HyCoSy vs HSG: Which Fallopian Tube Test Is Right for You

HyCoSy vs HSG: Which Fallopian Tube Test Is Right for You
Published
Tags
Fertility investigations affect approximately 1 in 7 couples in the UK, and understanding which fallopian tube test is most suitable for your circumstances can be crucial for your journey towards conception. Two primary diagnostic procedures, HyCoSy and HSG, offer different approaches to assessing fallopian tube patency and uterine health, each with distinct advantages and considerations that may influence your choice.
Understanding Fallopian Tube Testing
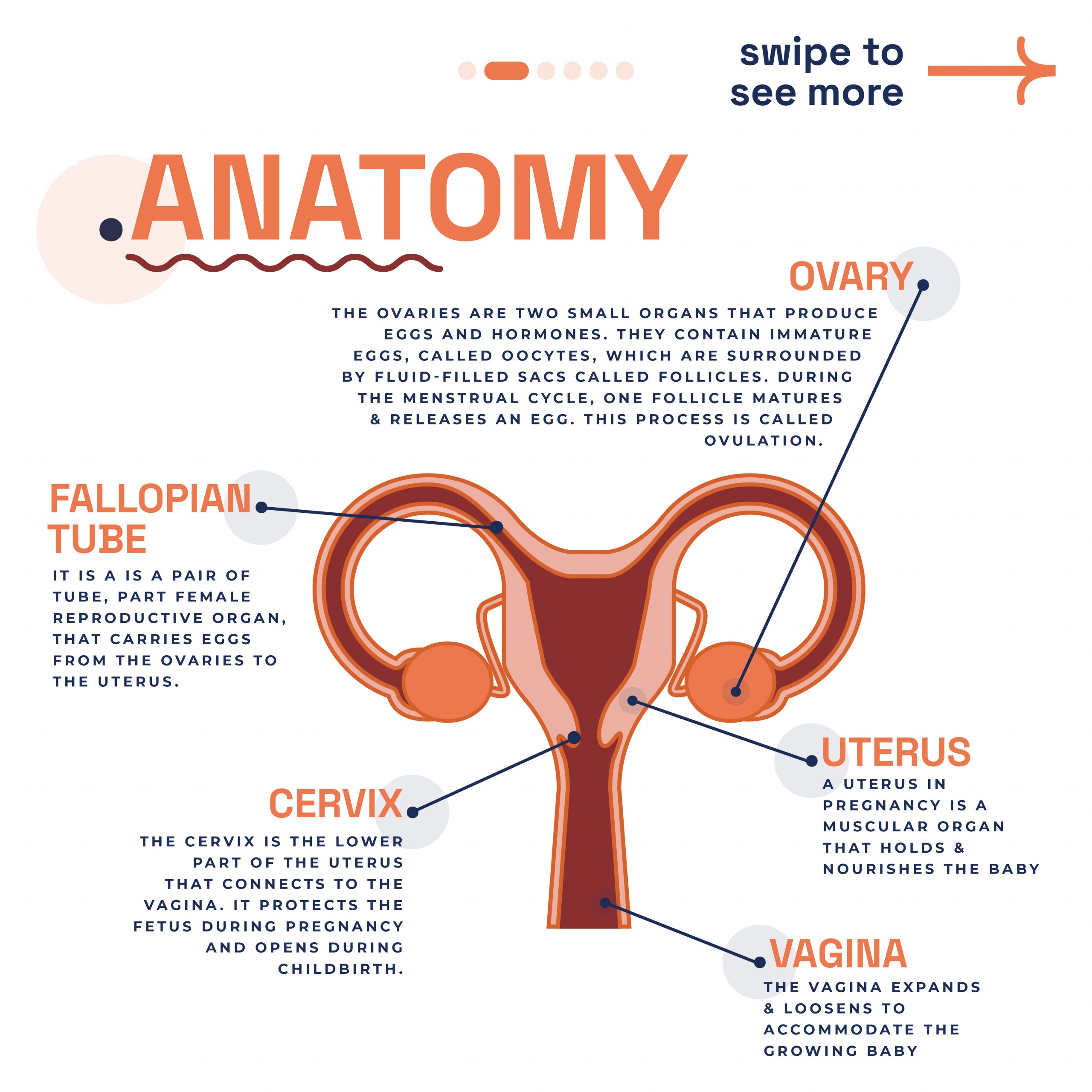
Fallopian tube testing forms an essential component of fertility assessment, helping clinicians identify potential blockages or abnormalities that may prevent conception. These diagnostic procedures evaluate whether eggs can travel freely from the ovaries through the fallopian tubes to reach the uterus, where fertilisation and implantation occur.
