What Is an AFC Scan and What Does Your Antral Follicle Count Mean for Your Fertility?

What Is an AFC Scan and What Does Your Antral Follicle Count Mean for Your Fertility?
Published
Tags
Understanding your fertility potential is a crucial step in family planning, and one of the most valuable assessments available is the antral follicle count (AFC) scan. This specialised fertility screening provides essential insights into your ovarian reserve, helping to guide treatment decisions and predict how you might respond to fertility treatments. With approximately one in seven couples in the UK experiencing fertility difficulties, AFC scans have become an indispensable tool for fertility specialists and patients alike.
What Is an AFC Scan?
An antral follicle count (AFC) scan is a specialised transvaginal ultrasound examination that measures the number of antral follicles visible in both ovaries. Antral follicles are small, fluid-filled sacs measuring 2-9mm in diameter, each containing an immature egg. These follicles appear as dark, roughly circular areas on the ultrasound screen and represent your ovarian reserve – essentially, the number of eggs remaining in your ovaries.
The AFC scan is considered one of the gold standard methods for assessing ovarian reserve, alongside hormone blood tests such as anti-Müllerian hormone (AMH). Unlike blood tests that can fluctuate, the AFC provides a direct visual assessment of your ovaries’ current state. This transvaginal scan is typically performed during the early follicular phase of your menstrual cycle, usually between days 2-4, when hormone levels are at their baseline.
The procedure itself is straightforward and similar to other transvaginal ultrasounds. A small ultrasound probe is gently inserted into the vagina, providing clear, detailed images of the ovaries. The sonographer can then count the visible antral follicles in each ovary, providing an accurate assessment of your ovarian reserve.
Understanding Normal AFC Ranges
Antral follicle count results are typically categorised into different ranges that indicate varying levels of ovarian reserve. Understanding these ranges can help you interpret your results and discuss treatment options with your fertility specialist.
- Low AFC (3-6 total follicles): Indicates diminished ovarian reserve and may suggest a reduced response to fertility treatments.
- Normal AFC (7-15 total follicles): Represents a healthy ovarian reserve with good potential for natural conception and fertility treatment success.
- High AFC (16-24 total follicles): Suggests excellent ovarian reserve but may increase the risk of ovarian hyperstimulation syndrome during fertility treatments.
- Very high AFC (25+ total follicles): May indicate polycystic ovary syndrome (PCOS) and requires careful management during fertility treatments.
It’s important to note that these ranges can vary slightly between different clinics and medical guidelines. The RCOG recognises that individual circumstances vary, and your fertility specialist will interpret your results in the context of your age, medical history, and other fertility factors. A pelvic scan may also be recommended to assess the overall structure and health of your reproductive organs.
Why AFC Matters for Your Fertility
Your antral follicle count provides crucial information about several aspects of your fertility potential. Understanding these implications can help you make informed decisions about family planning and treatment options.
Firstly, AFC serves as a predictor of ovarian response to fertility medications. Women with higher AFCs typically produce more eggs during ovarian stimulation, whilst those with lower counts may require adjusted medication protocols or different treatment approaches. This information is invaluable for fertility specialists planning IVF cycles or other assisted reproductive treatments.
The AFC also helps predict the likelihood of pregnancy success with various fertility treatments. Research indicates that women with very low AFCs may have reduced live birth rates, whilst those with normal to high counts generally have better prognosis. Additionally, AFC can help identify women at risk of ovarian hyperstimulation syndrome (OHSS), allowing specialists to adjust treatment protocols accordingly.
For women considering egg freezing, AFC provides essential information about the optimal timing and expected outcomes. A higher AFC suggests that more eggs can potentially be retrieved and frozen, improving future fertility options. This assessment is particularly valuable for women who wish to preserve their fertility for personal or medical reasons.
When Should You Have an AFC Scan?
Several circumstances may warrant an AFC scan as part of your fertility assessment. Understanding when this test is recommended can help you seek appropriate care at the right time.
Women experiencing difficulty conceiving after six months of trying (if over 35) or twelve months (if under 35) should consider comprehensive fertility testing, including an AFC scan. This assessment provides valuable baseline information that can guide further investigations and treatment decisions.
AFC scans are also recommended before starting any fertility treatments, including IVF, intrauterine insemination (IUI), or ovarian stimulation. The results help fertility specialists tailor medication doses and treatment protocols to your individual needs, optimising both safety and success rates.
Women with irregular menstrual cycles, suspected PCOS, or family history of early menopause may benefit from AFC assessment. Additionally, if you’re considering egg freezing or have concerns about your fertility potential, an AFC scan can provide valuable insights to inform your decisions. The scan works well alongside follicle tracking scans during treatment cycles.
The AFC Scan Procedure: What to Expect
Understanding what happens during an AFC scan can help alleviate any anxiety and ensure you’re properly prepared for the appointment. The procedure is straightforward, typically taking 15-20 minutes to complete.
You’ll be asked to undress from the waist down and lie on an examination couch with your knees bent and feet in stirrups, similar to a cervical screening position. The sonographer will insert a thin ultrasound probe, covered with a protective sheath and gel, gently into your vagina. This provides clear, detailed images of your ovaries on the ultrasound screen.
The sonographer will systematically examine both ovaries, counting the visible antral follicles and measuring your ovaries’ size and structure. You may feel slight pressure during the examination, but the procedure shouldn’t be painful. Many women find it helpful to empty their bladder before the scan for comfort.
Results are typically available immediately after the scan, and the sonographer or specialist can discuss the findings with you straight away. You’ll receive a detailed report that can be shared with your GP or fertility specialist for further treatment planning. This comprehensive assessment complements other fertility investigations you may have undergone.
Factors That Can Affect Your AFC
Several factors can influence your antral follicle count, some of which are modifiable whilst others are not. Understanding these factors can help you interpret your results and potentially improve your fertility outcomes.
Age is the most significant factor affecting AFC, with counts naturally declining as women get older. This decline accelerates after age 35, with more rapid decreases typically occurring in the early forties. However, there’s considerable individual variation, and some women maintain good AFCs longer than others.
Hormonal contraceptives, particularly the combined oral contraceptive pill, can temporarily suppress AFC measurements. If you’re taking hormonal contraception, your specialist may recommend stopping it for 1-3 months before the AFC scan for more accurate results. Other factors including smoking, certain medications, previous ovarian surgery, and medical conditions like endometriosis can also impact your AFC.
Lifestyle factors such as stress, poor nutrition, excessive exercise, and environmental toxins may negatively affect ovarian reserve. Whilst you cannot change your age or genetic factors, addressing modifiable risk factors may help optimise your fertility potential and overall reproductive health.
AFC Results and Treatment Planning
Your AFC results play a crucial role in determining the most appropriate fertility treatment approach for your individual circumstances. Fertility specialists use this information alongside other factors to develop personalised treatment plans.
For women with low AFCs, treatment protocols typically involve higher doses of fertility medications or alternative approaches such as natural cycle IVF or donor egg treatment in some cases. The focus shifts to maximising the quality of available eggs rather than quantity, and specialists may recommend proceeding with treatment sooner rather than later.
Normal AFC results generally indicate good treatment prospects, with standard stimulation protocols likely to be effective. Women in this category often have multiple treatment options available and may choose to delay treatment if desired, though age-related factors should still be considered.
High AFCs require careful management to prevent ovarian hyperstimulation syndrome. Treatment protocols typically use lower medication doses, close monitoring throughout the cycle, and sometimes alternative trigger medications. Women with very high AFCs and suspected PCOS may need additional assessments and specialised treatment approaches. Follicle tracking scans become particularly important during treatment cycles.
