Week 10 of Pregnancy
Week 10 of your Pregnancy
Discovering your baby’s progress since week 10
-
Published
-
Last Modified
Tags
At 10 weeks, your pregnancy reaches a significant stage of development. Your baby has now officially transitioned from an embryo to a fetus, and their growth is accelerating. With each passing day, vital organs mature, facial features become more defined, and tiny fingers and toes take shape. Though still small, about the size of a prune, your baby is now moving more actively inside the womb.
For many expectant parents, this is an ideal time to book a private early pregnancy scan. At London Pregnancy Clinic, we provide high-resolution ultrasound imaging to track your baby’s progress, offering reassurance and detailed insights. This is also the earliest point for non-invasive prenatal testing (NIPT), which can screen for chromosomal conditions and determine the baby’s sex.
Pregnancy Checklist at 9 Weeks
- Book and attend your private early pregnancy scan: Capturing clear images during the 6-9 week Viability Scan is crucial for assessing your baby’s development and health. These dating Scans are pivotal, offering crystal-clear imagery that plays a crucial role in monitoring your baby’s development and ensuring their health. Beyond the clinical benefits, these scans foster a profound emotional bond, providing expectant parents with a reassuring glimpse into their baby’s growth and vitality.
- Prioritise Health and Well-being: Your health directly impacts your baby’s growth. Eat well, stay active with gentle exercise, and heed your healthcare provider’s advice.
- Communication with healthcare professionals: Regular communication with medical professionals is crucial. They offer invaluable support and guidance through physical and hormonal changes. Trust them to make your pregnancy journey informed and smooth.
- Book Your Antenatal Appointment: If you’ve not yet booked your first antenatal appointment, now’s the time. The NHS offers thorough antenatal care, starting with this vital step. Alternatively, London Pregnancy Clinic’s early private midwifery services offer customised care, tailored to your pregnancy. Use this appointment to voice queries and concerns, laying the groundwork for a healthy pregnancy.
- Non-Invasive Prenatal Testing (NIPT): Consider NIPT, a screening that analyses the baby’s genetic information through a simple blood test from the mother. Mostly available from as early as 10 weeks, NIPT can detect certain genetic conditions and determine the baby’s sex. It’s a non-invasive way to gain early insights into your baby’s health and development. Discuss the option of NIPT with your healthcare provider to understand its benefits and whether it’s right for you. If you want to do the earliest possible NIPT we offer Panorama NIPT which can be done from week 9.
Developmental Milestones: Week 9
Embryonic Growth: At this stage, your baby measures between 23 to 31 mm from crown to rump (CRL), which is around the size of an olive. The embryonic shape evolves, with fingers and toes becoming more defined, moving away from their initial webbed appearance.
Gestational and Yolk Sac aDevelopment: According to Nature, By week 9, the gestational sac typically measures between 35-40 mm, with the yolk sac around 3.6 mm.
Heart Development: The fetal heart rate continues to slightly increase to an average of 140-170 beats per minute (BPM) and will gradually stabilise around 12 weeks. These statistics vary from person to person that’s why the range is so large.
Brain + Neural Development: By week 9, the neural tube closes, a vital step in the baby’s brain and spinal cord development. This lays the groundwork for the central nervous system. The brain’s rapid growth sees specific areas forming, enhancing its structure and complexity. Electrical activity starts by week 6, with significant development continuing into the first trimester.
Other Development: Your baby’s facial features, like closed eyes, mouth, tongue with taste buds, and ear lobes, are shaping up. The liver starts making blood cells, and blood vessels form under the skin. The genital tubercle, visible in all embryos, indicates a key point in gender development, observable in both 2D and 3D ultrasounds.
Umbilical cord: In week 9 of pregnancy, the umbilical cord becomes the baby’s vital connection to the placenta. It comprises one vein and two arteries, twined together, that transport crucial nutrients and oxygen to support the baby’s growth. The umbilical cord’s formation starts around week 3 from a connecting stalk, evolving into the mature cord by week 7. This structure, with its gelatinous coating, ensures the efficient exchange between mother and baby.
What is seen on the Ultrasound: Week 9?
As you enter week 9 of your pregnancy journey, an early pregnancy scan offers an enriched, detailed view of your baby’s development, a process both miraculous and fascinating. This period marks a significant milestone in your little one’s growth, as the ultrasound reveals the intricate formation of their tiny body, from the rhythm of the heartbeat to the delicate shaping of limbs and facial features. Perhaps most heartwarming is the possibility of observing movements, especially in the torso, as your baby starts to stretch and wriggle.
A week prior, black spots within your baby’s head signalled the initial stages of brain development. Now, these spaces are filled by the choroid plexus, visible as white spots on the ultrasound. This transition is vital for the growth of the brain’s primary divisions—forebrain (prosencephalon), midbrain (mesencephalon), and hindbrain (rhombencephalon)—laying the foundation for future cognitive and motor skills, emotions, and memories.
Also captured in the ultrasound is the growth of the placenta, depicted as two white lines framing the gestational sac. This organ is indispensable, serving as the lifeline that supplies essential nutrients and oxygen to your baby via the umbilical cord. Its presence and development are reassuring indicators of the pregnancy’s health and progression.
By week 9, the genital tubercle is visible in all embryos, signifying a key phase in gender development. Visible via 2D or 3D ultrasound, its clarity improves with transvaginal scans. This method provides high-resolution images, offering a clear glimpse of early baby movements. While each pregnancy is unique, ultrasound scans follow a similar process. As time goes on, the genital tubercle evolves into either a penis or a clitoris, marking the baby’s gender.