The two most commonly used non-surgical methods are HyCoSy (Hysterosalpingo-Contrast Sonography) and HSG (Hysterosalpingography). Both procedures involve introducing contrast medium into the reproductive system to visualise the internal structures, but they utilise different imaging technologies to achieve this assessment.
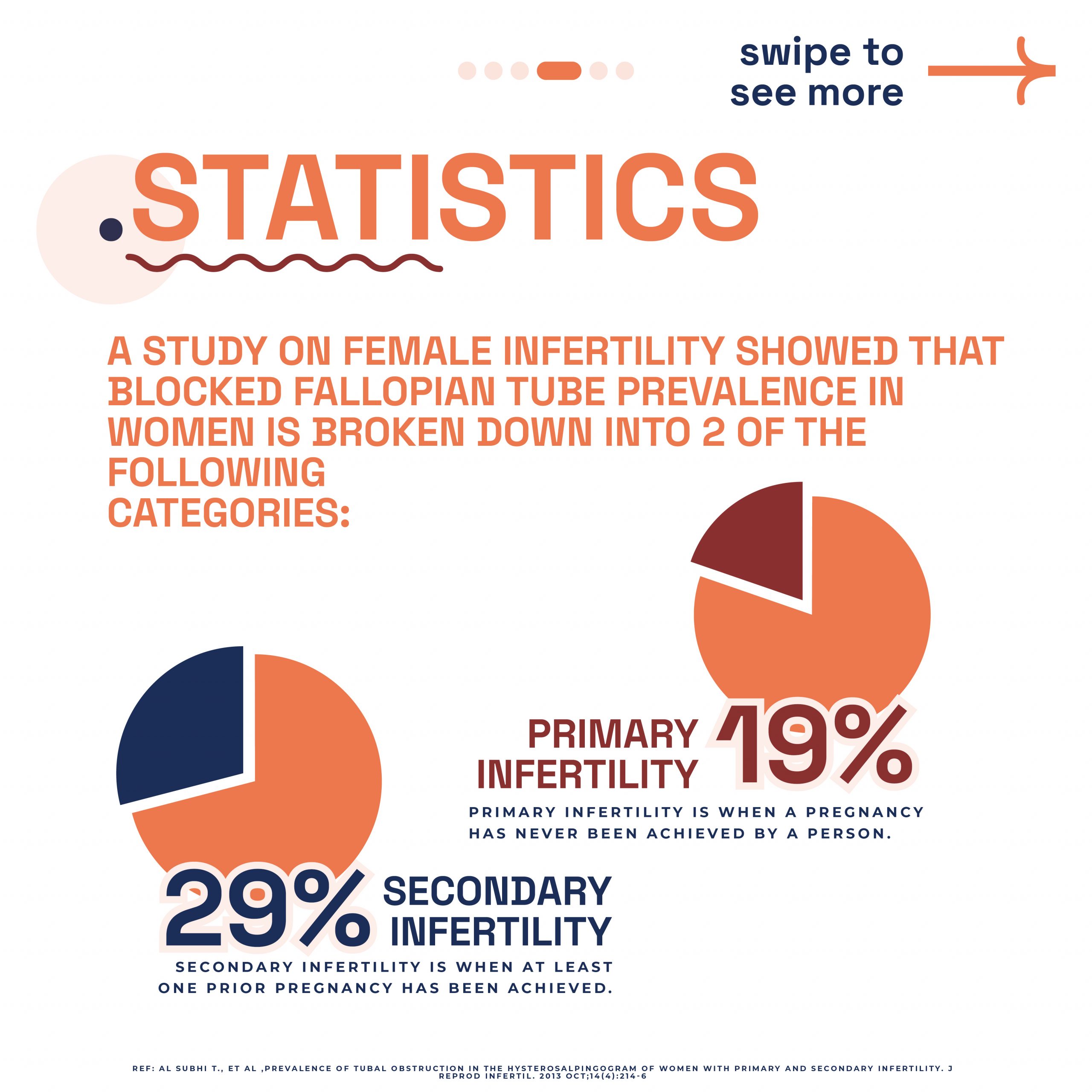
According to NHS guidelines, tubal factor infertility accounts for approximately 25-35% of female fertility issues, making accurate assessment of fallopian tube function vital for developing appropriate treatment plans.