AFC and Age: Understanding the Connection
The relationship between age and antral follicle count is one of the most important aspects to understand when interpreting your results. This connection has significant implications for fertility potential and treatment planning.
Women are born with all the eggs they’ll ever have, approximately 1-2 million at birth. This number continuously declines throughout life, falling to around 400,000 at puberty and continuing to decrease at an accelerating rate. By age 37, most women have only about 25,000 eggs remaining, with this number dropping to approximately 1,000 by age 51.
AFC generally correlates with this natural decline, but there’s considerable individual variation. Some women in their late thirties may have AFCs similar to women in their twenties, whilst others may show earlier declines. This variability makes individual assessment crucial rather than relying solely on age-based predictions.
Understanding your personal AFC in relation to your age helps set realistic expectations for treatment outcomes. A 35-year-old with a high AFC may have better treatment prospects than a 30-year-old with a low AFC, highlighting the importance of individualised assessment and counselling throughout the fertility journey.
Limitations and Considerations of AFC Testing
Whilst AFC scans provide valuable fertility information, it’s important to understand their limitations and what they cannot tell you about your reproductive potential.
AFC primarily indicates quantity rather than quality of eggs. A high antral follicle count doesn’t guarantee that the eggs are chromosomally normal or capable of developing into healthy embryos. Egg quality is more closely related to age, and even women with low AFCs can achieve pregnancy with good-quality eggs.
The scan also cannot predict natural conception rates with certainty. Some women with low AFCs conceive naturally, whilst others with normal counts may experience fertility difficulties due to other factors such as tubal blockages, male factor infertility, or unexplained infertility.
AFC measurements can vary between different operators and ultrasound machines, and results may fluctuate slightly between cycles. It’s important to have scans performed by experienced sonographers using high-quality equipment. Additionally, certain conditions like ovarian cysts or recent ovulation can affect follicle visibility and counting accuracy. Your specialist will consider these factors when interpreting your results alongside other fertility assessments and your medical history.
Improving Your Fertility Outcomes
Regardless of your AFC results, there are several steps you can take to optimise your fertility potential and improve treatment outcomes. These recommendations apply to all women trying to conceive, whether naturally or through assisted reproduction.
Maintaining a healthy lifestyle forms the foundation of fertility optimisation. This includes following a balanced diet rich in folate, vitamin D, and antioxidants, achieving and maintaining a healthy weight, engaging in regular moderate exercise, and avoiding smoking and excessive alcohol consumption. These factors can positively impact both egg quality and overall reproductive health.
Managing stress through relaxation techniques, counselling, or support groups can also be beneficial. Chronic stress may negatively affect hormone levels and ovulation, potentially impacting fertility outcomes. Ensuring adequate sleep and managing underlying health conditions such as diabetes or thyroid disorders are equally important.
Timing is crucial in fertility treatment, particularly for women with low AFCs. Don’t delay seeking specialist advice if you have concerns about your fertility. Early assessment and intervention can maximise your chances of success and provide more treatment options. Remember that fertility is a complex interplay of many factors, and AFC is just one piece of the puzzle.
How the London Pregnancy Clinic Can Help
At the London Pregnancy Clinic, we understand that fertility concerns can be both emotionally and physically challenging. Our experienced team of specialist sonographers and fetal medicine consultants provide comprehensive AFC scanning services using state-of-the-art ultrasound equipment to ensure accurate, reliable results.
Our fertility screening services include detailed AFC assessments performed by specialists who understand the nuances of ovarian reserve testing. We take time to explain your results thoroughly, discussing what they mean for your individual circumstances and potential treatment options. Our compassionate approach ensures you feel supported throughout your fertility journey.
We offer flexible appointment times to accommodate your menstrual cycle timing, ensuring optimal accuracy of your AFC scan. Our detailed reports can be easily shared with your fertility specialist or GP to facilitate seamless care coordination. Additionally, we provide access to genetic counselling services if your results indicate the need for further genetic assessment or family planning guidance.
Whether you’re just beginning to explore your fertility potential or seeking a second opinion on previous results, our clinic provides a comfortable, professional environment where you can receive expert care. We’re committed to delivering accurate, timely results that help inform your reproductive health decisions with confidence and clarity.
Final Thoughts
An AFC scan represents a valuable tool in modern fertility assessment, providing crucial insights into your ovarian reserve and helping guide treatment decisions. Whilst the results can feel overwhelming, remember that AFC is just one factor in your fertility journey, and many women with varying AFCs go on to achieve successful pregnancies.
Understanding your antral follicle count empowers you to make informed decisions about your reproductive health and family planning timeline. Whether your results indicate low, normal, or high ovarian reserve, working with experienced specialists ensures you receive personalised care tailored to your unique circumstances.
If you’re considering fertility assessment or have concerns about your reproductive health, don’t hesitate to seek professional guidance. Early evaluation can provide peace of mind and ensure you have all the information needed to make the best decisions for your future. Contact the London Pregnancy Clinic today to discuss your fertility screening options and take the first step towards understanding your reproductive potential.
Sources
- Antral follice counts (AFC) predict ovarian response and pregnancy outcomes in oocyte donation cycles – PMC
- Ovarian Reserve Testing: Range, Purpose & Results
- AFC (Antral Follicle Count) Ultrasound | Spital Clinic London
- AFC scan | TFP Fertility UK
- Antral follicle count: What is it? | Access Fertility
- What exactly is antral follicle count (AFC)?
- Antral follicle count | Radiology Reference Article | Radiopaedia.org
- What is Antral Follicle Count (& Why it Matters for Egg Freezing)
- Antral Follicle Count Testing Explained: How Clinics Measure AFC | Seen Fertility
- Fertility Testing 101: What Is An Antral Follicle Count (AFC) And Should You Get One?
- Antral Follicle Count (AFC): Normal Count & How To Increase
- Antral Follicle Count – Somerset Early Scans
Latest Stories
London Pregnancy Clinic West

Your Trusted Experts in West London
London Pregnancy Clinic Expands to Chelsea
-
Published
-
Last Modified
Tags
London Pregnancy Clinic is thrilled to announce the opening of its second location in Chelsea, West London, hosted within the prestigious Westminster Women’s Clinic. This expansion brings trusted services, including early pregnancy scans, viability scans, and advanced NIPT options such as PrenatalSafe and SMART Test, closer to West London families. Supported by a highly skilled team and advanced technology, the clinic offers personalised care in a serene environment. Book your appointment today for world-class pregnancy support.
We are delighted to announce the opening of London Pregnancy Clinic’s second location in Chelsea, West London. This expansion reflects our mission to make expert prenatal care and early pregnancy diagnostics accessible to even more expectant mothers across London.
A Partnership with Westminster Women’s Clinic
This exciting new chapter for London Pregnancy Clinic is hosted within the renowned Westminster Women’s Clinic (WWC) in Chelsea. Known for its outstanding reputation in women’s healthcare, WWC provides a state-of-the-art environment that aligns perfectly with our commitment to delivering excellence in care.
Miss Jess McMicking, founder of WWC, shared her enthusiasm about this collaboration, saying, “Very much looking forward to having London Pregnancy Clinic and their exceptional team in our surrounds, and most importantly, their expertise for our patients and the wider West London community.”
This partnership allows London Pregnancy Clinic to offer its trusted services in a setting renowned for prioritising women’s health, ensuring every patient feels supported and cared for during their journey.
