Acrania
Acrania is a rare but serious neural tube defect characterised by the complete or partial absence of the skull vault. This condition can be detected through detailed ultrasound scanning from early pregnancy, allowing for appropriate counselling and pregnancy management.
Acrania: Key Information
Acrania is a rare neural tube defect characterised by the complete or partial absence of the fetal skull vault, leaving the brain tissue exposed to amniotic fluid. This condition occurs during the early stages of fetal development, typically appearing during the fourth week of pregnancy. Unlike anencephaly, in acrania the brain tissue is initially present but unprotected by the skull bones. Acrania affects a small number of pregnancies and represents a serious developmental abnormality.
Early diagnosis of acrania can be made through detailed anomaly scanning from 11 weeks of gestation onwards, when skull ossification normally begins. Early pregnancy scans and advanced 3D/4D imaging may provide detailed assessment of fetal development and accurate identification of structural anomalies.
For more detailed information, visit our dedicated Acrania page.
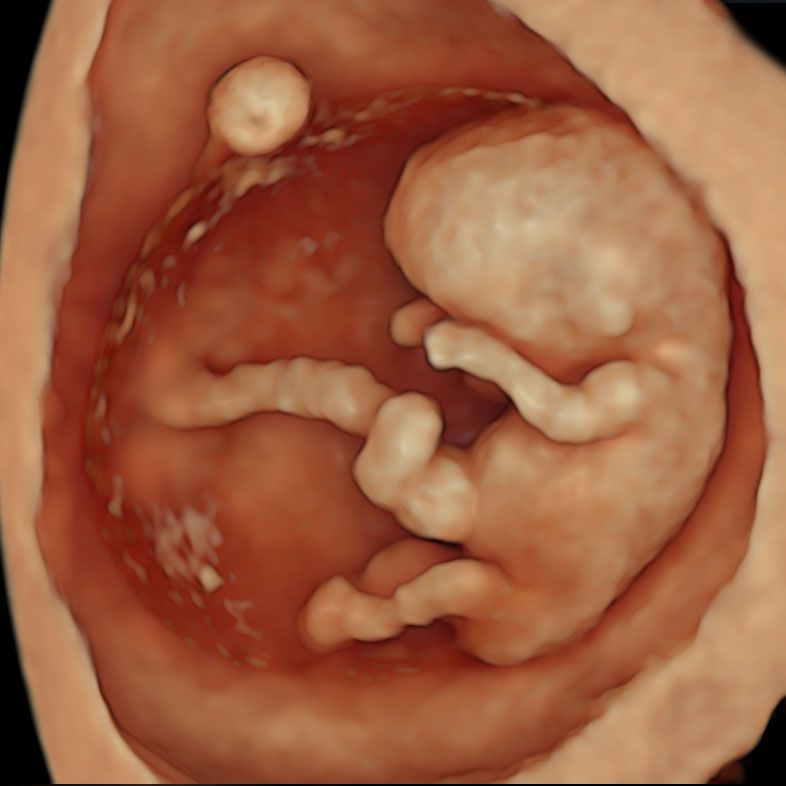
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Acrania statistics
-
Acrania is a rare neural tube defect
-
Chromosomal abnormalities in isolated acrania cases are rare
Investigations and support for acrania
Comprehensive anomaly scans are used to accurately identify acrania and assess for associated abnormalities. These detailed evaluations of fetal anatomy include assessment of the brain, spine, and other organ systems that may be affected. The characteristic absence of skull vault and distinctive ultrasound appearance allow confident diagnosis from 11 weeks of gestation.
Early detection through early fetal scans enables timely counselling and informed decision-making. Advanced imaging capabilities, including 3D/4D ultrasound, can provide clear visualisation of fetal structures and comprehensive assessment of the extent of the anomaly.
Following an acrania diagnosis, comprehensive genetic counselling is available to provide support and information about the condition, its implications, and available options. Both 30-minute and 60-minute genetic counselling sessions are available to address specific needs and concerns.
Genetic counselling sessions can discuss recurrence risks, provide information about neural tube defect prevention for future pregnancies, and offer ongoing emotional support. Families can receive accurate, up-to-date information to make informed decisions about their pregnancy and future family planning.
Given the potential for associated anomalies in acrania cases, detailed cardiac scanning can assess fetal heart structure and function. Specialist fetal echocardiography services are available to provide comprehensive evaluation of cardiovascular development from as early as 12 weeks of pregnancy.
Early cardiac assessment is particularly important as congenital heart defects may occur alongside neural tube defects. Detailed evaluation helps provide a complete picture of fetal health and informs ongoing pregnancy management decisions.
Following a diagnosis of acrania, a consultation with a fetal medicine consultant is available to help families understand the condition, its implications, and the options available. This specialist consultation provides detailed, personalised information about the diagnosis and what to expect.
Ongoing pregnancy monitoring and management is provided through the NHS pathway. A fetal medicine consultation can complement NHS care by offering additional time to discuss the diagnosis, ask questions, and receive guidance on next steps including referrals and support services.
