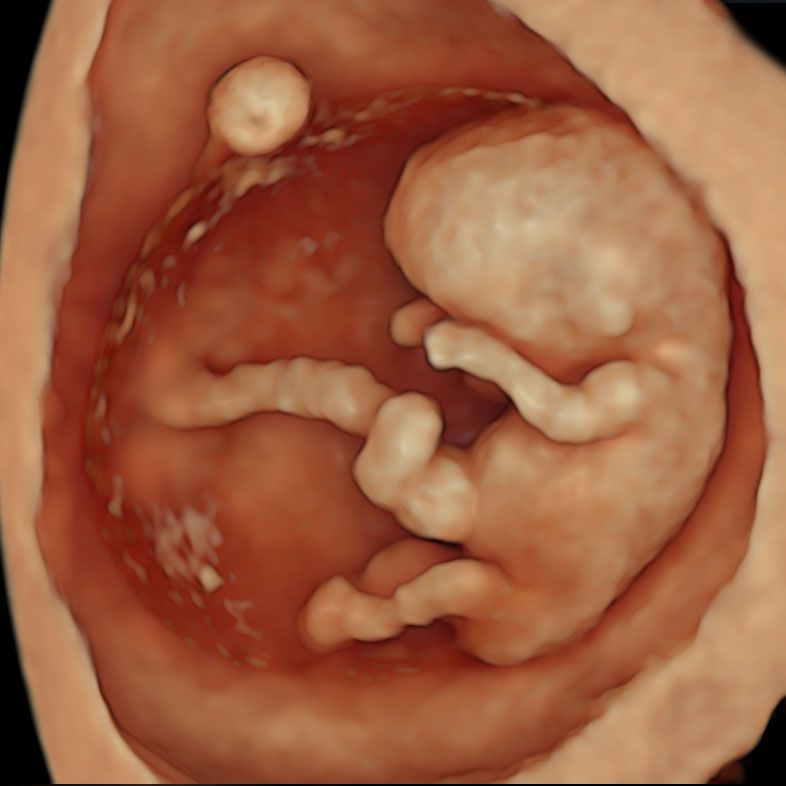
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Hydrocephalus statistics
-
Hydrocephalus can be detected during pregnancy through routine ultrasound scans
-
Around 70% of cases are detected during routine pregnancy ultrasound scans
-
Male fetuses are slightly more commonly affected than females
Investigations and support for hydrocephalus
Comprehensive anomaly scans can detect signs of hydrocephalus through detailed examination of brain structure, including measurement of enlarged ventricles and assessment of increased head circumference. These scans can identify even subtle changes in brain anatomy that may indicate early development of hydrocephalus, providing precise measurements of ventricular size to determine the severity of the condition.
Serial monitoring scans may be arranged to track the progression of hydrocephalus throughout pregnancy. These follow-up examinations can assess whether the condition remains stable, is progressing, or shows other changes, providing crucial information for delivery planning and postnatal care coordination.
When hydrocephalus is detected, genetic counselling services are available to help families understand the condition’s implications. These consultations can explain the different types of hydrocephalus, potential causes, and associated genetic factors that may have contributed to its development, as well as discuss inheritance patterns and recurrence risks for future pregnancies.
Coordination with genetic specialists can be arranged when additional testing is indicated, such as karyotyping or microarray analysis, to identify underlying chromosomal abnormalities that may be associated with hydrocephalus. This comprehensive approach ensures families receive all necessary information to make informed decisions about their pregnancy care.
Hydrocephalus can sometimes be associated with congenital heart defects, making cardiac evaluation an important component of comprehensive assessment. Fetal cardiac scans can provide detailed evaluation of heart structure and function to identify any coexisting cardiac abnormalities. Early detection of cardiac issues allows for appropriate planning and multidisciplinary care coordination.
These specialised examinations can assess all four chambers of the heart, major vessels, and blood flow patterns using high-resolution ultrasound technology. When cardiac abnormalities are identified alongside hydrocephalus, coordination with paediatric cardiologists can be arranged to ensure optimal care planning.
Third trimester scans can provide crucial monitoring for pregnancies affected by hydrocephalus, tracking the progression of ventricular enlargement and assessing overall fetal wellbeing. These detailed examinations can help inform optimal timing and method of delivery, considering factors such as head size and the severity of hydrocephalus.
Assessment of other important parameters including estimated fetal weight, amniotic fluid levels, and placental function can be performed to ensure comprehensive pregnancy monitoring. This information is vital for delivery planning and helps healthcare teams prepare for the specialised postnatal care that may be required.
Hydrocephalus can sometimes be associated with chromosomal abnormalities, making genetic screening an important consideration. Non-invasive prenatal testing (NIPT) is available to screen for common chromosomal conditions that may be associated with brain abnormalities, providing valuable additional information about fetal health.
When indicated, coordination of more comprehensive genetic testing such as amniocentesis can provide detailed chromosomal analysis. This information helps families understand the full scope of their baby’s condition and assists healthcare providers in developing appropriate care plans for both pregnancy and postnatal management.
