Innovations in Pregnancy Care

Innovations in Pregnancy Care
An evening dedicated to LPC’s commitment towards “Innovative Pregnancy Care”
Published
Tags
London Pregnancy Clinic’s recent “Innovative Pregnancy Care” event was a confluence of expertise and insight, shaping the future of prenatal care. Leading professionals gathered to discuss breakthroughs in early diagnostics and patient education, emphasising LPC’s forward-thinking approach.
A December evening at Spitalfields Market was transformed into a hub of medical expertise during the London Pregnancy Clinic’s event. The focus was on pioneering approaches in prenatal care, particularly the 10 Week Scan, Non-invasive prenatal testing (NIPT), and pre-eclampsia diagnosis.
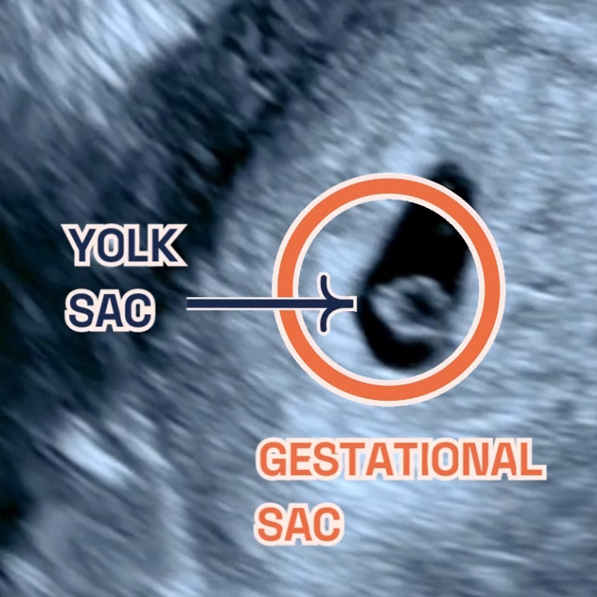
Advancing the 10 Week Scan
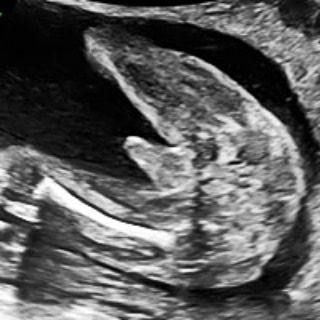
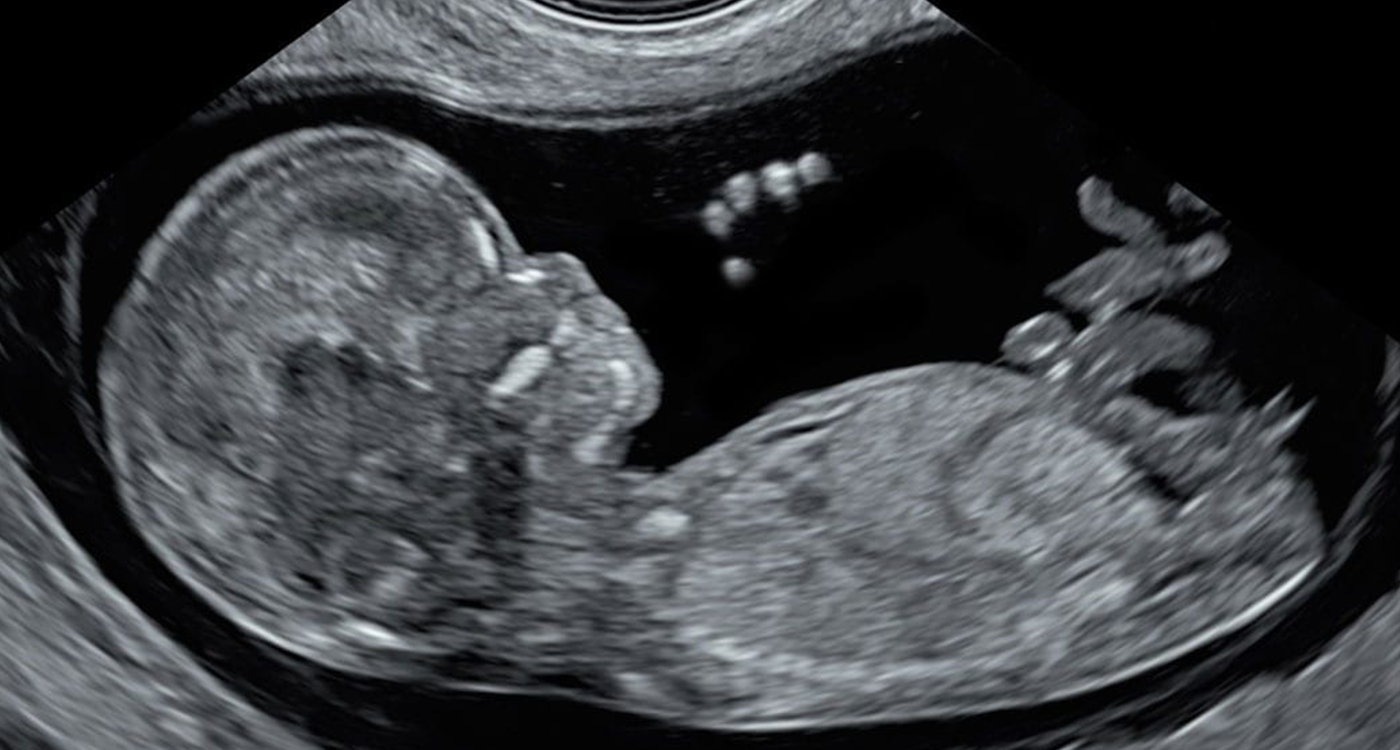
The evening began with Ms. Shaz Khojasteh, LPC’s clinical lead, greeting each attendee with a warmth that matched her expertise. Her introduction was not just an opening speech but a heartfelt welcome to LPC’s family. She shared with the audience our signature 10 Week Scan, which isn’t just a routine check. It’s a comprehensive examination of the baby’s anatomy, providing vital developmental insights at a crucial early stage, thereby enriching the information gathered before conducting NIPT.
Demystifying NIPT – Dr Fred Ushakov’s Perspective
The spotlight then shifted to Dr. Fred Ushakov, whose speech was not only insightful but also visionary. He spoke passionately about his mission, in collaboration with the London School of Ultrasound and UCLH, to train the next generation of doctors and sonographers. His goal is to equip them with the skills and knowledge necessary to leverage early pregnancy scans to their full potential, enhancing patient care and pregnancy outcomes. This mission, he explained, is vital in ensuring that every pregnancy is approached with the utmost care and precision.