What is HyCoSy
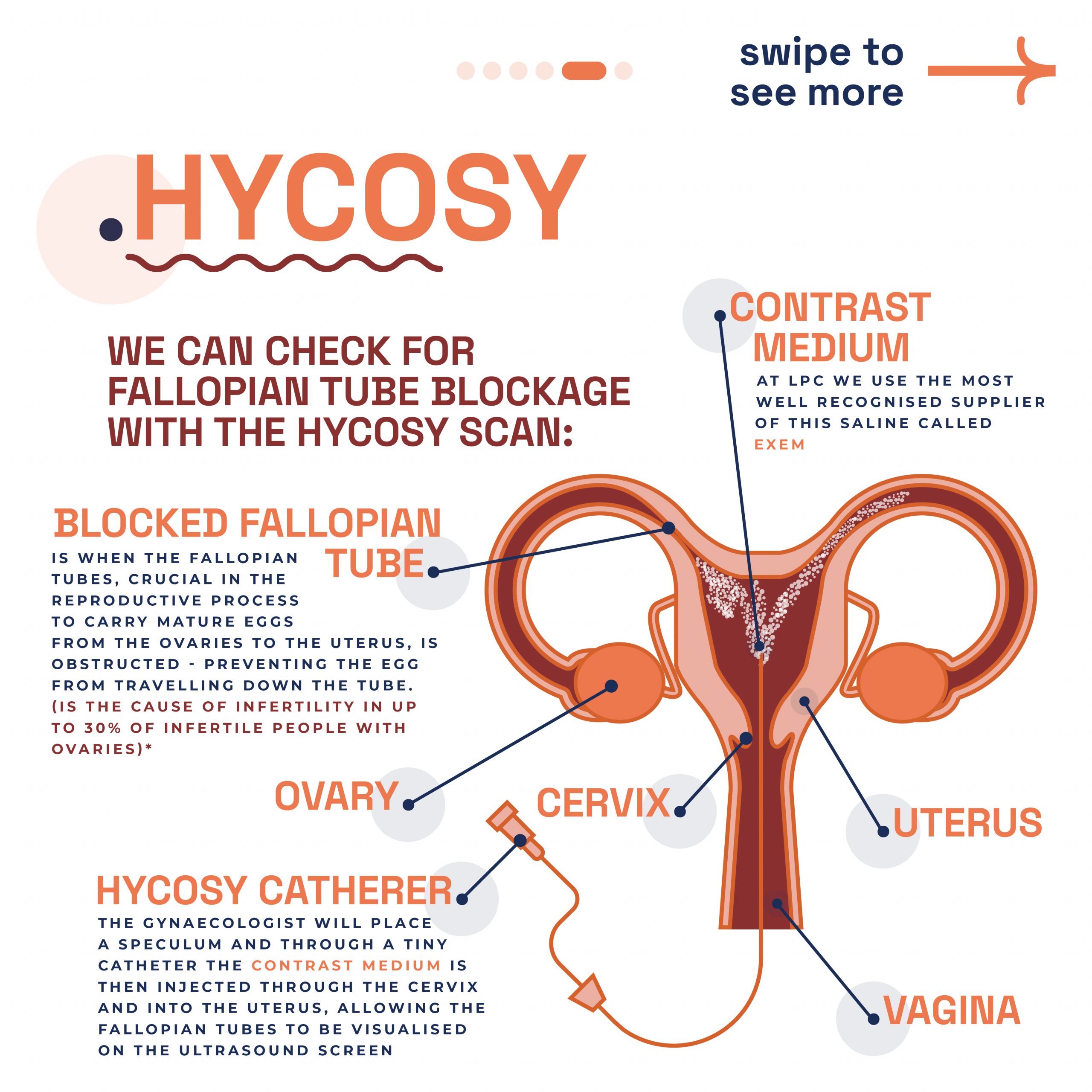
HyCoSy, or Hysterosalpingo-Contrast Sonography, represents a modern ultrasound-based approach to fallopian tube assessment. During this procedure, a specialised contrast medium is introduced through the cervix into the uterine cavity whilst real-time ultrasound monitoring captures detailed images of the reproductive organs.