Ultrasound scans can sometimes provide early clues
Ultrasound signs of hydrocephalus during pregnancy
Fetal signs of hydrocephalus typically involve enlargement of the brain’s fluid-filled spaces called ventricles. These changes can often be detected during pregnancy scans, particularly from the second trimester onwards.
Early detection of hydrocephalus relies on careful measurement of ventricular size and assessment of overall brain structure. While mild ventricular enlargement can sometimes be a normal variant, significant enlargement may indicate developing hydrocephalus.
When these findings are detected, additional monitoring scans may be recommended and genetic testing may be considered. Tests like NIPT, chorionic villus sampling (CVS), or amniocentesis may be suggested to rule out associated chromosomal abnormalities.
Enlarged lateral ventricles
The lateral ventricles appear abnormally enlarged on ultrasound, typically measuring more than 10mm in diameter. This is often the first and most obvious sign of developing hydrocephalus, visible as enlarged dark spaces within the brain tissue.
Increased head circumference
The fetal head appears disproportionately large compared to body size, with head circumference measurements consistently above the expected range for gestational age. This macrocephaly develops as increased brain pressure causes skull expansion.
Thinning of brain tissue
The cerebral cortex appears thinner than normal as increased fluid pressure compresses brain tissue against the skull. This can be seen on ultrasound as reduced thickness of the brain matter surrounding the enlarged ventricles.
Absent or compressed cisterna magna
The cisterna magna, a fluid-filled space at the back of the brain, may appear smaller than normal or absent due to altered cerebrospinal fluid dynamics. This finding often accompanies other signs of hydrocephalus.
Dangling choroid plexus
The choroid plexus, which normally fills much of the lateral ventricle, appears to hang freely within the enlarged ventricular space. This ‘dangling’ appearance is a classic ultrasound sign of significant ventricular dilatation.
Enlarged third ventricle
The third ventricle, located in the brain’s midline, appears wider than the normal narrow slit-like appearance. Enlargement of this structure often accompanies lateral ventricular dilatation in hydrocephalus.
Hydrocephalus is a medical condition characterised by an abnormal accumulation of cerebrospinal fluid (CSF) within the brain’s ventricles, causing them to enlarge. This clear, colourless fluid normally circulates around the brain and spinal cord, providing cushioning and delivering nutrients whilst removing waste products. In hydrocephalus, this normal circulation is disrupted, leading to fluid buildup and increased pressure within the skull.
The condition can be congenital (present from birth) or acquired (developing later due to infection, trauma, or other causes). During pregnancy, congenital hydrocephalus is the primary concern, potentially detectable through ultrasound scanning from the first trimester with advanced techniques.
Congenital hydrocephalus can result from several factors affecting fetal brain development. Genetic abnormalities may disrupt normal brain formation, whilst neural tube defects such as spina bifida can interfere with cerebrospinal fluid circulation. Infections during pregnancy, particularly toxoplasmosis, cytomegalovirus, or rubella, can also damage developing brain structures and lead to hydrocephalus.
Maternal factors including diabetes, pregnancy-induced hypertension, and certain medications can increase the risk of fetal brain abnormalities. Additionally, structural brain malformations such as aqueductal stenosis (narrowing of the passage between brain ventricles) can prevent normal fluid drainage, resulting in hydrocephalus.
Hydrocephalus can be diagnosed through ultrasound examination during pregnancy scans. The condition may be detected as early as the 10-week scan when severe abnormalities are present, or during later detailed scans when enlarged ventricles or increased head circumference become apparent. Sonographers measure ventricular width and assess overall brain structure to determine the severity of fluid accumulation.
If hydrocephalus is suspected, additional detailed scans and genetic testing may be recommended. Comprehensive anomaly scans can provide precise measurements and assessment, whilst genetic counselling can help families understand the implications and plan appropriate care.
Communicating hydrocephalus occurs when cerebrospinal fluid can flow between ventricles but is not properly absorbed, whilst non-communicating (obstructive) hydrocephalus results from blockages preventing fluid movement between brain compartments. The most common cause of non-communicating hydrocephalus is aqueductal stenosis, where the narrow passage connecting the third and fourth ventricles becomes blocked.
Mild, moderate, and severe classifications depend on the degree of ventricular enlargement and associated brain changes. Mild cases may remain stable throughout pregnancy and after birth, whilst severe hydrocephalus typically requires immediate postnatal surgical intervention to prevent brain damage.
Currently, there are no established prenatal treatments for hydrocephalus that are routinely recommended. Experimental procedures such as in-utero shunt placement have been attempted in research settings, but these carry significant risks and have not proven superior to postnatal treatment in most cases.
The primary focus during pregnancy is careful monitoring through regular ultrasound scans to assess progression and plan for delivery and immediate postnatal care. Multidisciplinary planning involving obstetricians, neonatologists, and paediatric neurosurgeons ensures the best possible outcomes for babies diagnosed with hydrocephalus.
The prognosis varies significantly depending on the severity of hydrocephalus, presence of associated abnormalities, and timing of treatment after birth. Many children with mild to moderate hydrocephalus who receive appropriate treatment can develop normally and lead fulfilling lives. Early intervention with surgical procedures such as shunt placement can prevent further brain damage and allow normal development.