Ultrasound scans can sometimes provide early clues
Ultrasound signs of acrania during pregnancy
Fetal anomalies linked to acrania may include various structural abnormalities affecting the central nervous system and other organ systems. The primary finding is absence of the skull vault with exposed brain tissue creating a characteristic appearance.
Ultrasound signs of acrania include specific anatomical features that can be identified through detailed scanning. The condition may present with additional soft markers or associated anomalies that require comprehensive evaluation.
When healthcare providers identify these findings, they may recommend additional testing. Tests like NIPT, chorionic villus sampling (CVS), or amniocentesis may be considered to assess for chromosomal abnormalities.
Absent Skull Vault
Complete or partial absence of the cranial bones forming the skull vault, with brain tissue directly exposed to amniotic fluid. This creates a characteristic ‘Mickey Mouse head’ appearance on ultrasound imaging.
Dorsally Bulging Brain
Protrusion of brain tissue through the absent skull vault, creating an abnormal contour of the fetal head. The brain tissue may appear to bulge posteriorly due to lack of bony protection.
Associated Spinal Defects
Spina bifida occurs in approximately 25% of acrania cases, involving incomplete closure of the spinal column. This may be visible as an open neural tube defect along the fetal spine.
Altered Cranial Measurements
Abnormal head circumference and biparietal diameter measurements due to absence of normal skull structure. Standard fetal biometry parameters may be significantly altered or unmeasurable.
Brain Tissue Degeneration
Progressive deterioration of exposed brain tissue due to contact with amniotic fluid, potentially leading to anencephaly in later pregnancy. Early brain tissue may initially appear normal but degrades over time.
Acrania is a rare neural tube defect characterised by the complete or partial absence of the skull vault, leaving the brain tissue exposed to amniotic fluid. Unlike anencephaly, where brain tissue is absent, in acrania the brain tissue is initially present but lacks the protective covering of skull bones. The condition occurs during early fetal development, typically appearing during the fourth week of pregnancy when neural tube closure should normally be complete.
This serious fetal anomaly is rare and requires immediate medical attention and counselling. The exposed brain tissue is vulnerable to damage from amniotic fluid, which may lead to progressive deterioration and potentially anencephaly if the pregnancy continues.
Acrania results from failure of the neural tube to close properly during early embryonic development, specifically affecting the formation of the skull vault. The exact cause is often unknown, but several risk factors have been identified including maternal folic acid deficiency, which is essential for proper neural tube development. Exposure to certain medications such as valproic acid, retinoic acid, and thalidomide during early pregnancy may increase the risk.
Environmental factors such as maternal alcohol consumption, poorly controlled diabetes, and obesity may also contribute to increased risk. Maternal age, particularly younger mothers, and certain genetic factors may play a role, though chromosomal abnormalities in isolated acrania cases are relatively rare according to research.
Acrania can be reliably diagnosed from 11 weeks of gestation onwards when normal skull ossification should begin to be visible on ultrasound. Detailed anomaly scans can accurately identify the absence of skull vault and assess for associated abnormalities. Early diagnosis enables appropriate counselling and pregnancy management.
The characteristic ‘Mickey Mouse head’ appearance on ultrasound, caused by absent cranial bones and dorsally bulging brain tissue, allows for confident diagnosis. Advanced 3D/4D ultrasound imaging can provide additional detail and help families understand the extent of the condition.
The key ultrasound features include absent skull vault and dorsally bulging brain tissue, creating the characteristic ‘Mickey Mouse head’ appearance. The brain tissue appears to protrude through the absent cranial bones, and normal head measurements cannot be obtained due to the lack of skull structure. Associated spinal abnormalities, particularly spina bifida, are found in approximately 25% of cases.
Other ultrasound findings may include altered amniotic fluid levels and abnormal fetal positioning. The brain tissue may show signs of degeneration over time due to exposure to amniotic fluid, and additional structural abnormalities affecting other organ systems should be carefully assessed.
Acrania is typically not inherited and usually occurs as an isolated developmental abnormality during early pregnancy. Chromosomal defects in isolated acrania cases are rare according to research, and most cases represent sporadic neural tube defects rather than genetic conditions. However, there may be a slightly increased risk of recurrence in future pregnancies.
Families with a history of neural tube defects may benefit from genetic counselling to discuss recurrence risks and prevention strategies. Proper folic acid supplementation before conception and during early pregnancy can significantly reduce the risk of neural tube defects in future pregnancies.
The prognosis for acrania is unfortunately very poor, with the condition being incompatible with long-term survival. Most affected pregnancies result in pregnancy loss, and babies born with acrania typically survive only hours to days after birth. The exposed brain tissue progressively deteriorates due to contact with amniotic fluid, often leading to anencephaly.
There is no cure or treatment available for acrania, and the condition represents a lethal fetal anomaly. Families facing this diagnosis require compassionate counselling and support to make informed decisions about their pregnancy and future family planning.