Comprehensive Services Tailored to Your Pregnancy
At the Chelsea clinic, you will find the same exceptional care that has earned London Pregnancy Clinic a trusted name in pregnancy health. Early pregnancy scans are available to provide reassurance during the critical first trimester, while viability and dating scans help confirm pregnancy progression and determine your baby’s due date. Advanced Non-Invasive Prenatal Testing (NIPT), including the PrenatalSafe NIPT and SMART Test, ensures accurate screening for chromosomal conditions like Down syndrome.
With over 30 years of expertise in Obstetrics and Gynaecology, our team ensures every service is delivered using cutting-edge ultrasound technology, providing accurate results in a calm and supportive environment.
Why Choose London Pregnancy Clinic in Chelsea?
The new clinic in Chelsea makes expert prenatal care accessible to mothers in West London, including Chelsea, Fulham, Kensington, Knightsbridge, and nearby areas. Situated within Westminster Women’s Clinic, the location combines the welcoming atmosphere and advanced diagnostic tools that are central to the London Pregnancy Clinic experience. From the moment you arrive, you will feel supported in a serene environment where your well-being is the priority.
Meet New Our Expert Team
We are proud to introduce new members of the London Pregnancy Clinic team who will be based at both the City and Chelsea locations. Saskia Hicks, a knowledgeable midwife, brings a compassionate approach to guiding expectant mothers. Eden Ovadia, our dedicated medical assistant, ensures patients feel comfortable and well-cared-for during every visit. Victoria Bennet, an experienced sonographer, offers advanced fetal imaging expertise, while Lih-Wen Wang, a skilled medical assistant and phlebotomist, brings professionalism and care to every interaction.
Looking Ahead: Expanding Services in Chelsea
While our Chelsea location already offers exceptional prenatal care, including early pregnancy scans, viability scans, and advanced NIPT options such as PrenatalSafe and SMART Test, we are committed to bringing even more comprehensive services to West London in the near future.
Plans are underway to introduce midwifery services, allowing us to provide expectant mothers with continuous, personalised support throughout their pregnancy journey. From antenatal appointments to postpartum care, our future midwifery services aim to offer holistic care for mothers and babies alike.
We are also looking to expand our offerings to include fertility screenings and consultations, ensuring that women seeking support with conception have access to expert guidance and diagnostics close to home. Whether it’s follicle tracking scans or pre-conception assessments, these services will help us provide well-rounded care to individuals and families at every stage of their reproductive journey.
Our goal is to ensure that our Chelsea clinic becomes a one-stop destination for women’s health in West London, with an emphasis on expert care, state-of-the-art facilities, and a compassionate approach. As we continue to grow, we remain dedicated to listening to our patients and evolving to meet their needs.

Final Thoughts
Whether you’re seeking early pregnancy scans, prenatal testing, or reassurance during your pregnancy journey, our Chelsea clinic is here to provide expert, compassionate care. Book your appointment today to receive world-class care tailored to your needs. Visit our booking system to learn more and schedule your visit.
Latest Stories
PCOS Awareness Month

PCOS Awareness Month 2024
Polycystic Ovary Syndrome (PCOS): Understanding, Symptoms, and Care
-
Published
-
Last Modified
Tags
Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder affecting 1 in 10 women in the UK, often leading to fertility challenges and other health risks such as diabetes and cardiovascular disease. This blog explores PCOS symptoms, including irregular periods, weight gain, and excess hair growth, and outlines management options like lifestyle changes, medication, and fertility treatments.
Polycystic Ovary Syndrome (PCOS) is a common hormonal disorder that can have a significant impact on women of reproductive age. Affecting around 1 in 10 women in the UK, PCOS is characterised by a range of symptoms and can lead to complications, including difficulties with fertility. At London Pregnancy Clinic, we are committed to raising awareness about PCOS, its implications, and the support available for managing this condition.
What is Polycystic Ovary Syndrome?
PCOS is a condition that affects the normal functioning of the ovaries due to hormonal imbalances. Typically, it results in irregular or absent periods, and in some cases, multiple small cysts form on the ovaries. The condition often begins during adolescence but can develop at any stage of a woman’s reproductive life. It is important to note that not all women with PCOS will have cysts, despite the name.
It occurs when a woman produces higher-than-normal levels of androgens, or “male hormones,” which disrupt ovulation and other hormonal processes. This imbalance can lead to a variety of symptoms and health challenges, making early detection and management essential.
Polycystic Ovary Syndrome Statistics
PCOS is one of the most common causes of infertility in women, but it often goes undiagnosed. According to the NHS, more than half of women with PCOS do not have any noticeable symptoms, which can delay diagnosis and treatment. In the UK alone, PCOS affects about 10% of women, with its prevalence varying worldwide. The condition not only affects fertility but can also lead to other health issues such as type 2 diabetes, cardiovascular diseases, and mental health problems if left untreated.
Polycystic Ovary Syndrome Symptoms
The symptoms can vary in severity and may develop gradually over time. The most common symptoms include:
- Irregular or absent periods: Due to disrupted ovulation, women with PCOS may experience infrequent or prolonged menstrual cycles.
- Excess hair growth (hirsutism): Elevated levels of androgen hormones can lead to excessive facial and body hair growth.
- Weight gain: Unexplained weight gain or difficulty losing weight is a common symptom, and excess weight can exacerbate the condition.
- Acne and oily skin: The hormonal imbalance often leads to acne, particularly on the face, chest, and back.
- Thinning hair or male-pattern baldness: Hair loss can occur on the scalp due to high androgen levels.
- Ovarian cysts: Although not always present, some women may develop multiple cysts on their ovaries, which can be detected via an ultrasound.
- Difficulty conceiving: As PCOS interferes with ovulation, it is one of the leading causes of infertility in women.
PCOS and Fertility
One of the primary concerns for women with PCOS is infertility. The hormonal imbalance associated with the condition can prevent ovulation, making it difficult for women to conceive. In fact, it is one of the most common causes of infertility worldwide. However, with appropriate medical treatment, many women with PCOS can conceive and have healthy pregnancies.
At London Pregnancy Clinic, we offer a range of fertility treatments, including ovulation induction, hormonal therapy, and assisted reproductive technologies like IVF, to help women with PCOS conceive. Early diagnosis and intervention are key to improving fertility outcomes.
Long-term Health Risks
In addition to reproductive health concerns, PCOS can lead to several long-term health issues. These include:
- Type 2 diabetes: Women are at a higher risk of developing insulin resistance, which can lead to type 2 diabetes.
- Cardiovascular disease: PCOS is associated with an increased risk of high blood pressure, high cholesterol, and heart disease.
- Endometrial cancer: Women may have an increased risk of developing endometrial cancer due to irregular periods and prolonged exposure to oestrogen.
- Mental health issues: Depression, anxiety, and poor body image are common, particularly those struggling with symptoms like infertility and unwanted hair growth.
Managing Polycystic Ovary Syndrome
Although there is no cure for PCOS, the symptoms can be managed effectively through lifestyle changes and medical treatments. At London Pregnancy Clinic, we provide comprehensive care for women with PCOS, focusing on both short-term symptom relief and long-term health management.
- Lifestyle changes: Maintaining a healthy weight through diet and regular exercise can significantly reduce PCOS symptoms. Even a small amount of weight loss can help regulate menstrual cycles and improve insulin sensitivity.
- Medication: Hormonal contraceptives are often prescribed to regulate periods and reduce androgen levels. For women trying to conceive, medications such as Clomiphene can help induce ovulation. Metformin, a medication typically used for type 2 diabetes, can also improve insulin resistance and lower androgen levels.
