Gestational Trophoblastic Disease

Gestational Trophoblastic Disease
Published
Tags
Receiving a diagnosis of gestational trophoblastic disease can feel overwhelming and frightening for expectant parents. However, understanding this rare group of conditions and their exceptionally positive outcomes can provide much-needed reassurance during an uncertain time. Gestational trophoblastic disease encompasses several related conditions that develop from abnormal trophoblast cells — the tissue that would normally form the placenta during pregnancy.
This comprehensive guide explains what gestational trophoblastic disease involves, from the more common molar pregnancies to the rarer malignant forms, and why early detection and proper follow-up care are essential for ensuring the best possible outcomes.
Understanding Gestational Trophoblastic Disease
Gestational trophoblastic disease (GTD) is a term used for a group of pregnancy-related conditions in which abnormal cells grow inside the uterus following conception. These conditions arise from the trophoblast — the tissue that would normally develop into the placenta during a healthy pregnancy.
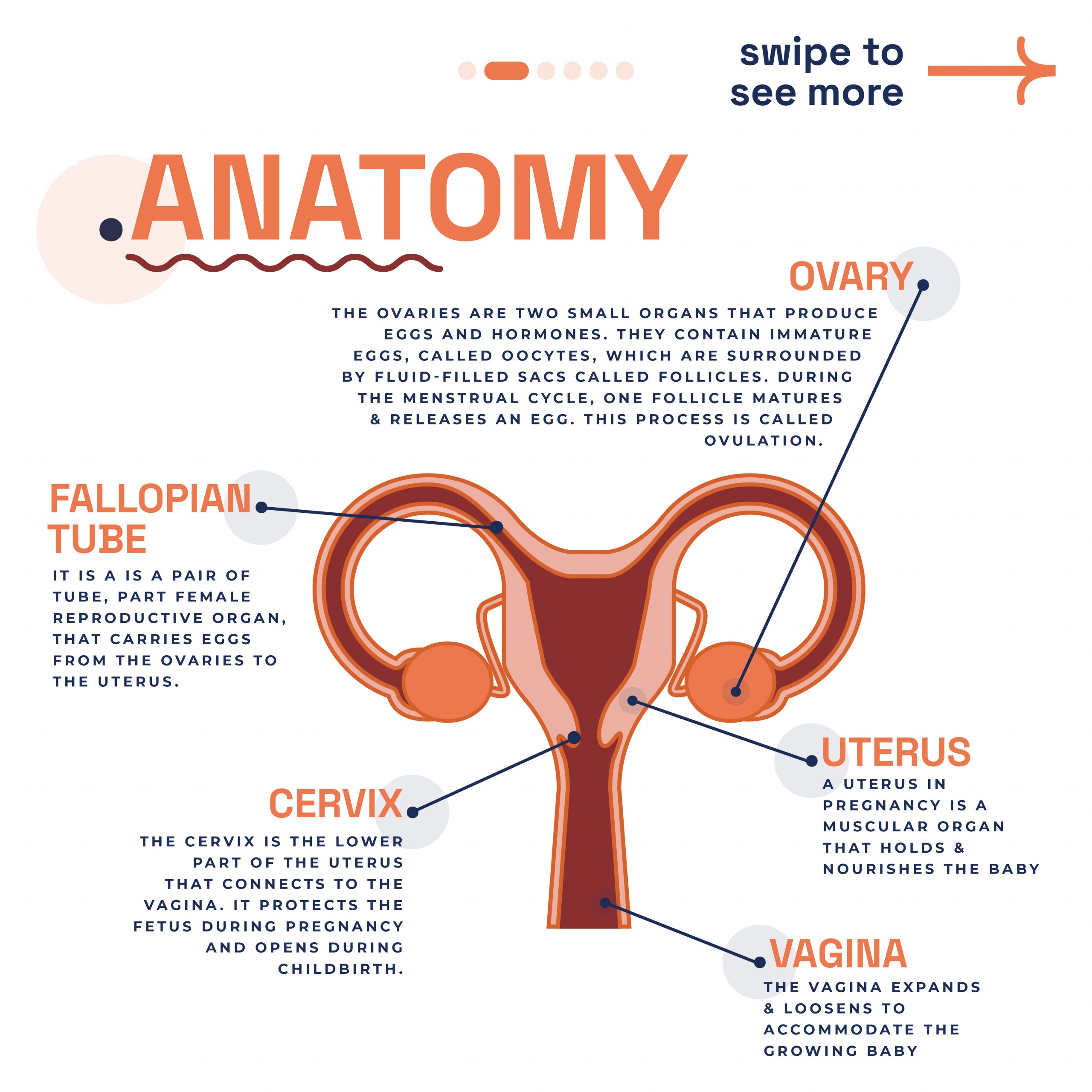
The trophoblast plays a crucial role in normal pregnancy development. After a sperm fertilises an egg, the trophoblast helps the fertilised egg implant into the uterine wall and forms part of the placenta, which nourishes the developing baby. In GTD, however, these trophoblast cells grow abnormally, creating various types of tumours rather than supporting normal fetal development.