-
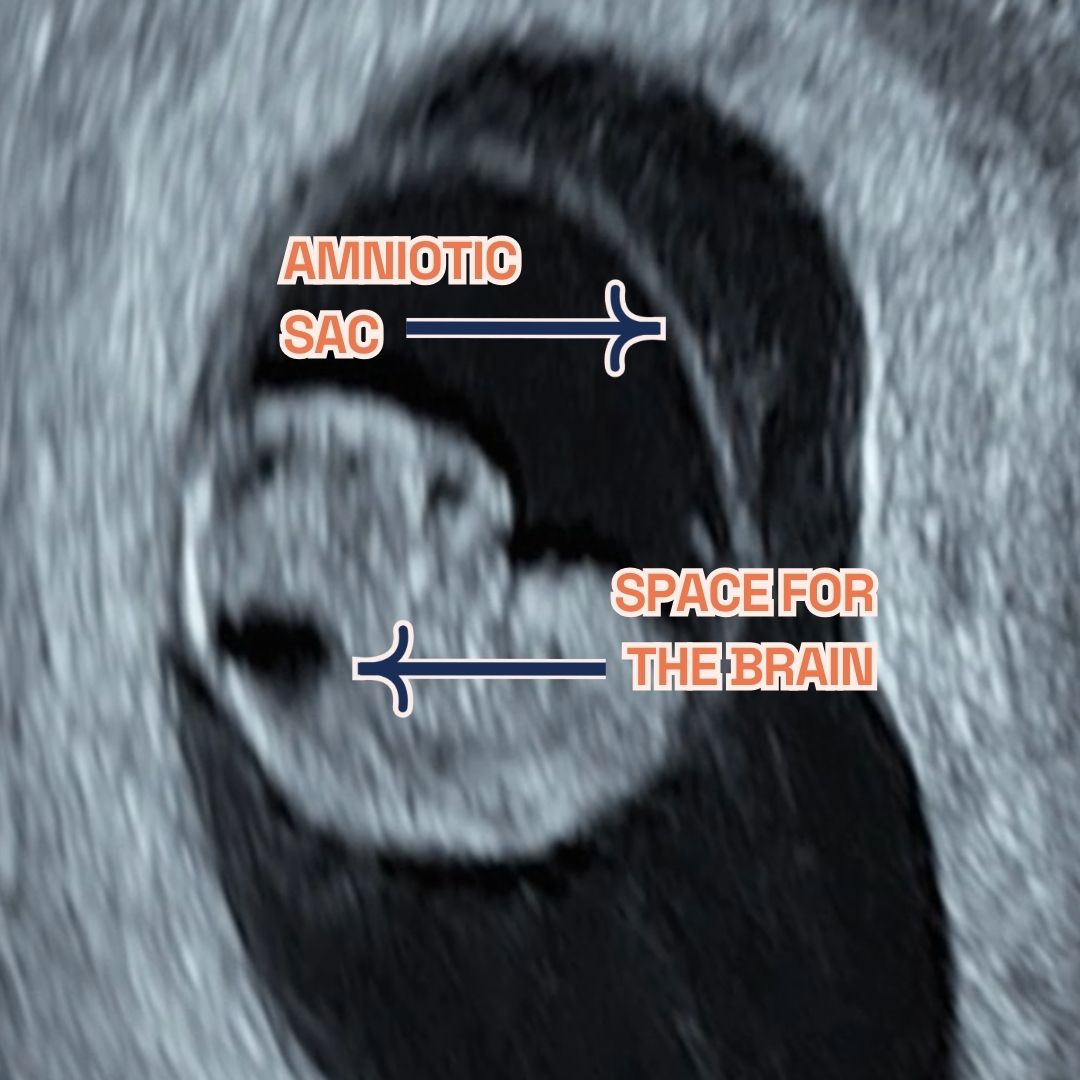
Gestational sac, fetal pole and amniotic sac at 8 weeks of pregnancy as seen on ultrasound scan.
-
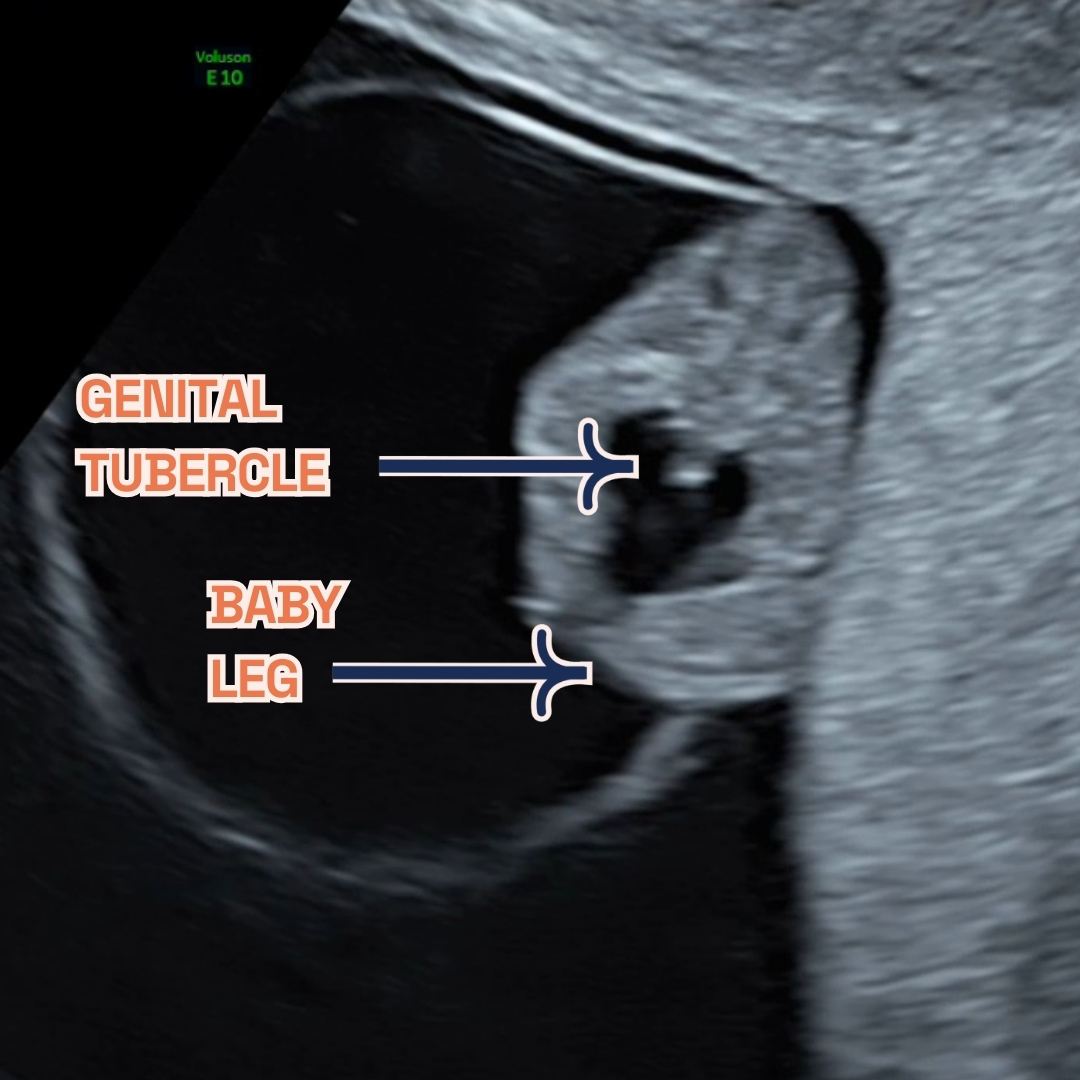
Gestational sac, fetal legs and Genital Tubercle at 9 weeks of pregnancy as seen on ultrasound scan.