- Fertility treatments: For women with PCOS struggling to conceive, fertility treatments like IVF may be recommended. Our specialists work closely with patients to develop tailored treatment plans that maximise the chances of a successful pregnancy.
- Cosmetic treatments: Treatments such as laser hair removal or prescription acne medications can help manage the physical symptoms of PCOS, such as excess hair growth and acne.
Raising Awareness About PCOS
The emotional toll of PCOS should not be underestimated. Many women with PCOS struggle with self-esteem, body image issues, and mental health challenges due to symptoms like infertility, weight gain, and hirsutism. At LPC, we offer support for the psychological aspects of PCOS, ensuring women have access to both physical and emotional care.
We are dedicated to raising awareness about PCOS and the importance of early diagnosis and management. PCOS is often underdiagnosed, but with the right care, women can lead healthy lives and achieve their fertility goals. We encourage women who suspect they may have PCOS to seek medical advice and take proactive steps towards managing the condition.
Diagnosing PCOS involves a combination of clinical assessments, blood tests, and imaging studies. During your consultation at London Pregnancy Clinic, your female GP doctor will assess your medical history, perform a physical examination, and conduct blood tests to measure hormone levels. An ultrasound may also be recommended to examine your ovaries for cysts and assess ovulation.
Final Thoughts
Ectopic pregnancy is a serious condition that requires prompt medical attention. Recognising the symptoms early and seeking immediate care can prevent life-threatening complications and preserve future fertility. London Pregnancy Clinic offers advanced early ultrasound services and expert care to detect and manage ectopic pregnancies effectively. If you have concerns about your pregnancy or are experiencing any symptoms of an ectopic pregnancy, contact LPC right away to schedule an early ultrasound and ensure your pregnancy is developing safely.
If you’re concerned about your pregnancy or have experienced any symptoms of an ectopic pregnancy, don’t hesitate to reach out to London Pregnancy Clinic. Early detection is key to managing extrauterine pregnancy effectively. Visit London Pregnancy Clinic for expert advice and care tailored to your needs.
Latest Stories
Ectopic Pregnancy

What is an Ectopic Pregnancy?
Understanding Ectopic Pregnancy: Causes, Symptoms, and Treatment
-
Published
-
Last Modified
Tags
Ectopic pregnancy is a serious and life-threatening condition where a fertilised egg implants outside the uterus. Unlike normal pregnancies, where the embryo develops within the uterine lining, ectopic pregnancies often occur in the fallopian tubes, leading to potentially severe complications. Understanding the signs, causes, and treatment options for extrauterine pregnancy is crucial for early detection and management, which can significantly improve outcomes for women.
In a typical pregnancy, the fertilised egg travels down the fallopian tube and implants itself in the uterus. However, in an ectopic pregnancy, the egg implants outside the uterus, most commonly in the fallopian tube, leading to what is often referred to as a “tubal pregnancy.” Although less common, ectopic pregnancies can also occur in the ovary, abdomen, or cervix. These locations are not equipped to support a growing pregnancy, and as the embryo develops, it can cause severe damage to the surrounding tissues, potentially leading to life-threatening bleeding.
Causes of Ectopic Pregnancy
Several factors can contribute to the likelihood of such a pregnancy. The primary cause is usually damage to the fallopian tubes, which may prevent the fertilised egg from reaching the uterus. Conditions such as pelvic inflammatory disease (PID), often caused by sexually transmitted infections, can inflame and scar the fallopian tubes. Other causes include endometriosis, which leads to abnormal tissue growth outside the uterus, and prior surgeries on the fallopian tubes, which can leave scar tissue that obstructs the egg’s journey. Additionally, hormonal imbalances and certain congenital abnormalities in the fallopian tubes can also increase the risk.
Symptoms of Ectopic Pregnancy
Recognising the symptoms of an ectopic pregnancy is vital for timely intervention. Early symptoms often mimic those of a normal pregnancy, including missed periods, breast tenderness, and nausea. However, the first warning signs of an extrauterine pregnancy are usually pain and vaginal bleeding. Pain can be felt in the pelvis, abdomen, or even the shoulder and neck if the bleeding irritates the diaphragm. This pain can vary from mild and dull to severe and sharp. Other symptoms might include dizziness, fainting, low blood pressure due to blood loss, and lower back pain. If an ectopic pregnancy is not detected early, it can lead to the rupture of the fallopian tube, which is a medical emergency.
Diagnosis of Ectopic Pregnancy
Diagnosing an ectopic pregnancy can be challenging, especially in the early stages when symptoms are similar to a normal pregnancy. If a woman presents with symptoms indicative of an ectopic pregnancy, doctors will typically conduct an ultrasound to determine the location of the pregnancy. However, an ultrasound may not always be able to detect an ectopic pregnancy early on, particularly if it is too small to be seen. In such cases, repeated testing may be necessary. Blood tests for pregnancy that measure human chorionic gonadotropin (hCG) levels are also used, as abnormal levels can indicate a non-intrauterine pregnancy.
Women’s Health Services Beyond Ultrasounds
The treatment for an ectopic pregnancy depends on its size and location, as well as the patient’s overall health. In some cases, if the extrauterine pregnancy is detected early and is small, doctors may use medication such as methotrexate to stop the growth of the embryo. The body then absorbs the tissue naturally. This non-surgical approach is less invasive but requires close monitoring of hCG levels until they return to zero. This can be done with a blood test which London Pregnancy Clinic offers.
For more advanced ectopic pregnancies, surgery is often required. Laparoscopic surgery is the most common method, where the surgeon removes the ectopic pregnancy and repairs any damage to the fallopian tube. In severe cases, where the fallopian tube has ruptured, emergency surgery may be necessary, and the affected fallopian tube might need to be removed. Following treatment, regular follow-up with healthcare providers is essential to ensure complete recovery and monitor future fertility.
Impact on Future Pregnancies
Having an ectopic pregnancy can affect future pregnancies, although many women go on to have normal pregnancies afterward. The risk of a subsequent non-intrauterine pregnancy is higher, especially if the woman has a history of conditions like PID or previous tubal surgeries. However, with proper medical care and monitoring, many women can conceive successfully. It’s important for women who have had an ectopic pregnancy to consult with their doctor before trying to conceive again to discuss the best timing and necessary precautions.
Preventing Ectopic Pregnancy
While it is not always possible to prevent an ectopic pregnancy, certain lifestyle choices can reduce the risk. Quitting smoking is one of the most effective preventive measures, as smoking is linked to damage in the fallopian tubes. Practicing safe sex by using condoms can help prevent sexually transmitted infections, which are a leading cause of PID and, subsequently, ectopic pregnancies. Regular gynecological exams and prompt treatment of infections can also lower the risk.
Emotional Support and Recovery
Experiencing an ectopic pregnancy can be emotionally challenging. It is not uncommon for women to feel a profound sense of loss, similar to that experienced after a miscarriage. Emotional recovery can take time, and many women find it helpful to seek support from counseling services or support groups. It’s important to acknowledge the grief and allow time for healing. Partners and families should also be supportive, understanding that the emotional impact can be significant.
The Importance of Early Ultrasound
Early detection is crucial when it comes to managing ectopic pregnancy effectively. At London Pregnancy Clinic (LPC), we understand the importance of early and accurate diagnosis. Our clinic offers advanced early pregnancy scans that can detect ectopic pregnancies as soon as they develop, often before symptoms become severe. These ultrasounds are essential in confirming the location of the pregnancy, whether it is intrauterine or ectopic. You can read on what to expect at an ultrasound scan on our blog, or watch our youtube video on this.
Ultrasound scans are a crucial part of early pregnancy care and can help ensure that your pregnancy is progressing normally. Here are the key points about when you should consider doing an ultrasound scan, especially in the context of monitoring for ectopic pregnancies:
When to Do an Ultrasound Scan
-
Confirmation of Pregnancy (6-8 Weeks): The first ultrasound is typically done around 6 to 8 weeks of pregnancy. This early scan confirms the pregnancy and helps determine whether the embryo has implanted in the uterus or if there’s a risk of ectopic pregnancy. It also provides information about the viability of the pregnancy, the gestational age, and the number of embryos (in the case of multiple pregnancies).
-
Early Signs of Ectopic Pregnancy: If you experience symptoms that may suggest an ectopic pregnancy, such as pelvic pain, abnormal vaginal bleeding, or shoulder pain, you should have an ultrasound as soon as possible. These symptoms can appear between 4 and 12 weeks of pregnancy. Early detection through ultrasound is crucial in managing ectopic pregnancy before it leads to more serious complications, such as the rupture of the fallopian tube.
-
Uncertain Pregnancy Dates: If your menstrual cycle is irregular or you’re unsure about the date of your last period, an ultrasound scan can help establish the gestational age of the pregnancy. This is important for ensuring that the pregnancy is developing as expected and for scheduling further scans and tests.
-
High-Risk Pregnancies: Women who have a history of ectopic pregnancies, pelvic inflammatory disease (PID), previous tubal surgery, or other risk factors should consider an early ultrasound. This is particularly important if there are any concerning symptoms or if the pregnancy is achieved through fertility treatments, which can increase the risk of ectopic pregnancy.
How LPC Can Help
By scheduling an early ultrasound at LPC, you can ensure that your pregnancy is progressing normally and reduce the risk of complications associated with ectopic pregnancies. Our team of experienced specialists uses the latest ultrasound technology to provide precise and reliable results, giving you peace of mind and the information you need to make informed decisions about your care.
If an ectopic pregnancy is detected, our clinic offers comprehensive support and care, including personalised treatment plans and close monitoring to ensure your safety and well-being. We are committed to providing compassionate care and expert guidance throughout your pregnancy journey.
Final Thoughts
Ectopic pregnancy is a serious condition that requires prompt medical attention. Recognising the symptoms early and seeking immediate care can prevent life-threatening complications and preserve future fertility. London Pregnancy Clinic offers advanced early ultrasound services and expert care to detect and manage ectopic pregnancies effectively. If you have concerns about your pregnancy or are experiencing any symptoms of an ectopic pregnancy, contact LPC right away to schedule an early ultrasound and ensure your pregnancy is developing safely.
If you’re concerned about your pregnancy or have experienced any symptoms of an ectopic pregnancy, don’t hesitate to reach out to London Pregnancy Clinic. Early detection is key to managing extrauterine pregnancy effectively. Visit London Pregnancy Clinic for expert advice and care tailored to your needs.
Latest Stories
The Fertility Show London

LPC at Fertility Show 2024
-
Published
-
Last Modified
Tags
London Pregnancy Clinic (LPC) is excited to share our experience exhibiting at the Fertility Show 2024 in Olympia, held on 18-19 May. This prestigious event brought together top fertility experts, clinics, and support groups, offering invaluable insights and support to those on the path to parenthood. LPC was thrilled to be part of this inspiring event, connecting with attendees and sharing our expertise in prenatal care.
Fertility Show 2024 at Olympia was a remarkable event that provided a comprehensive platform for individuals and couples looking to start or grow their families. As first-time exhibitors, LPC was honoured to participate in this two-day event, which featured over 70 exhibitors, including leading fertility specialists, clinics, and support groups.
Connecting with Attendees
At the Fertility Show, we had an amazing time, meeting and connecting with so many incredible professionals in the field. Our stand was buzzing with activity as we shared insights about our comprehensive prenatal services and discussed the latest advancements in fertility care. The event was an incredible opportunity for LPC to engage directly with prospective parents. Our team was on hand to answer questions, provide guidance, and offer reassurance to those embarking on their fertility journey. We were thrilled to meet so many individuals and couples seeking to expand their families.
Expert Insights and Panels
It featured a series of expert panels and seminars covering a wide range of topics, from the latest advancements in IVF to holistic approaches to fertility. LPC’s representatives attended sessions led by renowned fertility specialists and participated in discussions about the latest trends and techniques in reproductive medicine.
One of the standout features of the show was the Fertility Support Hub. This dedicated space offered attendees the chance to meet with nurses, counsellors, and workplace support teams. LPC’s own team of specialists provided one-on-one consultations, helping attendees navigate their options and make informed decisions about their fertility treatment.
Special Acknowledgments
A special shout out to our dedicated obstetrics and gynaecological team Shaz Khojasteh, Diane Nzelu, Prashant Purohit, and Molly Payne. Their expertise and passion were truly inspiring to all who visited our stand. Your commitment to advancing fertility and prenatal health is what makes us stand out.
Our team worked hard to set up and design the space to be welcoming and homey, and a lot of you loved it! Our totes were a big success and were taken very fast too.
Our Services
Here at LPC we offer comprehensive services designed to support you throughout your fertility and pregnancy journey. Our mission is to provide a reassuring experience through our extensive expertise and ultrasound technology.
Preconception
Fertility Scans: We specialise in fertility scans, including follicle tracking and endometrial lining scans. These scans monitor the growth and development of follicles, pinpoint ovulation, and enhance fertility treatment outcomes. Our endometrial lining scan evaluates the thickness and health of the endometrium, determining the best period for embryo implantation. These scans are crucial in both natural and assisted reproductive journeys.
HyCoSy and 3D SIS Scans: We offer Hysterosalpingo Contrast Sonography HyCoSy and 3D SIS scans to examine the uterus and fallopian tubes. These non-invasive procedures provide detailed images to detect blockages or abnormalities, ensuring a thorough evaluation of your reproductive health.
Pregnancy
Pregnancy Ultrasound Scans: Our clinic provides a range of prenatal scans to monitor your baby’s health at every stage of pregnancy. We use the latest 2D, 3D, and 4D ultrasound imaging technology to offer clear and detailed insights. From viability scans at 6-9 weeks to anomaly scans in the third trimester, our comprehensive approach ensures you receive the best care.
Non-Invasive Prenatal Testing (NIPT): LPC is a leading provider of NIPT in London. This advanced screening option detects Down’s syndrome and other chromosomal conditions. NIPT can be performed from 10 weeks of pregnancy and is the most accurate, safest screening test available. Our SMART Test combines NIPT with ultrasound, providing a comprehensive screening for a range of rare diseases and anomalies.
Holistic Care: Our holistic approach includes support from conception to birth. We offer a welcoming and homey environment, ensuring you feel comfortable throughout your journey. Our team worked hard to design a space that was both inviting and informative. Attendees appreciated the effort, and our totes, filled with useful information, were a big success.
Thank You
Thank you to everyone who stopped by to chat with us. Your enthusiasm and dedication to advancing fertility and prenatal health are truly inspiring. We’re excited to keep these conversations going and continue supporting you on your journey to parenthood.
Final Thoughts
Participating in the Fertility Show 2024 was a significant milestone for LPC. We are dedicated to supporting individuals and couples on their fertility journey, providing expert care and guidance every step of the way. Stay tuned for more updates and connect with us for the latest in prenatal care and fertility support. If you missed us at the show or would like to learn more about our services, please contact us directly to schedule a consultation. Together, we can make your dream of parenthood a reality.
Latest Stories
What is a Fallopian Tube?