GTD represents a spectrum of conditions ranging from benign (non-cancerous) to malignant (cancerous) forms. The most common type is hydatidiform mole, also known as molar pregnancy, which accounts for the majority of GTD cases. The rarer malignant forms include invasive moles, choriocarcinoma, placental site trophoblastic tumours, and epithelioid trophoblastic tumours.
Types of Gestational Trophoblastic Disease
Hydatidiform Moles (Molar Pregnancies)
Hydatidiform moles are the most common type of GTD and are typically benign. These occur when fertilisation goes wrong, creating abnormal cells or clusters of fluid-filled sacs inside the womb rather than a healthy pregnancy. Molar pregnancies cannot develop into viable babies.
There are two types of hydatidiform moles:
Complete hydatidiform moles form when sperm fertilises an egg that contains no maternal DNA. Most commonly, a single sperm duplicates itself to fertilise an empty egg, though sometimes two separate sperm fertilise the empty egg. No fetal tissue develops in complete moles.
Partial hydatidiform moles occur when two sperm fertilise a normal egg, resulting in abnormal genetic material with three sets of chromosomes instead of the normal two. Some fetal tissue may develop, but it cannot grow normally.
Gestational Trophoblastic Neoplasia (GTN)
Gestational trophoblastic neoplasia refers to the malignant forms of GTD. These are much rarer than molar pregnancies but require more intensive treatment.
Invasive moles develop when trophoblast cells from a molar pregnancy grow into the muscle layer of the uterus. They are more likely to grow and spread than regular hydatidiform moles.
Choriocarcinoma is a malignant tumour that can spread to the muscle layer of the uterus and nearby blood vessels. It may also spread to other parts of the body, including the brain, lungs, liver, and other organs. Choriocarcinoma can occur after any type of pregnancy, including normal pregnancies, miscarriages, or molar pregnancies.
Placental site trophoblastic tumours (PSTT) and epithelioid trophoblastic tumours (ETT) are extremely rare forms of GTN that develop where the placenta attaches to the uterus. These tumours grow very slowly and may not cause symptoms for months or years after pregnancy.
Gestational Trophoblastic Disease Symptoms: What to Look For
The symptoms of GTD can initially mimic those of a normal pregnancy, which often delays diagnosis. The most common signs include:
Abnormal vaginal bleeding is the most frequent symptom, occurring in most women with GTD. This bleeding may be heavier than normal menstrual periods and can contain grape-like clusters of tissue.
Enlarged uterus that is larger than expected for the stage of pregnancy is another common finding. Healthcare providers may notice this during routine examinations.
Severe nausea and vomiting (hyperemesis) that is more intense than typical morning sickness affects many women with GTD.
High blood pressure with headaches and swelling of the feet and hands may develop early in pregnancy, which is unusual for normal pregnancies.
Pelvic pain or pressure can occur as the abnormal tissue grows within the uterus.