Thinking ahead: Week 10?
Around 10 weeks into pregnancy, some women might had their initial ultrasound scan already. This scan helps confirm the due date by measuring the baby’s size and checks for multiple births or genetic conditions like Down’s syndrome risk. It’s crucial to keep regular prenatal check-ups and share any concerns with healthcare professionals for proper advice during pregnancy. Discuss the option of a NIPT with your doctor. Available from week 10, this test screens for chromosomal abnormalities and can reveal the baby’s sex.
You may be considering our innovative 10 Week Scan, it’s important to note that this is distinct from the usual viability or dating scans you might be familiar with. Specifically designed for 10-11 weeks of pregnancy, this scan acts as the earliest anomaly check, providing parents with early reassurance by screening for significant physical abnormalities. It marks the first opportunity for a structural examination of the baby, at the earliest stage possible. This timing also makes it the optimal period for non-invasive prenatal testing (NIPT), leveraging our blend of professional expertise and the latest in ultrasound technology to deliver results with unmatched clarity. Compared to the standard NHS 12 week scan, our 10-week scan offers a more comprehensive checklist, ensuring nothing is overlooked.
Remember, NIPT indicates the likelihood of certain conditions, unlike amniocentesis or chorionic villus sampling (CVS), which provide definitive results but are invasive. Always check if your insurance covers NIPT. For those over 35 or with a family history of genetic conditions, consider NIPT, CVS (done between 10 and 13 weeks), and amniocentesis (usually between weeks 15 to 20). The likelihood of a baby having a chromosomal condition, such as aneuploidy, rises with maternal age, notably after 35 years, termed “advanced maternal age.”
Week 9: Your body?
Alongside fetal developments, maternal changes may be observed during the ultrasound. Increased blood volume and fluid retention can lead to frequent urination. Hormonal fluctuations may cause symptoms like headaches, low blood pressure, constipation, and fatigue. These changes reflect the body’s adaptation to support the growing fetus during pregnancy.
Keep hydrated by drinking plenty of water, aiming to drink more in the morning to avoid nighttime trips to the loo. At 9 weeks, you might struggle to fasten your jeans as your uterus expands, doubling in size to accommodate your growing baby. You may even start to show a little. As the weeks progress, your uterus will grow beyond your pelvis. Gaining weight now is not just normal—it’s advisable. Your ideal weight gain during pregnancy depends on your pre-pregnancy BMI. Generally, with a normal BMI, you’d be expected to gain 25 to 35 pounds throughout, with one to five pounds in the first trimester.
However, morning sickness and food aversions may lead to weight loss instead of gain at this stage. Discuss any weight concerns, gain or loss, especially if changes are sudden or severe, with your obstetrician or midwife. Minor weight loss is often seen as acceptable early on. As your appetite returns, there’ll be chances to get your weight gain on track. Severe nausea may require medical intervention. Many under-report nausea and vomiting, but numerous safe Over-The-Counter and prescription options can manage symptoms.
Week 9 of Pregnancy FAQs
-
what happens during week 9 of pregnancy?
At 9 weeks pregnant, your body and baby undergo significant changes. Not everyone experiences the same symptoms, ranging from hair thickening—due to reduced shedding and possibly healthier lifestyles including prenatal vitamins—to bloating, caused by increased progesterone slowing digestion.
An early scan reveals your baby’s rapid growth, from forming hands and feet to facial features developing, and even early movements. The scan also shows the brain’s development, the steady heartbeat indicating a strong cardiovascular system, and the placenta’s vital role in providing nutrients. The genital tubercle’s visibility marks the beginning of gender development, becoming clearer with transvaginal scans.
-
spotting during week 9 of pregnancy?
Spotting in week 9 of pregnancy is commonly seen and typically isn’t a cause for concern. Light bleeding or spotting can be normal in the first trimester. Nonetheless, consulting your midwife or healthcare provider for a check-up is always wise to dismiss any potential issues.
Usually, spotting isn’t alarming, but monitoring the situation and getting medical advice if the bleeding gets heavy or continuous is vital. Keeping in contact with your healthcare provider during your pregnancy is crucial to quickly address concerns and safeguard the health of you and your baby.
Every pregnancy is distinct, and although spotting can be standard, consulting your healthcare provider for tailored advice and reassurance is always recommended.