Fallopian Tubes: all you need to know
Discovering the importance of fallopian tubes for fertility.
-
Published
-
Last Modified
Tags
Explore the critical role of fallopian tubes, or uterine tubes, in pregnancy and fertility. This post delves into their anatomy, function, and common issues affecting fertility, providing essential insights for expectant mothers and those planning pregnancy.
Welcome to our comprehensive guide on the fallopian tubes, an essential component of the female reproductive system. We also explore common pathologies that affect these tubes, leading to infertility issues and complications like ectopic pregnancies. Our esteemed in-house gynae team, brings their extensive knowledge and expertise to this discussion, providing invaluable insights into the significance of maintaining fallopian tube health. Join us as we unfold the mysteries of the fallopian tubes and their vital function in the miracle of life.
What are Fallopian Tubes
In the female body, the pelvis houses two vital structures known as fallopian tubes. One on either side of the uterus. These tubes act as pathways, connecting the ovaries to the uterus. Each fallopian tube is made up of four distinct parts: the infundibulum, fimbriae, ampulla, and isthmus. The fimbriae are delicate, finger-like extensions that gently guide the egg from the ovary into the tube.
The Role of Fallopian tubes in Pregnancy
Moreover, fallopian tubes are critical in the earliest stages of pregnancy, integral to the reproductive process, and serve a trio of critical functions. They are the conduits for egg transportation from the ovaries to the uterus and the venue where fertilisation typically occurs. Post-fertilisation, these tubes facilitate the journey of the fertilised egg to the uterus, setting the stage for implantation and the progression of pregnancy. The health and integrity of the fallopian tubes are paramount for successful conception as they are closely linked to fertility. Problems with these tubes are a common reason why some women may have difficulty getting pregnant.
Uterine Tube Pathologies & Infertility
According to a report, nearly one-third of infertility cases are attributed to issues with the fallopian tubes, including various pathologies like inflammation and obstructions. Damage to the tube’s cilia can hinder the movement of sperm or egg, contributing to infertility. Additionally, sexually transmitted infections are a known cause of these tubal issues. Let’s dive into the specific pathologies that can manifest.
Salpingitis
Salpingitis, an inflammation in the fallopian tubes, often forms part of wider pelvic inflammatory diseases (PIDs). Its hallmark is a thickened tube in the isthmus area, known as salpingitis isthmica nodosa. This condition can resemble endometriosis, potentially leading to fertility blockages or raising ectopic pregnancy risks.
