Sirenomelia
Sirenomelia, also known as mermaid syndrome, is an extremely rare congenital condition that can be detected through prenatal ultrasound examination. This complex developmental disorder affects multiple organ systems and comprehensive assessment and support services are available for affected families.
Sirenomelia: Key Information
Sirenomelia, commonly known as mermaid syndrome, is an extremely rare congenital condition characterised by partial or complete fusion of both legs. This severe developmental anomaly affects multiple organ systems, including the spine, pelvis, genitourinary tract, and gastrointestinal system. The condition occurs sporadically with no increased risk in subsequent pregnancies, and most cases are incompatible with life. Sirenomelia affects approximately 1 in 60,000 to 100,000 pregnancies worldwide — the live birth prevalence is considerably lower as many affected pregnancies do not reach term.
Prenatal diagnosis of sirenomelia can be made through detailed ultrasound examination as early as the first trimester. The condition can be screened during the 10-week scan or through comprehensive anomaly scans, allowing families to access appropriate support services and make informed decisions. Additional assessment through third trimester anomaly scans can provide ongoing fetal evaluation, whilst specialist genetic counselling is available to offer guidance and emotional support throughout the diagnostic process.
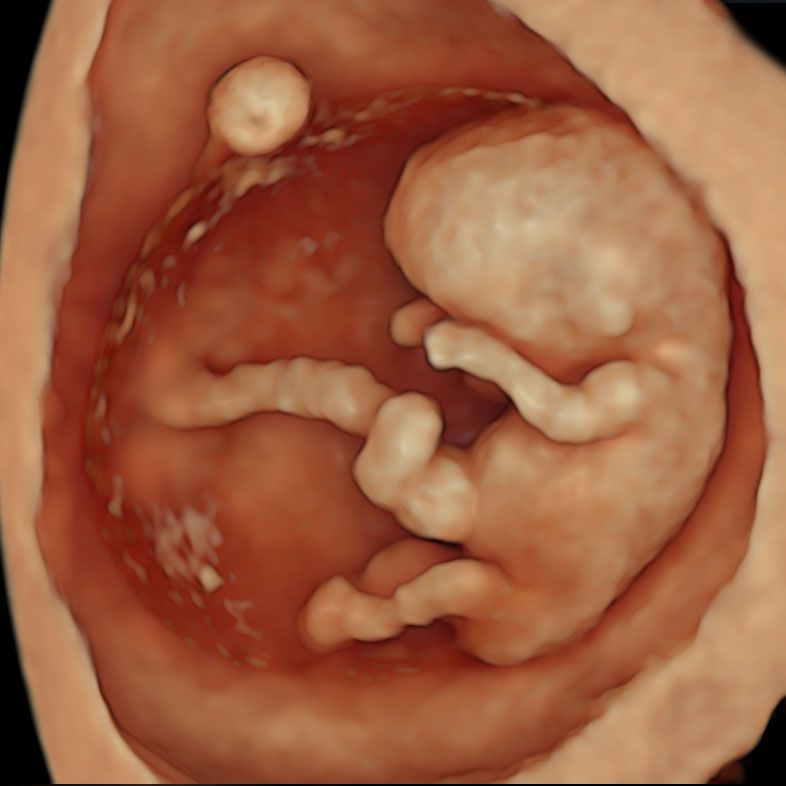
Early pregnancy scans can often exclude over 100 severe fetal abnormalities
Sirenomelia statistics
-
Sirenomelia affects approximately 1 in 60,000-100,000 pregnancies worldwide
-
Most affected pregnancies result in stillbirth or death shortly after delivery
Investigations and support for sirenomelia
Detailed anomaly scans use advanced ultrasound technology to assess fetal development between 18-22 weeks of pregnancy. These examinations can identify the characteristic features of sirenomelia, including limb fusion, spinal abnormalities, and associated organ defects.
Early detection through comprehensive scanning allows families to access appropriate support services and make informed decisions. Specialist referrals can be arranged when complex conditions like sirenomelia are suspected, providing access to further assessment and management options.
Sirenomelia may be identifiable from the first trimester through detailed ultrasound assessment. The 10-week scan includes a structural survey that can detect limb abnormalities and associated features of sirenomelia, whilst nuchal translucency screening can identify other early developmental concerns.
Early detection provides families with more time to access appropriate counselling and support services. Further detailed assessment through the anomaly scan at 18-22 weeks can provide comprehensive evaluation of all associated features.
Given the association between sirenomelia and cardiac abnormalities, specialist cardiac scanning provides detailed evaluation of fetal heart structure and function. This assessment is important as congenital heart defects frequently accompany sirenomelia.
Fetal echocardiography services offer detailed cardiac evaluation from 12 weeks of pregnancy, allowing detection of associated heart abnormalities. This specialised imaging helps provide a complete picture of the condition’s impact on fetal development.
When sirenomelia is diagnosed, genetic counselling services provide support to help families understand the condition, its implications, and available options. Genetic counselling sessions offer detailed discussion of the condition’s sporadic nature and lack of increased recurrence risk.
Ongoing emotional support and practical guidance are available throughout the pregnancy journey, helping families navigate complex medical decisions. Counsellors can work with specialist medical teams to ensure families receive comprehensive, coordinated care during this challenging time.
Advanced 3D/4D scanning technology can provide detailed visualisation of fetal limb development and spinal structure, offering enhanced assessment of sirenomelia features. This imaging may help provide families with clearer understanding of the condition’s physical manifestations.
Three-dimensional imaging can reveal the extent of limb fusion and associated skeletal abnormalities with greater clarity than traditional 2D ultrasound. This detailed visualisation supports accurate diagnosis and helps in planning for potential postnatal care requirements.
Ultrasound scans can sometimes provide early clues
Ultrasound signs of sirenomelia during pregnancy
Fetal anomalies associated with sirenomelia typically involve multiple organ systems and can be detected through detailed ultrasound examination. The condition is characterised by fusion of the lower limbs along with various internal abnormalities affecting the spine, pelvis, and organ systems.
Ultrasound features of sirenomelia are usually evident during routine anomaly scanning in the second trimester. The characteristic appearance of fused lower limbs, combined with associated abnormalities, typically allows for definitive diagnosis during pregnancy.
When these findings are identified, additional assessment and counselling may be recommended. Comprehensive evaluation through detailed anomaly scanning and genetic counselling services can be arranged.
Fused Lower Limbs
The hallmark feature of sirenomelia is partial or complete fusion of both legs, creating a single limb structure. This characteristic appearance gives the condition its common name of ‘mermaid syndrome’ and is typically clearly visible on ultrasound examination from the second trimester onwards.
Spinal Defects
Abnormalities of the lower spine and sacral region are commonly associated with sirenomelia. These may include absent or underdeveloped vertebrae in the lower spine, which can be identified through careful ultrasound assessment of the fetal skeletal system.
Severe Oligohydramnios
Severely reduced amniotic fluid levels often accompany sirenomelia due to associated kidney abnormalities and impaired fetal urine production. This finding may be one of the first indicators that prompts detailed fetal assessment during routine scanning.
Renal Agenesis
Absence of one or both kidneys is frequently associated with sirenomelia and contributes to the poor prognosis of the condition. The kidneys may be completely absent or severely underdeveloped, leading to complications with amniotic fluid production and fetal development.
Pelvic Abnormalities
Structural abnormalities of the pelvis are commonly seen in sirenomelia, often including underdevelopment or fusion of pelvic bones. These changes are closely associated with the characteristic limb fusion and can be identified through detailed ultrasound examination.
Genitourinary Defects
Abnormalities of the internal and external genitalia are frequently present, including absent or underdeveloped reproductive organs. The bladder may also be absent or severely underdeveloped, contributing to the overall poor prognosis of the condition.
Gastrointestinal Anomalies
Defects of the gastrointestinal system, including imperforate anus or rectal atresia, are commonly associated with sirenomelia. These abnormalities affect the normal development of the lower digestive tract and contribute to the complex nature of the condition.
Single Umbilical Artery
The presence of only one umbilical artery instead of the normal two may be detected in some cases of sirenomelia. This vascular abnormality can be identified during routine ultrasound examination and may indicate increased risk of associated anomalies.
Sirenomelia, also known as mermaid syndrome, is an extremely rare congenital condition characterised by partial or complete fusion of both legs. The condition affects approximately 1 in 60,000 to 100,000 pregnancies worldwide and involves abnormalities of multiple organ systems including the spine, pelvis, kidneys, and gastrointestinal tract. Most cases occur sporadically with no identifiable cause.
The condition is typically incompatible with life, with most affected pregnancies resulting in stillbirth or death shortly after delivery. The poor prognosis is largely due to associated kidney abnormalities and severe oligohydramnios (reduced amniotic fluid), which affect normal fetal development and lung maturation.
The exact cause of sirenomelia remains unknown, though several theories have been proposed. Most cases occur sporadically with no identifiable genetic or environmental cause. Research suggests that abnormal development of blood vessels in the lower part of the developing embryo may play a role, leading to inadequate blood supply to the lower limbs and associated structures.
Maternal diabetes has been identified as a potential risk factor, with approximately 2% of mothers of affected pregnancies having diabetes. However, the vast majority of cases occur in pregnancies without any known risk factors, and the condition does not typically recur in subsequent pregnancies.
Sirenomelia can be detected as early as the first trimester through detailed ultrasound examination. Early structural assessment during the 10-week scan can identify features of the condition, whilst anomaly scanning between 18-22 weeks gestation typically allows for more comprehensive evaluation. The characteristic fusion of the lower limbs, combined with associated features such as severe oligohydramnios and kidney abnormalities, usually allows for definitive diagnosis.
Early detection enables families to access appropriate counselling and support services promptly, allowing time for informed decision-making and planning of care.
The primary feature of sirenomelia is fusion of both legs, which may be partial or complete. Associated abnormalities commonly include spinal defects affecting the lower spine and sacrum, pelvic abnormalities, and severe kidney problems including renal agenesis (absent kidneys). Gastrointestinal defects such as imperforate anus or rectal atresia are also frequently present.
Internal abnormalities affecting the genitourinary system are common, including absent or underdeveloped reproductive organs and bladder. These multiple system abnormalities contribute to the serious nature of the condition and its typically poor prognosis.
Sirenomelia is not typically hereditary and occurs sporadically in most cases. There is no increased risk of recurrence in subsequent pregnancies, as the condition is not usually caused by genetic factors that can be passed from parents to children. Most cases represent isolated developmental accidents during early embryonic development.
However, given the complexity of the condition, families may benefit from genetic counselling to discuss the specific circumstances of their case and address any concerns about future pregnancies. Professional counselling can provide personalised risk assessment and support.
Unfortunately, the prognosis for babies with sirenomelia is typically very poor. Most affected pregnancies result in stillbirth or death shortly after delivery due to the severe associated abnormalities, particularly kidney problems and underdeveloped lungs. The absence or severe underdevelopment of kidneys leads to oligohydramnios, which affects normal lung development and is incompatible with survival.
In extremely rare cases where some kidney function is preserved, intensive medical and surgical intervention may be attempted, but the overall survival rate remains very low. The complex nature of the multiple system abnormalities makes successful treatment extremely challenging.
Sirenomelia significantly affects pregnancy due to associated severe oligohydramnios (reduced amniotic fluid levels). This occurs because the fetal kidneys, which are often absent or severely underdeveloped, cannot produce normal amounts of urine to maintain adequate amniotic fluid levels. Oligohydramnios can lead to complications including poor fetal growth and lung development problems.
The condition requires careful monitoring throughout pregnancy with regular ultrasound assessments. Wellbeing scans can be used to monitor fetal development and amniotic fluid levels to assess the pregnancy’s progress.
Following a diagnosis of sirenomelia, comprehensive emotional and practical support is available for affected families. Genetic counselling services provide detailed information about the condition, discuss all available options, and offer ongoing emotional support throughout the decision-making process. Care coordination with other healthcare providers can ensure comprehensive support.
Support may include referral to specialist fetal medicine units, connection with appropriate support groups, and provision of resources to help families understand and cope with the diagnosis. Healthcare teams can provide ongoing guidance and support throughout the pregnancy journey.
Unfortunately, there are no effective treatments available during pregnancy to correct sirenomelia or its associated abnormalities. The condition involves fundamental structural abnormalities that develop early in embryonic development and cannot be reversed or corrected through prenatal intervention.
Management during pregnancy focuses on careful monitoring, family support, and planning for delivery. This may include discussions about delivery location and arrangements for immediate postnatal care, though the overall prognosis remains very poor regardless of interventions attempted.
Prenatal diagnosis of sirenomelia is typically highly accurate when performed during detailed ultrasound examination. The characteristic fusion of the lower limbs, combined with associated features such as severe oligohydramnios and kidney abnormalities, usually allows for definitive diagnosis during routine screening.
Detailed ultrasound assessment can provide accurate diagnosis from early pregnancy onwards. Additional imaging or consultation with fetal medicine specialists may be arranged if needed to confirm the diagnosis and assess the full extent of associated abnormalities.
During an ultrasound assessment for suspected sirenomelia, a comprehensive evaluation of fetal anatomy is performed, paying particular attention to the lower limbs, spine, kidneys, and amniotic fluid levels. The examination includes detailed assessment of limb structure, spinal development, organ formation, and overall fetal wellbeing.
The scan typically takes longer than routine examinations to ensure all aspects of fetal development are thoroughly assessed. Healthcare providers can explain findings as the examination proceeds and ensure families understand what is being evaluated and why additional assessment may be needed.
Yes, sirenomelia can be classified based on the degree of limb fusion and associated skeletal abnormalities. Classifications range from less severe forms where the legs are fused but separate feet may be present, to more severe forms with complete fusion into a single limb structure. The extent of fusion often correlates with the severity of associated internal abnormalities.
Different classification systems exist in the medical literature, but all forms of sirenomelia involve significant developmental abnormalities that affect multiple organ systems. The specific type and extent of abnormalities can usually be determined through detailed ultrasound examination.
Sirenomelia is distinct from other limb abnormalities due to its specific pattern of lower limb fusion combined with characteristic associated abnormalities affecting the spine, kidneys, and other organ systems. Unlike isolated limb defects, sirenomelia represents a complex developmental syndrome with multiple system involvement and typically poor prognosis.
The condition was previously thought to be related to caudal regression syndrome, but recent research has confirmed these are distinct conditions with different developmental mechanisms and patterns of abnormality. Accurate diagnosis is important for appropriate counselling and management.
Receiving a diagnosis of sirenomelia can be extremely distressing for families, and comprehensive emotional support is available. Genetic counselling services provide not only medical information but also emotional support and counselling throughout the diagnostic process and beyond. The impact such a diagnosis can have on families is recognised and compassionate, individualised care is available.
Support may include referral to counsellors, connection with support groups for families affected by fetal abnormalities, and provision of resources to help families cope with their situation. Healthcare teams can provide ongoing support and facilitate referrals to additional support services as needed.
Currently, there are no known preventive measures for sirenomelia, as the exact cause of the condition remains unknown and most cases occur sporadically. General measures that promote healthy pregnancy, such as taking folic acid supplements, maintaining good diabetic control if diabetic, and avoiding harmful substances, are always recommended but do not specifically prevent sirenomelia.
Since the condition typically occurs as an isolated developmental accident during early embryonic development, and does not usually recur in subsequent pregnancies, specific prevention strategies are not available. Families can be reassured that nothing they did or did not do caused the condition to occur.
If sirenomelia is diagnosed later in pregnancy, the focus shifts to delivery planning and postnatal care arrangements. While the overall prognosis remains very poor regardless of when diagnosis is made, late diagnosis requires careful planning to ensure appropriate support and resources are available for the family during delivery and the immediate postnatal period.
Late diagnosis may occur if earlier scans were limited by technical factors or if the pregnancy was not routinely monitored. Healthcare teams can provide support and guidance even when diagnosis occurs later in pregnancy, helping families understand their situation and access appropriate care and support services.
Sirenomelia has a significantly higher prevalence in monozygotic (identical) twins, occurring 100-150 times more frequently compared to singleton pregnancies. This increased risk may be related to vascular sharing between twins or other factors specific to monozygotic twinning, though the exact mechanisms remain unclear.
When sirenomelia occurs in twin pregnancies, it typically affects only one twin, creating additional challenges for management and decision-making. Families in this situation require counselling and support to understand the implications for both babies and make informed decisions about their pregnancy.
Research into sirenomelia continues to focus on understanding the underlying developmental mechanisms that lead to the condition. Studies are investigating the role of vascular development abnormalities, genetic factors, and environmental influences in the development of sirenomelia. Improved understanding of these mechanisms may eventually lead to better prevention or treatment strategies.
Current research also focuses on improving early diagnosis and developing better support strategies for affected families. While treatment options remain extremely limited due to the fundamental nature of the developmental abnormalities, ongoing research continues to provide important insights into this rare condition.
Management of sirenomelia varies between healthcare systems but typically involves multidisciplinary care coordination between fetal medicine specialists, genetic counsellors, neonatologists, and other relevant specialists. In the UK, care is usually coordinated through fetal medicine units within the NHS, with additional support available through private clinics for families seeking more personalised care or additional opinions.
Healthcare providers can work together with NHS specialists and other healthcare providers to ensure families receive comprehensive, well-coordinated care throughout their journey. This collaborative approach ensures that all aspects of diagnosis, counselling, and support can be addressed effectively.
Important questions to ask include: What is the certainty of the diagnosis, what associated abnormalities have been identified, what does this mean for the current pregnancy, and what support services are available? You may also want to ask about the implications for future pregnancies, what delivery planning is needed, and what resources are available to help you understand and cope with the diagnosis.
Genetic counselling services can help families formulate questions and provide information tailored to each family’s specific situation. Healthcare teams can ensure that all concerns are addressed and that families feel supported throughout their journey with this challenging diagnosis.