-
why is week 9 of pregnancy the worst?
Week 9 of pregnancy might bring challenges due to physical and hormonal changes. Your breasts may enlarge and your waist could thicken as your uterus grows. High levels of pregnancy hormones may cause discomfort and morning sickness. These symptoms are often temporary and improve by the second trimester. Nausea and vomiting, known as “morning sickness,” can happen any time. This is often due to the rise in human chorionic gonadotropin (hCG), peaking around week 10. So, the most intense nausea might occur between now and next week. Additionally, increased progesterone can make your breasts larger or swollen.
-
Common symptoms during nine weeks pregnant
Feeling early flutters at 8 weeks? Expect:
- Fatigue: Your body is working hard, so tiredness is typical. Make rest a priority.
- Frequent urination: Your expanding uterus presses on the bladder, meaning more loo visits.
- Morning sickness: Nausea and vomiting might strike any time. Keep hydrated and seek relief methods.
- Enhanced senses: You may experience metallic tastes or strong smells. It’s all part of the journey!
- Mood swings: Hormonal changes may affect your emotions. Treat yourself gently.
- Sore breasts: Hormones are prepping for breastfeeding, causing discomfort.
- Bloating and cramping: These are signs of your growing uterus.
- Light spotting: It’s rare but can occur. Contact your doctor if worried.
- Other signs: Thicker hair, skin changes, or milky discharge are normal during pregnancy.
Each pregnancy differs. Some women get many symptoms; others have few. Always consult your healthcare provider with concerns. Consider a private midwife consultation for worries.
-
Can I do NIPT at 9 weeks of pregnancy?
Non-invasive prenatal testing (NIPT)
can start at 9 weeks into pregnancy. It’s a safe, accurate way to screen for chromosomal abnormalities like Down’s, Edwards’, and Patau’s syndromes. By analysing the mother’s blood for cell-free DNA, NIPT gauges the fetus’s risk for specific genetic conditions without miscarriage risks, ensuring early detection and reassurance. We advise waiting until week 10 for NIPT, allowing it to coincide with our 10-week scan for optimal results.
NIPT stands out for its precise detection of chromosomal disorders, showing high sensitivity for conditions such as Down’s syndrome. Early testing allows for informed decisions and tailored prenatal care. Discussing NIPT with your healthcare provider is crucial to see if it suits your needs and to understand test implications.
Benefits of NIPT include:
- Non-invasive with no risk to the baby.
- High accuracy for peace of mind.
- Early detection for proactive decision-making.
- Optional sex determination for early family planning.
Remember: NIPT is a screening test, not a definitive diagnosis. Consult your healthcare provider for further information and personalised guidance. We at LPC offer multiple NIPTs (PrenatalSafe, Panorama, Unity, SMART TEST, Illumina,
Harmony) and out specialists will help you choose the best option for you!
Final Thoughts
Week 9 is a time of remarkable progress, and London Pregnancy Clinic is here to guide and support you through every step. With each visit, you’ll gain deeper insights into your baby’s development, reinforcing the bond you share. Embrace this journey with confidence, knowing we’re by your side.
Stay informed and excited about what each new week will reveal about your baby’s growth on our blog.
Latest Stories
What Is an AFC Scan and What Does Your Antral Follicle Count Mean for Your Fertility?

What Is an AFC Scan and What Does Your Antral Follicle Count Mean for Your Fertility?
Published
Tags
Understanding your fertility potential is a crucial step in family planning, and one of the most valuable assessments available is the antral follicle count (AFC) scan. This specialised fertility screening provides essential insights into your ovarian reserve, helping to guide treatment decisions and predict how you might respond to fertility treatments. With approximately one in seven couples in the UK experiencing fertility difficulties, AFC scans have become an indispensable tool for fertility specialists and patients alike.
What Is an AFC Scan?
An antral follicle count (AFC) scan is a specialised transvaginal ultrasound examination that measures the number of antral follicles visible in both ovaries. Antral follicles are small, fluid-filled sacs measuring 2-9mm in diameter, each containing an immature egg. These follicles appear as dark, roughly circular areas on the ultrasound screen and represent your ovarian reserve – essentially, the number of eggs remaining in your ovaries.
The AFC scan is considered one of the gold standard methods for assessing ovarian reserve, alongside hormone blood tests such as anti-Müllerian hormone (AMH). Unlike blood tests that can fluctuate, the AFC provides a direct visual assessment of your ovaries’ current state. This transvaginal scan is typically performed during the early follicular phase of your menstrual cycle, usually between days 2-4, when hormone levels are at their baseline.
The procedure itself is straightforward and similar to other transvaginal ultrasounds. A small ultrasound probe is gently inserted into the vagina, providing clear, detailed images of the ovaries. The sonographer can then count the visible antral follicles in each ovary, providing an accurate assessment of your ovarian reserve.
Understanding Normal AFC Ranges
Antral follicle count results are typically categorised into different ranges that indicate varying levels of ovarian reserve. Understanding these ranges can help you interpret your results and discuss treatment options with your fertility specialist.
- Low AFC (3-6 total follicles): Indicates diminished ovarian reserve and may suggest a reduced response to fertility treatments.
- Normal AFC (7-15 total follicles): Represents a healthy ovarian reserve with good potential for natural conception and fertility treatment success.
- High AFC (16-24 total follicles): Suggests excellent ovarian reserve but may increase the risk of ovarian hyperstimulation syndrome during fertility treatments.
- Very high AFC (25+ total follicles): May indicate polycystic ovary syndrome (PCOS) and requires careful management during fertility treatments.
It’s important to note that these ranges can vary slightly between different clinics and medical guidelines. The RCOG recognises that individual circumstances vary, and your fertility specialist will interpret your results in the context of your age, medical history, and other fertility factors. A pelvic scan may also be recommended to assess the overall structure and health of your reproductive organs.