During diagnosis, doctors first look for tenderness and swelling. They may conduct blood and urine tests to spot infection indicators. Swab tests from the vagina and cervix help identify specific bacterial infections. Ultrasound scans of the fallopian tubes and reproductive tract are common. A crucial test, the hysterosalpingogram, uses a special X-ray and dye through the cervix to detect tubal blockages.
Untreated, salpingitis can cause long-term fertility issues and increase ectopic pregnancy chances. Symptoms vary, including lower abdominal pain, nausea, and fever; sometimes, no symptoms appear initially. Antibiotics typically treat this condition, but severe cases might require surgery or IVF. Seeking medical advice early is vital to prevent serious outcomes. Early detection and treatment significantly aid in managing salpingitis effectively.
Fallopian Tube Blockage & Narrowing
Addressing fallopian tube obstructions can significantly boost pregnancy chances. These blockages may develop in various parts of the tube – proximal, distal, or mid-segmental. Testing the tubes’ full functionality presents challenges, yet assessing their patency (openness) is possible with hysterosalpingography, laparoscopy with dye, or hysterosalpingo contrast sonography (HyCoSy). During surgical evaluations, specialists examine the tubes and introduce a dye, such as methylene blue, into the uterus to test its passage through the tubes when the cervix is closed.
Research published in PubMed indicates a notable prevalence of tubal obstruction: 19.1% in primary infertility cases and 28.7% in secondary infertility scenarios. The study highlights cornual blockage’s predominance in primary infertility, whereas complete hydrosalpinx and peritubal adhesions appear less frequently. Due to the frequent link between tubal disease and Chlamydia infection, Chlamydia antibody screening is now a cost-effective approach for identifying possible tubal pathologies.
At London Pregnancy Clinic, we conduct the HyCoSy procedure. This test evaluates fallopian tube functionality by injecting a special dye and monitoring its flow. It also assesses the womb for abnormalities affecting pregnancy implantation. Additionally, we use dye and ultrasound scans to check for fallopian tube blockages or abnormalities. Discover more through the slider below, offering further insights into our advanced diagnostic techniques.
-

Fallopian Tubes
-
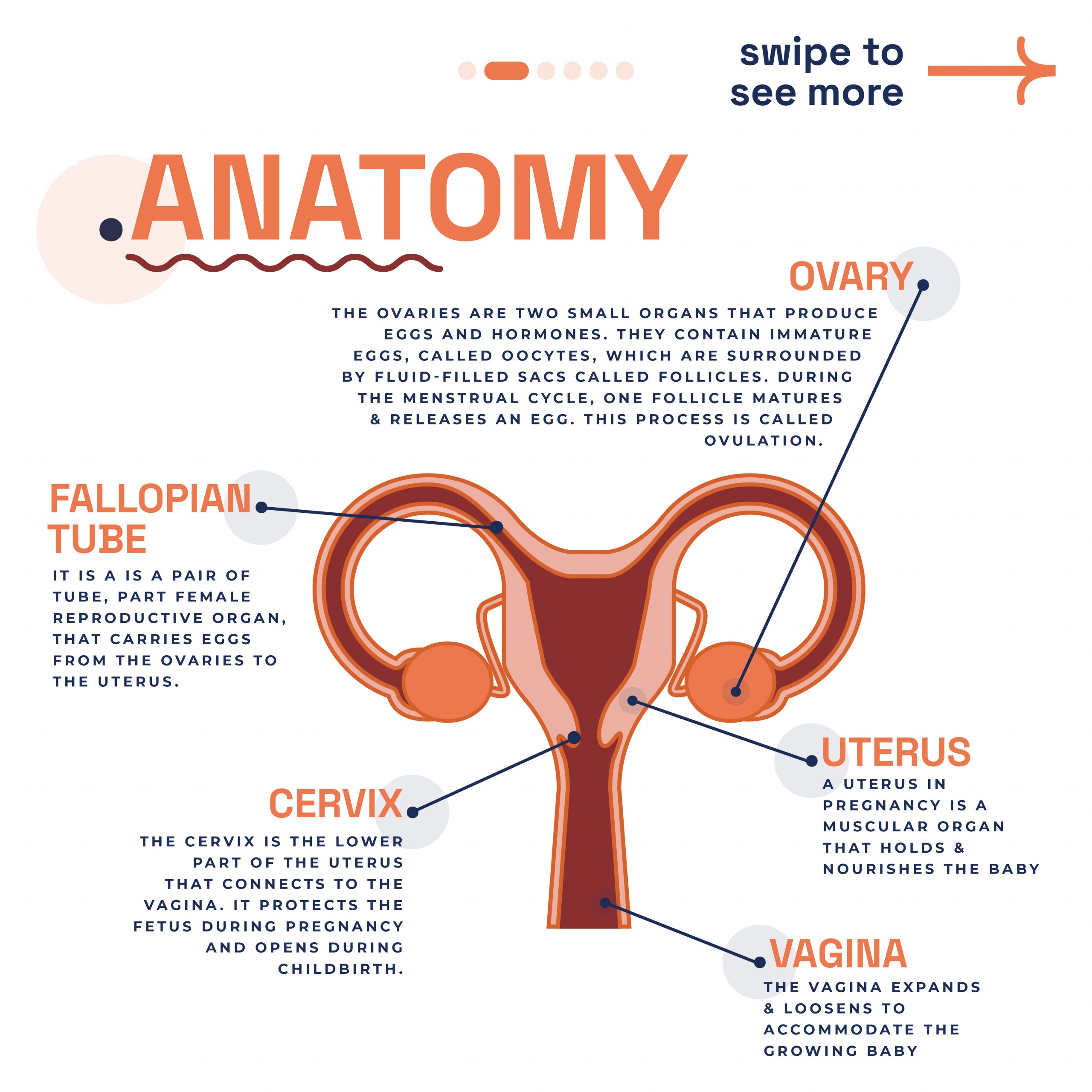
Fallopian tube diagram
-
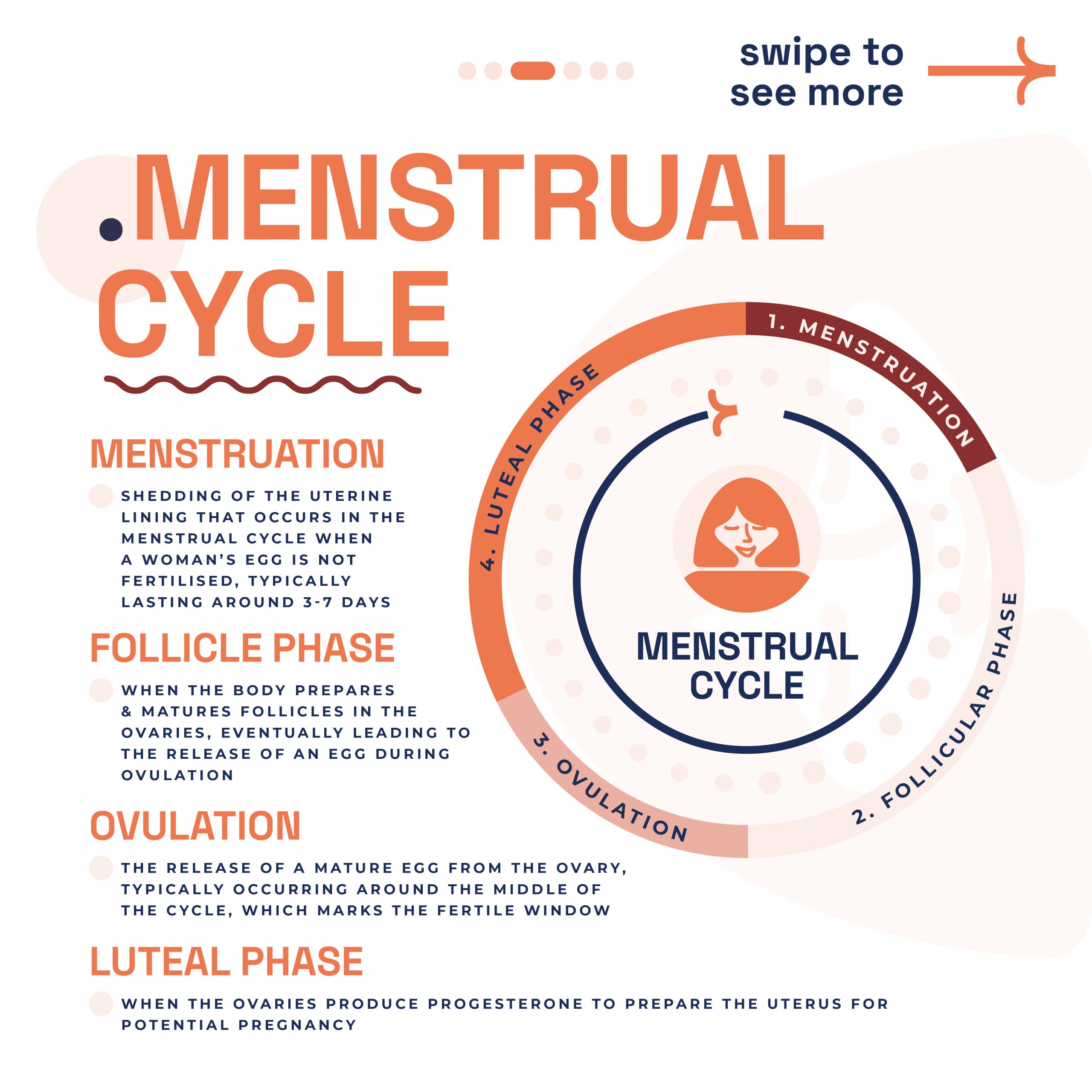
Menstrual Cycle
-
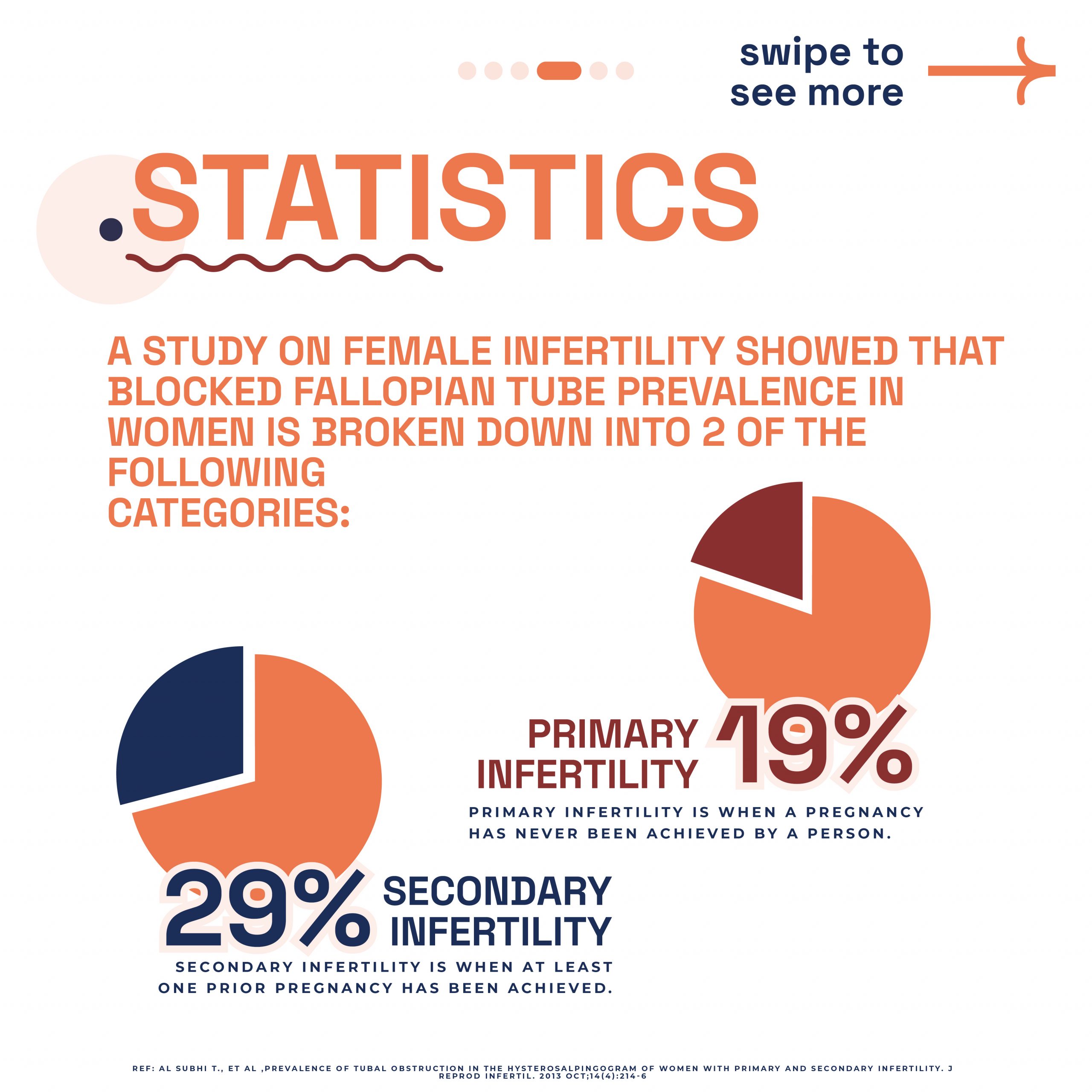
Stats on blocked fallopian tube
-
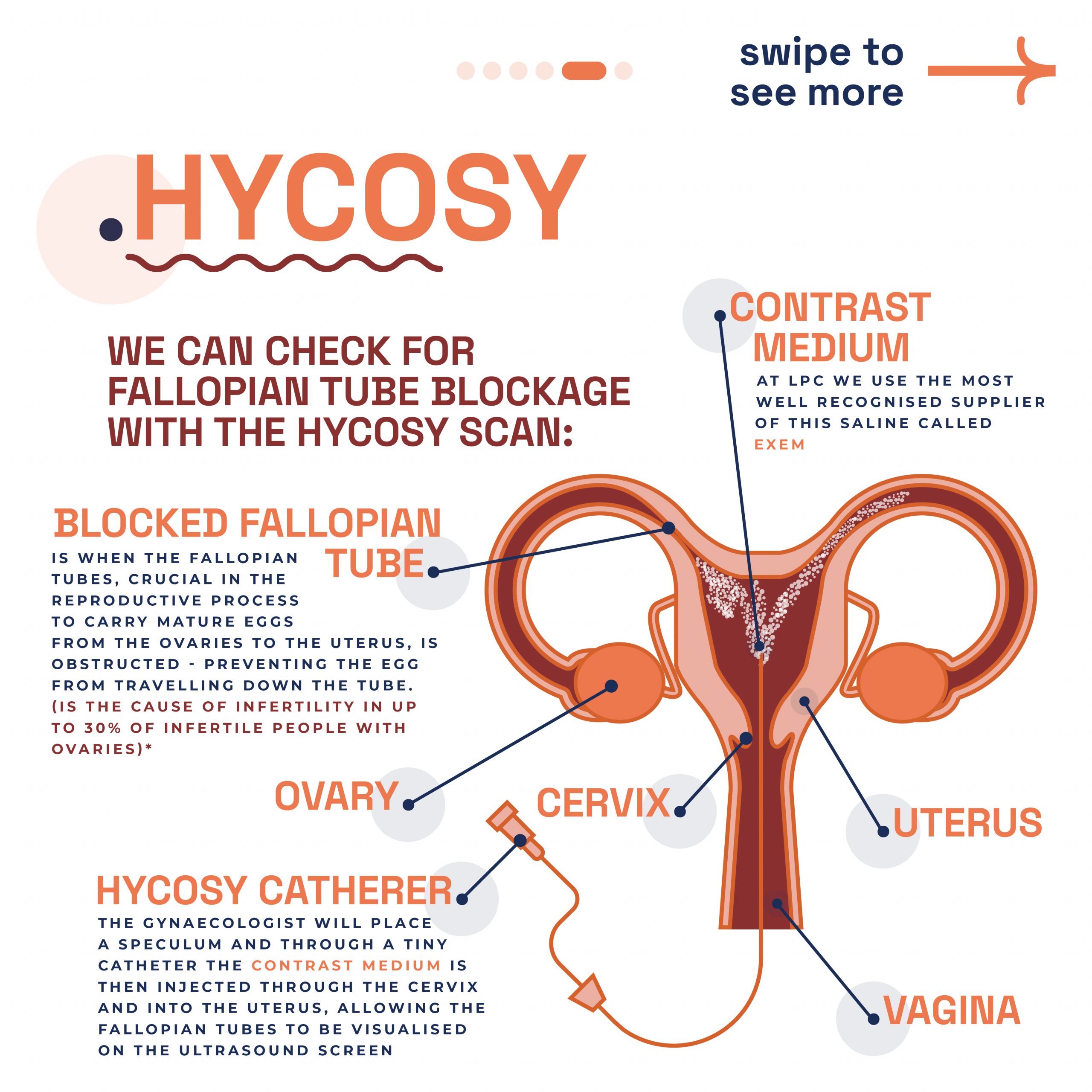
HyCoSy
-

Mr. Prashant Purohit specialist gynaecologist
Ectopic Pregnancy
Statistics and Locations of Ectopic Pregnancies: Ectopic pregnancies, which occur in about 1%-2% of all pregnancies, predominantly implant in the fallopian tubes, with over 98% of cases occurring there. Within the fallopian tubes, the distribution of ectopic pregnancies varies: approximately 75% happen in the ampullary segment, 13% in the isthmic segment, and around 12% in the fimbrial segment. These statistics highlight the critical nature of monitoring tubal health.
Fertilisation and its Relation to Ectopic Pregnancies: It’s important to note that fertilisation typically occurs in the ampulla, the same section of the fallopian tube where the majority of ectopic pregnancies are found. This correlation emphasises the need for awareness and early detection in cases of suspected ectopic pregnancy, as the ampulla is a common site for both normal fertilisation and ectopic implantation.
Understanding the statistics and locations of ectopic pregnancies in the fallopian tubes is crucial. It not only sheds light on the commonality and risks associated with these pregnancies but also underscores the importance of early ultrasound pregnancy scans for detection and intervention. The earlier you scan the quicker we can detect an ectopic pregnancy meaning that we can begin this from week 6 of pregnancy.
Pregnant with Just One Fallopian Tube?
Typically, women possess two fallopian tubes for transporting the mature egg from the ovary to the uterus, where it may encounter sperm. However, a single healthy tube can efficiently undertake this task. Remarkably, up to 85% of women aged 22-28 with only one tube successfully conceive within two years of trying, even following an ectopic pregnancy.
If you have a blocked tube due to scarring, trauma, or a previous ectopic pregnancy, your pregnancy prospects remain normal, considering other health factors. Loss of a fallopian tube might result from pelvic surgery due to infection, tumours, or a past ectopic pregnancy. In some instances, women are naturally born with just one tube. Still, pregnancy is achievable with one tube, provided you have a functioning ovary, you’re ovulating and the fallopian tube is in good health.
If you’re struggling to conceive or have a history of fallopian tube issues, it’s wise to consult your gynaecologist or a reproductive endocrinologist. They can offer a thorough evaluation to guide your next steps. Remember, one healthy fallopian tube can effectively support your journey to motherhood.
Conclusion
Mr. Prashant Purohit, our dedicated in-house gynaecologist at London Pregnancy Clinic, emphasises the need for awareness and timely medical consultation to address these concerns. His expertise in managing these conditions reflects our clinic’s commitment to providing comprehensive care and support to women facing fertility challenges. Understanding the complexities of the fallopian tubes is not just about medical knowledge; it’s about empowering women with the information they need to make informed decisions about their reproductive health. We encourage you, readers to stay vigilant about their gynaecological well-being and seek expert guidance when needed. Remember, early detection and treatment are key to overcoming obstacles on the path to motherhood.
Latest Stories
- 1
- 2