The HyCoSy procedure utilises high-frequency sound waves to create detailed visualisations of both the uterine cavity and fallopian tubes. The contrast medium appears bright white on the ultrasound screen, allowing clinicians to observe its flow through the reproductive system and identify any areas of blockage or abnormal anatomy.
This technique offers the advantage of being radiation-free, making it particularly suitable for women who prefer to avoid X-ray exposure or who may require repeated assessments during their fertility journey.
What is HSG
HSG, or Hysterosalpingography, represents the traditional gold standard for fallopian tube assessment, utilising X-ray technology to visualise the reproductive organs. During this procedure, a radio-opaque contrast dye is introduced into the uterine cavity through the cervix, with X-ray images captured to show the dye’s progression through the fallopian tubes.
The HSG procedure provides excellent image quality and has been extensively studied and validated over decades of clinical use. The X-ray images offer exceptional detail of the uterine cavity shape and can clearly demonstrate whether the fallopian tubes are patent (open) or blocked.
HSG has traditionally been considered the first-line investigation for tubal patency assessment in many fertility clinics, with extensive research supporting its accuracy and reliability in diagnosing various reproductive conditions.
Key Differences Between HyCoSy and HSG
Understanding the fundamental differences between these two procedures can help you make an informed decision about which test may be most appropriate for your circumstances:
- Imaging Technology: HyCoSy uses ultrasound waves whilst HSG employs X-ray radiation to create images of the reproductive organs.
- Radiation Exposure: HyCoSy involves no radiation exposure, whereas HSG uses a controlled amount of ionising radiation.
- Real-time Monitoring: HyCoSy provides real-time visualisation during the procedure, allowing immediate assessment of contrast flow.
- Contrast Medium: HyCoSy uses specialised ultrasound contrast agents, whilst HSG employs radio-opaque dye visible on X-ray.
- Procedure Duration: Both procedures typically take 15-30 minutes, though HyCoSy may be slightly quicker due to real-time imaging capabilities.
- Equipment Requirements: HyCoSy requires specialised ultrasound equipment, whilst HSG needs X-ray facilities and fluoroscopy capabilities.
Research indicates that both procedures demonstrate comparable accuracy in detecting tubal blockages, with studies showing similar sensitivity and specificity rates for identifying fallopian tube abnormalities.
Advantages of HyCoSy
HyCoSy offers several compelling advantages that make it an attractive option for many women undergoing fertility assessment:
- No Radiation Exposure: The absence of ionising radiation makes HyCoSy suitable for women who wish to avoid X-ray exposure or require multiple assessments.
- Real-time Assessment: Immediate visualisation allows clinicians to observe contrast flow dynamics and make instant assessments during the procedure.
- Comfortable Environment: The procedure can be performed in a standard ultrasound room rather than requiring specialised X-ray facilities.
- Detailed Ovarian Assessment: Ultrasound technology allows simultaneous evaluation of ovarian morphology and other pelvic structures.
- Reduced Contrast Requirements: Often requires smaller volumes of contrast medium compared to HSG procedures.