Why AFC Matters for Your Fertility
Your antral follicle count provides crucial information about several aspects of your fertility potential. Understanding these implications can help you make informed decisions about family planning and treatment options.
Firstly, AFC serves as a predictor of ovarian response to fertility medications. Women with higher AFCs typically produce more eggs during ovarian stimulation, whilst those with lower counts may require adjusted medication protocols or different treatment approaches. This information is invaluable for fertility specialists planning IVF cycles or other assisted reproductive treatments.
The AFC also helps predict the likelihood of pregnancy success with various fertility treatments. Research indicates that women with very low AFCs may have reduced live birth rates, whilst those with normal to high counts generally have better prognosis. Additionally, AFC can help identify women at risk of ovarian hyperstimulation syndrome (OHSS), allowing specialists to adjust treatment protocols accordingly.
For women considering egg freezing, AFC provides essential information about the optimal timing and expected outcomes. A higher AFC suggests that more eggs can potentially be retrieved and frozen, improving future fertility options. This assessment is particularly valuable for women who wish to preserve their fertility for personal or medical reasons.
When Should You Have an AFC Scan?
Several circumstances may warrant an AFC scan as part of your fertility assessment. Understanding when this test is recommended can help you seek appropriate care at the right time.
Women experiencing difficulty conceiving after six months of trying (if over 35) or twelve months (if under 35) should consider comprehensive fertility testing, including an AFC scan. This assessment provides valuable baseline information that can guide further investigations and treatment decisions.
AFC scans are also recommended before starting any fertility treatments, including IVF, intrauterine insemination (IUI), or ovarian stimulation. The results help fertility specialists tailor medication doses and treatment protocols to your individual needs, optimising both safety and success rates.
Women with irregular menstrual cycles, suspected PCOS, or family history of early menopause may benefit from AFC assessment. Additionally, if you’re considering egg freezing or have concerns about your fertility potential, an AFC scan can provide valuable insights to inform your decisions. The scan works well alongside follicle tracking scans during treatment cycles.
The AFC Scan Procedure: What to Expect
Understanding what happens during an AFC scan can help alleviate any anxiety and ensure you’re properly prepared for the appointment. The procedure is straightforward, typically taking 15-20 minutes to complete.
You’ll be asked to undress from the waist down and lie on an examination couch with your knees bent and feet in stirrups, similar to a cervical screening position. The sonographer will insert a thin ultrasound probe, covered with a protective sheath and gel, gently into your vagina. This provides clear, detailed images of your ovaries on the ultrasound screen.
The sonographer will systematically examine both ovaries, counting the visible antral follicles and measuring your ovaries’ size and structure. You may feel slight pressure during the examination, but the procedure shouldn’t be painful. Many women find it helpful to empty their bladder before the scan for comfort.
Results are typically available immediately after the scan, and the sonographer or specialist can discuss the findings with you straight away. You’ll receive a detailed report that can be shared with your GP or fertility specialist for further treatment planning. This comprehensive assessment complements other fertility investigations you may have undergone.
Factors That Can Affect Your AFC
Several factors can influence your antral follicle count, some of which are modifiable whilst others are not. Understanding these factors can help you interpret your results and potentially improve your fertility outcomes.
Age is the most significant factor affecting AFC, with counts naturally declining as women get older. This decline accelerates after age 35, with more rapid decreases typically occurring in the early forties. However, there’s considerable individual variation, and some women maintain good AFCs longer than others.
Hormonal contraceptives, particularly the combined oral contraceptive pill, can temporarily suppress AFC measurements. If you’re taking hormonal contraception, your specialist may recommend stopping it for 1-3 months before the AFC scan for more accurate results. Other factors including smoking, certain medications, previous ovarian surgery, and medical conditions like endometriosis can also impact your AFC.
Lifestyle factors such as stress, poor nutrition, excessive exercise, and environmental toxins may negatively affect ovarian reserve. Whilst you cannot change your age or genetic factors, addressing modifiable risk factors may help optimise your fertility potential and overall reproductive health.
AFC Results and Treatment Planning
Your AFC results play a crucial role in determining the most appropriate fertility treatment approach for your individual circumstances. Fertility specialists use this information alongside other factors to develop personalised treatment plans.
For women with low AFCs, treatment protocols typically involve higher doses of fertility medications or alternative approaches such as natural cycle IVF or donor egg treatment in some cases. The focus shifts to maximising the quality of available eggs rather than quantity, and specialists may recommend proceeding with treatment sooner rather than later.
Normal AFC results generally indicate good treatment prospects, with standard stimulation protocols likely to be effective. Women in this category often have multiple treatment options available and may choose to delay treatment if desired, though age-related factors should still be considered.
High AFCs require careful management to prevent ovarian hyperstimulation syndrome. Treatment protocols typically use lower medication doses, close monitoring throughout the cycle, and sometimes alternative trigger medications. Women with very high AFCs and suspected PCOS may need additional assessments and specialised treatment approaches. Follicle tracking scans become particularly important during treatment cycles.
AFC and Age: Understanding the Connection
The relationship between age and antral follicle count is one of the most important aspects to understand when interpreting your results. This connection has significant implications for fertility potential and treatment planning.
Women are born with all the eggs they’ll ever have, approximately 1-2 million at birth. This number continuously declines throughout life, falling to around 400,000 at puberty and continuing to decrease at an accelerating rate. By age 37, most women have only about 25,000 eggs remaining, with this number dropping to approximately 1,000 by age 51.
AFC generally correlates with this natural decline, but there’s considerable individual variation. Some women in their late thirties may have AFCs similar to women in their twenties, whilst others may show earlier declines. This variability makes individual assessment crucial rather than relying solely on age-based predictions.
Understanding your personal AFC in relation to your age helps set realistic expectations for treatment outcomes. A 35-year-old with a high AFC may have better treatment prospects than a 30-year-old with a low AFC, highlighting the importance of individualised assessment and counselling throughout the fertility journey.