Some women may also experience symptoms of hyperthyroidism, including rapid heartbeat, shakiness, sweating, and weight loss. This occurs because the abnormally high levels of hCG hormone can stimulate the thyroid gland.
Gestational Trophoblastic Disease Diagnosis and Testing
Diagnosing GTD involves several tests and examinations. The key diagnostic tool is measuring levels of human chorionic gonadotropin (hCG) in the blood. This hormone is normally produced during pregnancy, but in GTD, levels are often abnormally high.
Ultrasound examination is crucial for diagnosis. In molar pregnancies, ultrasound typically shows a characteristic “snowstorm” pattern of fluid-filled sacs instead of normal fetal development. The ultrasound can also help identify the size and extent of abnormal tissue.
A pelvic examination may reveal an enlarged uterus that doesn’t match the expected size for the stage of pregnancy. Healthcare providers will also check for other signs of GTD during this examination.
Blood tests beyond hCG measurement help assess overall health and check for complications. These may include tests for anaemia, thyroid function, and blood clotting ability.
Once GTD is suspected, tissue samples obtained during treatment can provide definitive histological confirmation of the diagnosis and determine the specific type of GTD present.
Treatment Options and Prognosis
The treatment approach for GTD depends on the specific type and extent of disease. For hydatidiform moles, the primary treatment involves evacuation of the abnormal tissue from the uterus, typically performed using suction curettage under general anaesthesia.
For women who don’t wish to have future pregnancies, hysterectomy may be considered as an alternative treatment option. However, this is rarely necessary, as most women can be successfully treated while preserving their fertility.
Malignant forms of GTD, including invasive moles and choriocarcinoma, usually require chemotherapy treatment. The specific chemotherapy regimen depends on various factors, including the extent of disease and risk factors. Common chemotherapy drugs include methotrexate and dactinomycin.
The prognosis for all forms of GTD is exceptionally positive. Even the malignant forms are among the most curable of all gynaecological cancers. Women with hydatidiform moles have an excellent prognosis, while those with malignant GTD typically have excellent cure rates when managed at specialist centres.
The Importance of Follow-Up Care and hCG Monitoring
Follow-up care is absolutely essential for all women diagnosed with GTD. This monitoring involves regular blood tests to measure hCG levels, which should gradually decrease and return to normal after successful treatment.
The UK operates a nationally coordinated follow-up programme. Specialist centres at Charing Cross Hospital in London, Sheffield, and Dundee provide this service. This system ensures every woman with GTD receives expert monitoring and care throughout recovery.
During the follow-up period, reliable contraception is essential. Pregnancy during this time could make it difficult to distinguish between rising hCG levels due to new pregnancy versus persistent or recurrent GTD.
The duration of follow-up varies depending on the type of GTD and how quickly hCG levels normalise. For most women with molar pregnancies, follow-up continues until hCG levels have been normal for several months. Those who receive chemotherapy may require longer monitoring periods.
Women who have had GTD should also have hCG levels checked after any future pregnancies to ensure no reactivation of the condition has occurred.
Living with Gestational Trophoblastic Disease
A diagnosis of GTD can be emotionally challenging, particularly as it often occurs when couples are expecting a normal pregnancy. The loss of the anticipated pregnancy, combined with concerns about cancer and fertility, can create significant emotional distress.
Support from healthcare teams, family, and friends is crucial during this time. Many women find it helpful to connect with others who have experienced similar diagnoses through support groups or online communities.
Fertility is typically preserved after treatment for GTD. Most women can go on to have successful pregnancies once their follow-up care is complete and they receive clearance from their healthcare team.
The excellent cure rates and fertility preservation associated with GTD treatment provide hope and reassurance for women facing this diagnosis. With proper treatment and follow-up care, the vast majority of women make complete recoveries and can pursue their family planning goals in the future.
Understanding gestational trophoblastic disease and its management can help reduce anxiety and ensure that women receive the comprehensive care they need. At London Pregnancy Clinic, our experienced team provides expert gestational trophoblastic disease guidance and support throughout the diagnostic process and beyond.