- Immediate Discussion: Results can be discussed immediately after the procedure, reducing anxiety and waiting times.
Clinical studies have demonstrated that HyCoSy provides excellent visualisation of uterine cavity abnormalities and can effectively identify both proximal and distal tubal blockages with high accuracy rates.
Advantages of HSG
Despite being the more traditional approach, HSG continues to offer distinct advantages in certain clinical situations:
- Established Gold Standard: Decades of clinical use and extensive research validation support HSG’s reliability and accuracy.
- Superior Image Quality: X-ray technology often provides exceptional detail of uterine cavity shape and tubal anatomy.
- Widely Available: HSG facilities are commonly available in most hospitals and fertility centres across the UK.
- Detailed Documentation: X-ray images provide permanent, high-quality records for future reference and specialist consultations.
- Cost-Effective: HSG may be slightly more cost-effective in some healthcare settings due to established protocols and equipment.
- Therapeutic Benefits: Some studies suggest that HSG may have mild therapeutic effects, potentially improving conception rates in certain cases.
The RCOG recognises HSG as an effective method for assessing tubal patency, with guidelines supporting its use as part of comprehensive fertility investigations when clinically appropriate.
Potential Disadvantages and Considerations
Both procedures have specific limitations and considerations that may influence your decision:
HyCoSy Considerations:
- Operator Dependency: Results may vary depending on the sonographer’s experience and expertise with the technique.
- Image Quality Limitations: Ultrasound images may be affected by patient factors such as body habitus or bowel gas.
- Specialised Equipment: Requires specific ultrasound contrast agents and experienced personnel trained in the technique.
- Limited Availability: May not be available in all healthcare facilities compared to traditional HSG.
HSG Considerations:
- Radiation Exposure: Involves controlled X-ray exposure, which some women prefer to avoid.
- Contrast Reactions: Rare but possible allergic reactions to iodine-based contrast media.
- Facility Requirements: Requires access to specialised X-ray equipment and trained radiological staff.
- Static Images: Provides snapshot images rather than real-time dynamic assessment of contrast flow.
Procedure Experience and Comfort
Understanding what to expect during each procedure can help you prepare mentally and physically for the assessment:
HyCoSy Experience: The procedure takes place in a comfortable ultrasound room, similar to routine pregnancy scans. You’ll lie on an examination couch whilst a transvaginal ultrasound probe and small catheter are used to introduce contrast and monitor its flow. Most women describe the experience as similar to a smear test with mild cramping during contrast injection.
HSG Experience: The procedure occurs in an X-ray department, where you’ll lie on an examination table beneath X-ray equipment. A speculum is used to visualise the cervix, and contrast dye is introduced through a small catheter. The experience may involve slightly more intense cramping, particularly when the contrast fills the fallopian tubes.
Both procedures are typically performed without anaesthesia, though some clinics may offer pain relief options. Most women can return to normal activities immediately after either procedure, though mild cramping or light spotting may occur for 24-48 hours.
Accuracy and Clinical Outcomes
Research comparing HyCoSy and HSG demonstrates that both procedures offer comparable accuracy in detecting tubal abnormalities. Clinical studies indicate sensitivity rates of approximately 85-95% for both techniques in identifying blocked fallopian tubes, with specificity rates similarly high.
A systematic review published in fertility journals found no significant difference between HyCoSy and HSG in terms of diagnostic accuracy for tubal patency assessment. Both procedures effectively identify:
- Tubal Blockages: Complete or partial obstruction of one or both fallopian tubes.
- Uterine Abnormalities: Structural anomalies affecting the uterine cavity shape or size.
- Hydrosalpinx: Fluid accumulation within blocked fallopian tubes.
- Adhesions: Scar tissue affecting tubal function or mobility.
The choice between procedures often depends on individual circumstances, patient preferences, and clinical considerations rather than significant differences in diagnostic accuracy.
Timing and Preparation
Both HyCoSy and HSG require careful timing and preparation to ensure optimal results and patient safety:
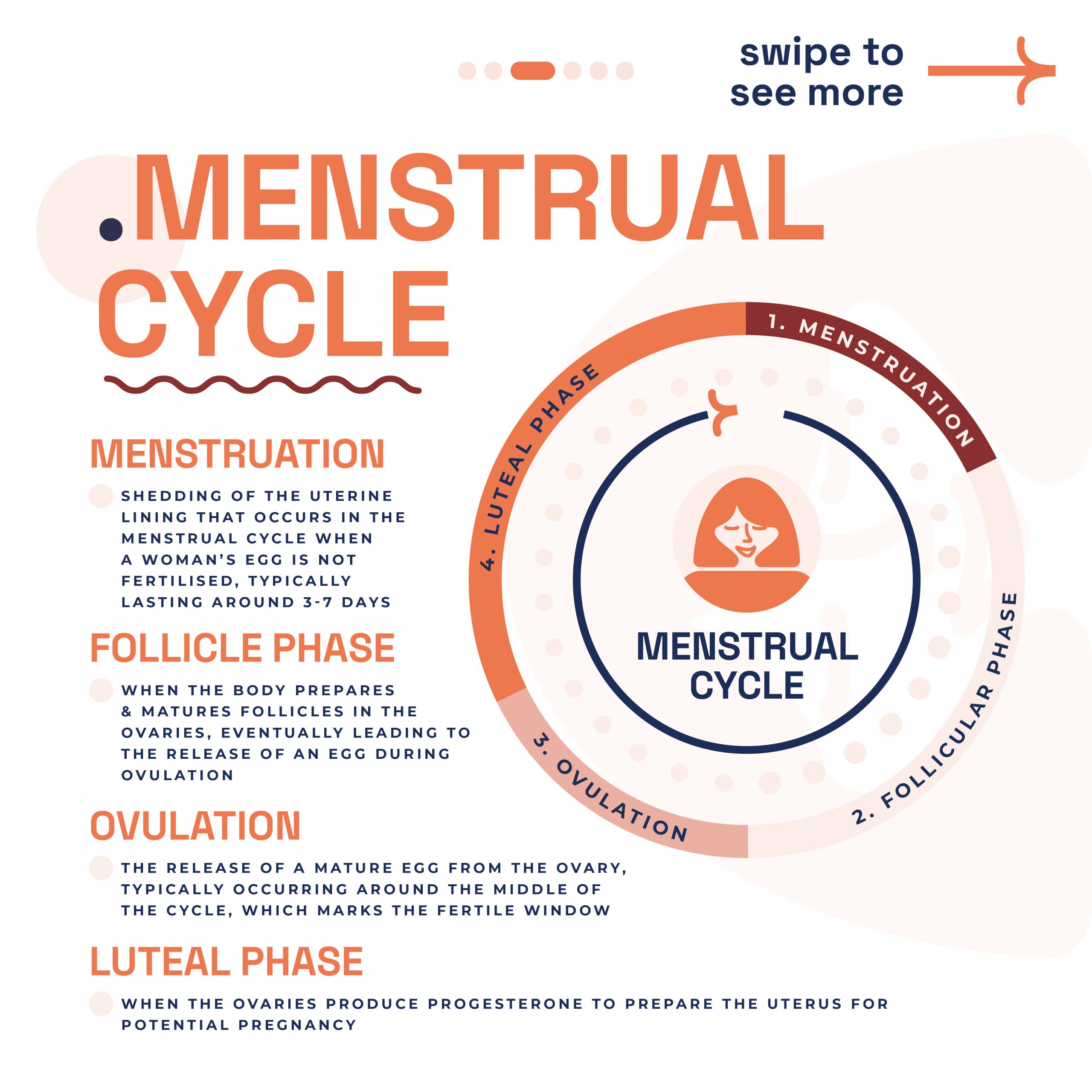
Optimal Timing: Both procedures should be performed in the first half of your menstrual cycle, typically between days 7-12, to avoid potential early pregnancy and ensure the endometrium is appropriately thin for clear visualisation.
Pre-procedure Preparation:
- Contraception: Reliable contraception should be used from the start of your cycle until the procedure to prevent pregnancy.
- Infection Screening: Some clinics may require screening for sexually transmitted infections before the procedure.
- Pain Management: Taking ibuprofen 1-2 hours before the procedure may help reduce discomfort.
- Medical History: Inform your clinician about any allergies, particularly to contrast media or medications.
Your healthcare provider will provide specific preparation instructions tailored to your individual circumstances and the chosen procedure.
Cost Considerations and NHS Availability
The availability and cost of HyCoSy versus HSG can vary significantly depending on whether you choose NHS or private healthcare pathways:
NHS Provision: Both procedures may be available through NHS fertility services, though availability varies by region and local commissioning decisions. HSG tends to be more widely available across NHS trusts, whilst HyCoSy availability may be limited to specialist centres.
Private Healthcare: Private fertility clinics typically offer both options, with costs varying depending on location and clinic facilities. HSG may be slightly less expensive in some settings due to established protocols and wider availability of equipment.
When considering costs, factor in potential follow-up appointments, additional imaging requirements, and the overall fertility assessment pathway rather than just the individual procedure cost.
Making Your Decision
Choosing between HyCoSy and HSG involves considering multiple factors specific to your individual circumstances:
- Radiation Sensitivity: If you have concerns about radiation exposure or require multiple assessments, HyCoSy may be preferable.
- Previous Procedures: Your experience with ultrasound scans versus X-ray procedures may influence your comfort level.
- Clinical Complexity: Your clinician may recommend one procedure over another based on your specific medical history.
- Availability and Timing: Local availability of equipment and expertise may influence your options.
- Personal Preferences: Your comfort with different types of medical procedures and imaging technologies.
Discussing these factors with your healthcare provider will help determine which procedure aligns best with your individual needs and circumstances. Both procedures provide valuable diagnostic information to guide your fertility treatment journey.
How the London Pregnancy Clinic Can Help
At the London Pregnancy Clinic, we offer comprehensive HyCoSy scanning services performed by experienced sonographers using state-of-the-art ultrasound equipment. Our team understands the emotional and physical aspects of fertility investigations and provides compassionate, professional care throughout your assessment.
Our HyCoSy procedures are conducted in comfortable, private facilities with immediate results discussion and detailed reporting for your healthcare providers. We work closely with fertility specialists and can provide comprehensive imaging assessments as part of your broader fertility investigation pathway.
For women requiring additional screening or genetic counselling as part of their fertility journey, we also offer carrier screening tests and genetic counselling services to provide comprehensive reproductive health assessments.
Final Thoughts
Both HyCoSy and HSG represent valuable diagnostic tools in fertility assessment, each offering distinct advantages depending on your individual circumstances. The choice between these procedures should be based on careful consideration of your medical history, personal preferences, and clinical recommendations from your healthcare team.
Remember that these investigations form just one component of comprehensive fertility assessment, and the results will help guide your treatment options and reproductive health decisions. Whether you choose HyCoSy or HSG, both procedures provide crucial information about fallopian tube function and uterine health.
If you’re considering fallopian tube assessment as part of your fertility journey, our experienced team at the London Pregnancy Clinic is here to provide expert care and support. Contact us today to discuss your options and book a consultation to determine the most appropriate diagnostic pathway for your individual needs.
Sources
-
- Hysterosalpingography (HSG) – Leeds Teaching Hospitals NHS Trust
- Hystero Contrast Sonography (HyCoSy) test – Buckinghamshire Healthcare NHS Trust
- Imaging department Booking your hysterosalpingogram (HSG)
- Tubal Patency Testing (HSG/HyCoSy) Eligibility (690) | Right Decisions
- Leeds Centre for Women’s Health Hysterosalpingography (HSG)
- Hysterosalpingo Contrast Sonography (HyCoSy) – Leeds Teaching Hospitals NHS Trust
- HSG (Hysterosalpingography) — Chelsea and Westminster Hospital NHS Foundation Trust