Limitations and Considerations of AFC Testing
Whilst AFC scans provide valuable fertility information, it’s important to understand their limitations and what they cannot tell you about your reproductive potential.
AFC primarily indicates quantity rather than quality of eggs. A high antral follicle count doesn’t guarantee that the eggs are chromosomally normal or capable of developing into healthy embryos. Egg quality is more closely related to age, and even women with low AFCs can achieve pregnancy with good-quality eggs.
The scan also cannot predict natural conception rates with certainty. Some women with low AFCs conceive naturally, whilst others with normal counts may experience fertility difficulties due to other factors such as tubal blockages, male factor infertility, or unexplained infertility.
AFC measurements can vary between different operators and ultrasound machines, and results may fluctuate slightly between cycles. It’s important to have scans performed by experienced sonographers using high-quality equipment. Additionally, certain conditions like ovarian cysts or recent ovulation can affect follicle visibility and counting accuracy. Your specialist will consider these factors when interpreting your results alongside other fertility assessments and your medical history.
Improving Your Fertility Outcomes
Regardless of your AFC results, there are several steps you can take to optimise your fertility potential and improve treatment outcomes. These recommendations apply to all women trying to conceive, whether naturally or through assisted reproduction.
Maintaining a healthy lifestyle forms the foundation of fertility optimisation. This includes following a balanced diet rich in folate, vitamin D, and antioxidants, achieving and maintaining a healthy weight, engaging in regular moderate exercise, and avoiding smoking and excessive alcohol consumption. These factors can positively impact both egg quality and overall reproductive health.
Managing stress through relaxation techniques, counselling, or support groups can also be beneficial. Chronic stress may negatively affect hormone levels and ovulation, potentially impacting fertility outcomes. Ensuring adequate sleep and managing underlying health conditions such as diabetes or thyroid disorders are equally important.
Timing is crucial in fertility treatment, particularly for women with low AFCs. Don’t delay seeking specialist advice if you have concerns about your fertility. Early assessment and intervention can maximise your chances of success and provide more treatment options. Remember that fertility is a complex interplay of many factors, and AFC is just one piece of the puzzle.
How the London Pregnancy Clinic Can Help
At the London Pregnancy Clinic, we understand that fertility concerns can be both emotionally and physically challenging. Our experienced team of specialist sonographers and fetal medicine consultants provide comprehensive AFC scanning services using state-of-the-art ultrasound equipment to ensure accurate, reliable results.
Our fertility screening services include detailed AFC assessments performed by specialists who understand the nuances of ovarian reserve testing. We take time to explain your results thoroughly, discussing what they mean for your individual circumstances and potential treatment options. Our compassionate approach ensures you feel supported throughout your fertility journey.
We offer flexible appointment times to accommodate your menstrual cycle timing, ensuring optimal accuracy of your AFC scan. Our detailed reports can be easily shared with your fertility specialist or GP to facilitate seamless care coordination. Additionally, we provide access to genetic counselling services if your results indicate the need for further genetic assessment or family planning guidance.
Whether you’re just beginning to explore your fertility potential or seeking a second opinion on previous results, our clinic provides a comfortable, professional environment where you can receive expert care. We’re committed to delivering accurate, timely results that help inform your reproductive health decisions with confidence and clarity.
Final Thoughts
An AFC scan represents a valuable tool in modern fertility assessment, providing crucial insights into your ovarian reserve and helping guide treatment decisions. Whilst the results can feel overwhelming, remember that AFC is just one factor in your fertility journey, and many women with varying AFCs go on to achieve successful pregnancies.
Understanding your antral follicle count empowers you to make informed decisions about your reproductive health and family planning timeline. Whether your results indicate low, normal, or high ovarian reserve, working with experienced specialists ensures you receive personalised care tailored to your unique circumstances.
If you’re considering fertility assessment or have concerns about your reproductive health, don’t hesitate to seek professional guidance. Early evaluation can provide peace of mind and ensure you have all the information needed to make the best decisions for your future. Contact the London Pregnancy Clinic today to discuss your fertility screening options and take the first step towards understanding your reproductive potential.
Sources
- Antral follice counts (AFC) predict ovarian response and pregnancy outcomes in oocyte donation cycles – PMC
- Ovarian Reserve Testing: Range, Purpose & Results
- AFC (Antral Follicle Count) Ultrasound | Spital Clinic London
- AFC scan | TFP Fertility UK
- Antral follicle count: What is it? | Access Fertility
- What exactly is antral follicle count (AFC)?
- Antral follicle count | Radiology Reference Article | Radiopaedia.org
- What is Antral Follicle Count (& Why it Matters for Egg Freezing)
- Antral Follicle Count Testing Explained: How Clinics Measure AFC | Seen Fertility
- Fertility Testing 101: What Is An Antral Follicle Count (AFC) And Should You Get One?
- Antral Follicle Count (AFC): Normal Count & How To Increase
- Antral Follicle Count – Somerset Early Scans
Latest Stories
HyCoSy vs HSG: Which Fallopian Tube Test Is Right for You

HyCoSy vs HSG: Which Fallopian Tube Test Is Right for You
Published
Tags
Fertility investigations affect approximately 1 in 7 couples in the UK, and understanding which fallopian tube test is most suitable for your circumstances can be crucial for your journey towards conception. Two primary diagnostic procedures, HyCoSy and HSG, offer different approaches to assessing fallopian tube patency and uterine health, each with distinct advantages and considerations that may influence your choice.
Understanding Fallopian Tube Testing
Fallopian tube testing forms an essential component of fertility assessment, helping clinicians identify potential blockages or abnormalities that may prevent conception. These diagnostic procedures evaluate whether eggs can travel freely from the ovaries through the fallopian tubes to reach the uterus, where fertilisation and implantation occur.
The two most commonly used non-surgical methods are HyCoSy (Hysterosalpingo-Contrast Sonography) and HSG (Hysterosalpingography). Both procedures involve introducing contrast medium into the reproductive system to visualise the internal structures, but they utilise different imaging technologies to achieve this assessment.
According to NHS guidelines, tubal factor infertility accounts for approximately 25-35% of female fertility issues, making accurate assessment of fallopian tube function vital for developing appropriate treatment plans.
What is HyCoSy
HyCoSy, or Hysterosalpingo-Contrast Sonography, represents a modern ultrasound-based approach to fallopian tube assessment. During this procedure, a specialised contrast medium is introduced through the cervix into the uterine cavity whilst real-time ultrasound monitoring captures detailed images of the reproductive organs.
The HyCoSy procedure utilises high-frequency sound waves to create detailed visualisations of both the uterine cavity and fallopian tubes. The contrast medium appears bright white on the ultrasound screen, allowing clinicians to observe its flow through the reproductive system and identify any areas of blockage or abnormal anatomy.
This technique offers the advantage of being radiation-free, making it particularly suitable for women who prefer to avoid X-ray exposure or who may require repeated assessments during their fertility journey.
What is HSG
HSG, or Hysterosalpingography, represents the traditional gold standard for fallopian tube assessment, utilising X-ray technology to visualise the reproductive organs. During this procedure, a radio-opaque contrast dye is introduced into the uterine cavity through the cervix, with X-ray images captured to show the dye’s progression through the fallopian tubes.
The HSG procedure provides excellent image quality and has been extensively studied and validated over decades of clinical use. The X-ray images offer exceptional detail of the uterine cavity shape and can clearly demonstrate whether the fallopian tubes are patent (open) or blocked.
HSG has traditionally been considered the first-line investigation for tubal patency assessment in many fertility clinics, with extensive research supporting its accuracy and reliability in diagnosing various reproductive conditions.
Key Differences Between HyCoSy and HSG
Understanding the fundamental differences between these two procedures can help you make an informed decision about which test may be most appropriate for your circumstances:
- Imaging Technology: HyCoSy uses ultrasound waves whilst HSG employs X-ray radiation to create images of the reproductive organs.
- Radiation Exposure: HyCoSy involves no radiation exposure, whereas HSG uses a controlled amount of ionising radiation.
- Real-time Monitoring: HyCoSy provides real-time visualisation during the procedure, allowing immediate assessment of contrast flow.
- Contrast Medium: HyCoSy uses specialised ultrasound contrast agents, whilst HSG employs radio-opaque dye visible on X-ray.
- Procedure Duration: Both procedures typically take 15-30 minutes, though HyCoSy may be slightly quicker due to real-time imaging capabilities.
- Equipment Requirements: HyCoSy requires specialised ultrasound equipment, whilst HSG needs X-ray facilities and fluoroscopy capabilities.
Research indicates that both procedures demonstrate comparable accuracy in detecting tubal blockages, with studies showing similar sensitivity and specificity rates for identifying fallopian tube abnormalities.
Advantages of HyCoSy
HyCoSy offers several compelling advantages that make it an attractive option for many women undergoing fertility assessment:
- No Radiation Exposure: The absence of ionising radiation makes HyCoSy suitable for women who wish to avoid X-ray exposure or require multiple assessments.
- Real-time Assessment: Immediate visualisation allows clinicians to observe contrast flow dynamics and make instant assessments during the procedure.
- Comfortable Environment: The procedure can be performed in a standard ultrasound room rather than requiring specialised X-ray facilities.
- Detailed Ovarian Assessment: Ultrasound technology allows simultaneous evaluation of ovarian morphology and other pelvic structures.
- Reduced Contrast Requirements: Often requires smaller volumes of contrast medium compared to HSG procedures.
- Immediate Discussion: Results can be discussed immediately after the procedure, reducing anxiety and waiting times.
Clinical studies have demonstrated that HyCoSy provides excellent visualisation of uterine cavity abnormalities and can effectively identify both proximal and distal tubal blockages with high accuracy rates.
Advantages of HSG
Despite being the more traditional approach, HSG continues to offer distinct advantages in certain clinical situations:
- Established Gold Standard: Decades of clinical use and extensive research validation support HSG’s reliability and accuracy.
- Superior Image Quality: X-ray technology often provides exceptional detail of uterine cavity shape and tubal anatomy.
- Widely Available: HSG facilities are commonly available in most hospitals and fertility centres across the UK.
- Detailed Documentation: X-ray images provide permanent, high-quality records for future reference and specialist consultations.
- Cost-Effective: HSG may be slightly more cost-effective in some healthcare settings due to established protocols and equipment.
- Therapeutic Benefits: Some studies suggest that HSG may have mild therapeutic effects, potentially improving conception rates in certain cases.
The RCOG recognises HSG as an effective method for assessing tubal patency, with guidelines supporting its use as part of comprehensive fertility investigations when clinically appropriate.
Potential Disadvantages and Considerations
Both procedures have specific limitations and considerations that may influence your decision:
HyCoSy Considerations:
- Operator Dependency: Results may vary depending on the sonographer’s experience and expertise with the technique.
- Image Quality Limitations: Ultrasound images may be affected by patient factors such as body habitus or bowel gas.
- Specialised Equipment: Requires specific ultrasound contrast agents and experienced personnel trained in the technique.
- Limited Availability: May not be available in all healthcare facilities compared to traditional HSG.
HSG Considerations:
- Radiation Exposure: Involves controlled X-ray exposure, which some women prefer to avoid.
- Contrast Reactions: Rare but possible allergic reactions to iodine-based contrast media.
- Facility Requirements: Requires access to specialised X-ray equipment and trained radiological staff.
- Static Images: Provides snapshot images rather than real-time dynamic assessment of contrast flow.