Severe cases or those associated with other major abnormalities may have more challenging outcomes, potentially affecting cognitive development, motor skills, and requiring ongoing medical care. However, advances in neurosurgical techniques and supportive care continue to improve outcomes for affected children.
Hydrocephalus significantly impacts delivery planning due to potential complications from enlarged fetal head size. Severe macrocephaly (enlarged head) may prevent normal vaginal delivery, necessitating caesarean section to avoid birth trauma. The timing of delivery may also be adjusted based on the progression of hydrocephalus and overall fetal wellbeing.
Multidisciplinary care planning is essential, involving obstetricians, neonatologists, and paediatric neurosurgeons who can provide immediate postnatal assessment and intervention if required. Delivery should ideally occur at a specialist centre with paediatric neurosurgical facilities to ensure optimal care for the newborn.
Hydrocephalus can be associated with chromosomal abnormalities including trisomy 18, trisomy 13, and triploidy, though many cases occur in chromosomally normal fetuses. When hydrocephalus is detected, genetic testing may be offered to rule out underlying chromosomal causes and provide families with comprehensive information about their baby’s condition.
Genetic syndromes such as X-linked hydrocephalus may also be considered, particularly when there is a family history of the condition or if the fetus is male. Genetic counselling services can help families understand these associations and decide about appropriate testing.
Pregnancies complicated by fetal hydrocephalus require regular monitoring scans to assess the progression of ventricular enlargement and overall fetal wellbeing. These scans typically occur every 2-4 weeks, depending on the severity of the condition and rate of progression. Measurements of head circumference, ventricular size, and assessment of brain tissue thickness help guide care decisions.
Additional monitoring may include assessment of amniotic fluid levels, fetal growth, and screening for other associated abnormalities. Specialist monitoring scans can ensure comprehensive assessment throughout pregnancy to optimise outcomes for both mother and baby.
The recurrence risk for hydrocephalus in future pregnancies depends on the underlying cause. If the condition resulted from a chromosomal abnormality or genetic syndrome, there may be an increased risk of recurrence based on the specific inheritance pattern. For isolated hydrocephalus without an identified genetic cause, the recurrence risk is generally low but slightly higher than the general population risk.
Genetic counselling is valuable for families who have had a pregnancy affected by hydrocephalus, as it can provide personalised risk assessment based on family history and test results. Preconceptual counselling can discuss screening options and monitoring strategies for future pregnancies.
Receiving a diagnosis of fetal hydrocephalus can be overwhelming for families, and comprehensive support is available. Genetic counselling services can provide detailed information about the condition, its implications, and help families make informed decisions about their pregnancy and future family planning. Support groups and patient organisations can connect families with others who have similar experiences.
Multidisciplinary care teams including maternal-fetal medicine specialists, neonatologists, paediatric neurosurgeons, and social workers work together to provide comprehensive support throughout pregnancy and beyond. Early connection with paediatric specialists can help families prepare for their baby’s needs after birth.
Prenatal diagnosis of hydrocephalus is generally highly accurate when performed using modern ultrasound equipment with experienced practitioners. The detection rate is highest during the second and third trimesters when fetal brain structures are well-developed and ventricular enlargement becomes more apparent.
Mild cases may be more challenging to diagnose definitively, as borderline ventricular measurements can sometimes represent normal variation. Serial scans may be used to monitor progression and confirm the diagnosis, whilst additional imaging techniques such as fetal MRI may provide further detail in complex cases.
The primary treatment for hydrocephalus after birth is surgical intervention to divert excess cerebrospinal fluid and reduce brain pressure. The most common procedure involves placing a shunt system, typically from the brain ventricles to the abdomen, allowing fluid to drain and be absorbed naturally by the body.
Alternative procedures such as endoscopic third ventriculostomy may be suitable in some cases, creating a new pathway for fluid drainage within the brain itself. The choice of treatment depends on the type and severity of hydrocephalus, the child’s age, and other individual factors determined by the paediatric neurosurgical team.
Long-term developmental outcomes for children with hydrocephalus vary widely depending on the severity at diagnosis, effectiveness of treatment, and presence of associated conditions. Many children who receive prompt, appropriate treatment develop normally and achieve typical developmental milestones, attending mainstream schools and participating in normal childhood activities.
Some children may experience challenges with learning, coordination, or other developmental areas, requiring additional support and therapies. Regular follow-up with developmental specialists, physiotherapists, and educational support services helps optimise outcomes and address any difficulties as they arise.
If your baby is diagnosed with hydrocephalus, you can expect comprehensive care planning involving multiple specialists to ensure the best possible outcomes. This typically includes consultation with maternal-fetal medicine specialists, neonatologists, and paediatric neurosurgeons who will discuss treatment options and care plans for both pregnancy and after birth.
Immediate postnatal care often involves assessment by the neurosurgical team to determine if urgent intervention is needed. Many babies with hydrocephalus are born healthy and can await planned treatment, whilst others may require immediate surgical intervention. The care team will guide you through each step and ensure you have all the support and information needed.