Dr Ushakov then addressed a common misunderstanding about NIPT. He emphasised that while NIPT is effective, it’s not all-encompassing. Patients may misinterpret it as a guarantee against all prenatal issues, not realising that conditions more severe than Down’s syndrome can occur and cannot be detected by NIPT. He further highlighted the importance of the dual approach (watch the explainer video here) that he instilled at LPC. Dr. Ushakov’s call for broader education and comprehensive scanning techniques underscored the need for a more informed approach to prenatal care.
Advocacy for Pre-eclampsia Awareness
Next, we were captivated by Dr. Daniel Stott, whose talk about pre-eclampsia was as enlightening as it was heartfelt. It was clear from his words and the energy in his voice just how dedicated he is to this topic. Dr. Stott walked us through the workings of a groundbreaking blood test for pre-eclampsia. With an approachable manner, he explained how this test isn’t just for identifying pre-eclampsia; it’s a crucial tool in carefully guiding expectant mothers through the rest of their pregnancy.
Conclusion
As the expert talks wrapped up, the event naturally transitioned into festive networking. It was a perfect opportunity for attendees to connect, exchange experiences, and build professional ties in a holiday atmosphere. The evening emerged as a crucible of innovative ideas and shared goals for advancing prenatal care. Leaving the market, we carried with us the night’s insights and a renewed hope for the future of prenatal health. The event proved to be not just a confluence of minds but a beacon of hope for prenatal care’s future.
A special thank you to our sponsors Eurofins.