Procedure Experience and Comfort
Understanding what to expect during each procedure can help you prepare mentally and physically for the assessment:
HyCoSy Experience: The procedure takes place in a comfortable ultrasound room, similar to routine pregnancy scans. You’ll lie on an examination couch whilst a transvaginal ultrasound probe and small catheter are used to introduce contrast and monitor its flow. Most women describe the experience as similar to a smear test with mild cramping during contrast injection.
HSG Experience: The procedure occurs in an X-ray department, where you’ll lie on an examination table beneath X-ray equipment. A speculum is used to visualise the cervix, and contrast dye is introduced through a small catheter. The experience may involve slightly more intense cramping, particularly when the contrast fills the fallopian tubes.
Both procedures are typically performed without anaesthesia, though some clinics may offer pain relief options. Most women can return to normal activities immediately after either procedure, though mild cramping or light spotting may occur for 24-48 hours.
Accuracy and Clinical Outcomes
Research comparing HyCoSy and HSG demonstrates that both procedures offer comparable accuracy in detecting tubal abnormalities. Clinical studies indicate sensitivity rates of approximately 85-95% for both techniques in identifying blocked fallopian tubes, with specificity rates similarly high.
A systematic review published in fertility journals found no significant difference between HyCoSy and HSG in terms of diagnostic accuracy for tubal patency assessment. Both procedures effectively identify:
- Tubal Blockages: Complete or partial obstruction of one or both fallopian tubes.
- Uterine Abnormalities: Structural anomalies affecting the uterine cavity shape or size.
- Hydrosalpinx: Fluid accumulation within blocked fallopian tubes.
- Adhesions: Scar tissue affecting tubal function or mobility.
The choice between procedures often depends on individual circumstances, patient preferences, and clinical considerations rather than significant differences in diagnostic accuracy.
Timing and Preparation
Both HyCoSy and HSG require careful timing and preparation to ensure optimal results and patient safety:
Optimal Timing: Both procedures should be performed in the first half of your menstrual cycle, typically between days 7-12, to avoid potential early pregnancy and ensure the endometrium is appropriately thin for clear visualisation.
Pre-procedure Preparation:
- Contraception: Reliable contraception should be used from the start of your cycle until the procedure to prevent pregnancy.
- Infection Screening: Some clinics may require screening for sexually transmitted infections before the procedure.
- Pain Management: Taking ibuprofen 1-2 hours before the procedure may help reduce discomfort.
- Medical History: Inform your clinician about any allergies, particularly to contrast media or medications.
Your healthcare provider will provide specific preparation instructions tailored to your individual circumstances and the chosen procedure.
Cost Considerations and NHS Availability
The availability and cost of HyCoSy versus HSG can vary significantly depending on whether you choose NHS or private healthcare pathways:
NHS Provision: Both procedures may be available through NHS fertility services, though availability varies by region and local commissioning decisions. HSG tends to be more widely available across NHS trusts, whilst HyCoSy availability may be limited to specialist centres.
Private Healthcare: Private fertility clinics typically offer both options, with costs varying depending on location and clinic facilities. HSG may be slightly less expensive in some settings due to established protocols and wider availability of equipment.
When considering costs, factor in potential follow-up appointments, additional imaging requirements, and the overall fertility assessment pathway rather than just the individual procedure cost.
Making Your Decision
Choosing between HyCoSy and HSG involves considering multiple factors specific to your individual circumstances:
- Radiation Sensitivity: If you have concerns about radiation exposure or require multiple assessments, HyCoSy may be preferable.
- Previous Procedures: Your experience with ultrasound scans versus X-ray procedures may influence your comfort level.
- Clinical Complexity: Your clinician may recommend one procedure over another based on your specific medical history.
- Availability and Timing: Local availability of equipment and expertise may influence your options.
- Personal Preferences: Your comfort with different types of medical procedures and imaging technologies.
Discussing these factors with your healthcare provider will help determine which procedure aligns best with your individual needs and circumstances. Both procedures provide valuable diagnostic information to guide your fertility treatment journey.
How the London Pregnancy Clinic Can Help
At the London Pregnancy Clinic, we offer comprehensive HyCoSy scanning services performed by experienced sonographers using state-of-the-art ultrasound equipment. Our team understands the emotional and physical aspects of fertility investigations and provides compassionate, professional care throughout your assessment.
Our HyCoSy procedures are conducted in comfortable, private facilities with immediate results discussion and detailed reporting for your healthcare providers. We work closely with fertility specialists and can provide comprehensive imaging assessments as part of your broader fertility investigation pathway.
For women requiring additional screening or genetic counselling as part of their fertility journey, we also offer carrier screening tests and genetic counselling services to provide comprehensive reproductive health assessments.
Final Thoughts
Both HyCoSy and HSG represent valuable diagnostic tools in fertility assessment, each offering distinct advantages depending on your individual circumstances. The choice between these procedures should be based on careful consideration of your medical history, personal preferences, and clinical recommendations from your healthcare team.
Remember that these investigations form just one component of comprehensive fertility assessment, and the results will help guide your treatment options and reproductive health decisions. Whether you choose HyCoSy or HSG, both procedures provide crucial information about fallopian tube function and uterine health.
If you’re considering fallopian tube assessment as part of your fertility journey, our experienced team at the London Pregnancy Clinic is here to provide expert care and support. Contact us today to discuss your options and book a consultation to determine the most appropriate diagnostic pathway for your individual needs.
Sources
-
- Hysterosalpingography (HSG) – Leeds Teaching Hospitals NHS Trust
- Hystero Contrast Sonography (HyCoSy) test – Buckinghamshire Healthcare NHS Trust
- Imaging department Booking your hysterosalpingogram (HSG)
- Tubal Patency Testing (HSG/HyCoSy) Eligibility (690) | Right Decisions
- Leeds Centre for Women’s Health Hysterosalpingography (HSG)
- Hysterosalpingo Contrast Sonography (HyCoSy) – Leeds Teaching Hospitals NHS Trust
- HSG (Hysterosalpingography) — Chelsea and Westminster Hospital NHS Foundation Trust