Acrania significantly impacts pregnancy outcomes, with most affected pregnancies ending in miscarriage or stillbirth. The condition may be associated with polyhydramnios (excess amniotic fluid) due to impaired fetal swallowing. Maternal health is generally not directly affected by the fetal condition, but emotional support is crucial given the serious implications.
Regular monitoring through ultrasound scanning can assess fetal wellbeing and detect any additional complications. Families may choose various management options including continuing the pregnancy with palliative care planning or pregnancy termination, depending on their personal circumstances and beliefs.
Several screening options are available to help identify increased risk for neural tube defects including acrania. Nuchal scans performed between 11-13 weeks can identify structural abnormalities and assess overall fetal development. Maternal serum alpha-fetoprotein (AFP) screening may show elevated levels in neural tube defects.
Detailed ultrasound examination remains the primary diagnostic tool, with specialist anomaly scans providing comprehensive assessment of fetal anatomy. While NIPT screening focuses on chromosomal conditions, it may be considered to rule out additional genetic abnormalities in affected pregnancies.
While acrania cannot be completely prevented, the risk can be significantly reduced through proper preconceptional care and folic acid supplementation. Taking 400 micrograms of folic acid daily before conception and during the first 12 weeks of pregnancy helps prevent neural tube defects. Women with increased risk may require higher doses of 5mg daily.
Avoiding known risk factors such as certain medications, alcohol, and ensuring good diabetic control before pregnancy can help reduce risk. Maintaining a healthy weight and avoiding exposure to environmental toxins during early pregnancy are also important preventive measures.
Comprehensive support is available for families facing an acrania diagnosis, including detailed genetic counselling, emotional support, and practical guidance. Counselling services can provide information about the condition, discuss available options, and offer ongoing support throughout the decision-making process.
Coordination with specialist fetal medicine units, maternal mental health services, and support organisations can ensure families receive comprehensive care. Bereavement counselling and support groups may be beneficial for families coping with pregnancy loss or neonatal death.
Acrania diagnosis through ultrasound is highly accurate when performed by experienced sonographers using modern equipment. The characteristic absence of skull vault and distinctive appearance make confident diagnosis possible from 11 weeks of gestation. Specialist scanning services can provide detailed assessment and accurate diagnosis of this condition.
Confirmation of diagnosis may involve multiple scans and assessment by fetal medicine specialists to ensure accuracy and evaluate for associated abnormalities. The distinct ultrasound features of acrania make misdiagnosis rare when proper protocols are followed.
Following acrania diagnosis, immediate counselling and support are available to help families understand the condition and available options. Detailed assessment for associated abnormalities can be performed, including evaluation of the spine, heart, and other organ systems. Referral to specialist fetal medicine services may be arranged for comprehensive care.
Families receive information about pregnancy management options, including palliative care planning if continuing the pregnancy or pregnancy termination procedures if that choice is made. Ongoing psychological support and counselling are available throughout the process, with planning for future pregnancies including prevention strategies.
Acrania may present as complete or partial absence of the skull vault, with varying degrees of brain tissue exposure. The condition may be isolated or associated with other neural tube defects such as spina bifida in approximately 25% of cases. Some cases may progress from acrania to exencephaly (herniated brain) and eventually anencephaly due to brain tissue degeneration.
The extent of skull absence and degree of brain exposure can vary between cases, but all forms represent serious developmental abnormalities with similar prognosis. Comprehensive ultrasound assessment helps determine the specific features and extent of the condition in each individual case.
Future pregnancies require careful planning and increased surveillance following an acrania diagnosis. High-dose folic acid supplementation (5mg daily) is recommended before conception and during early pregnancy to reduce recurrence risk. Preconceptional counselling helps optimise maternal health and discuss prevention strategies.
Early detailed ultrasound scanning in subsequent pregnancies allows for prompt identification of any neural tube defects. The recurrence risk is slightly increased compared to the general population, but most families can expect normal outcomes in future pregnancies with appropriate care and monitoring.
Acrania and anencephaly represent different stages of the same developmental process. In acrania, the skull vault is absent but brain tissue is initially present, whereas in anencephaly, both skull and brain tissue are absent or severely malformed. Acrania may progress to anencephaly during pregnancy as exposed brain tissue degenerates from contact with amniotic fluid.
Both conditions result from neural tube defects and have similar causes and risk factors. The prognosis remains equally poor for both conditions, as both are incompatible with long-term survival. Early diagnosis allows for appropriate counselling regardless of the specific terminology used.
Folic acid plays a crucial role in neural tube development and proper supplementation can reduce the risk of acrania and other neural tube defects by up to 70%. The standard recommendation is 400 micrograms daily before conception and during the first 12 weeks of pregnancy. Women with increased risk factors may require higher doses of 5mg daily.
Folic acid is essential for DNA synthesis and cell division during rapid embryonic development. Deficiency during the critical period of neural tube closure (typically around 4 weeks of pregnancy) can increase the risk of developmental abnormalities. Food fortification with folic acid has significantly reduced neural tube defect rates in many countries.
This page was created using information from the following trusted medical sources:


