Week 10 of Pregnancy
Week 10 of your Pregnancy
Discovering your baby’s progress since week 10
-
Published
-
Last Modified
Tags
At 10 weeks, your pregnancy reaches a significant stage of development. Your baby has now officially transitioned from an embryo to a fetus, and their growth is accelerating. With each passing day, vital organs mature, facial features become more defined, and tiny fingers and toes take shape. Though still small, about the size of a prune, your baby is now moving more actively inside the womb.
For many expectant parents, this is an ideal time to book a private early pregnancy scan. At London Pregnancy Clinic, we provide high-resolution ultrasound imaging to track your baby’s progress, offering reassurance and detailed insights. This is also the earliest point for non-invasive prenatal testing (NIPT), which can screen for chromosomal conditions and determine the baby’s sex.
Pregnancy Checklist at 9 Weeks
- Book and attend your private early pregnancy scan: Capturing clear images during the 6-9 week Viability Scan is crucial for assessing your baby’s development and health. These dating Scans are pivotal, offering crystal-clear imagery that plays a crucial role in monitoring your baby’s development and ensuring their health. Beyond the clinical benefits, these scans foster a profound emotional bond, providing expectant parents with a reassuring glimpse into their baby’s growth and vitality.
- Prioritise Health and Well-being: Your health directly impacts your baby’s growth. Eat well, stay active with gentle exercise, and heed your healthcare provider’s advice.
- Communication with healthcare professionals: Regular communication with medical professionals is crucial. They offer invaluable support and guidance through physical and hormonal changes. Trust them to make your pregnancy journey informed and smooth.
- Book Your Antenatal Appointment: If you’ve not yet booked your first antenatal appointment, now’s the time. The NHS offers thorough antenatal care, starting with this vital step. Alternatively, London Pregnancy Clinic’s early private midwifery services offer customised care, tailored to your pregnancy. Use this appointment to voice queries and concerns, laying the groundwork for a healthy pregnancy.
- Non-Invasive Prenatal Testing (NIPT): Consider NIPT, a screening that analyses the baby’s genetic information through a simple blood test from the mother. Mostly available from as early as 10 weeks, NIPT can detect certain genetic conditions and determine the baby’s sex. It’s a non-invasive way to gain early insights into your baby’s health and development. Discuss the option of NIPT with your healthcare provider to understand its benefits and whether it’s right for you. If you want to do the earliest possible NIPT we offer Panorama NIPT which can be done from week 9.
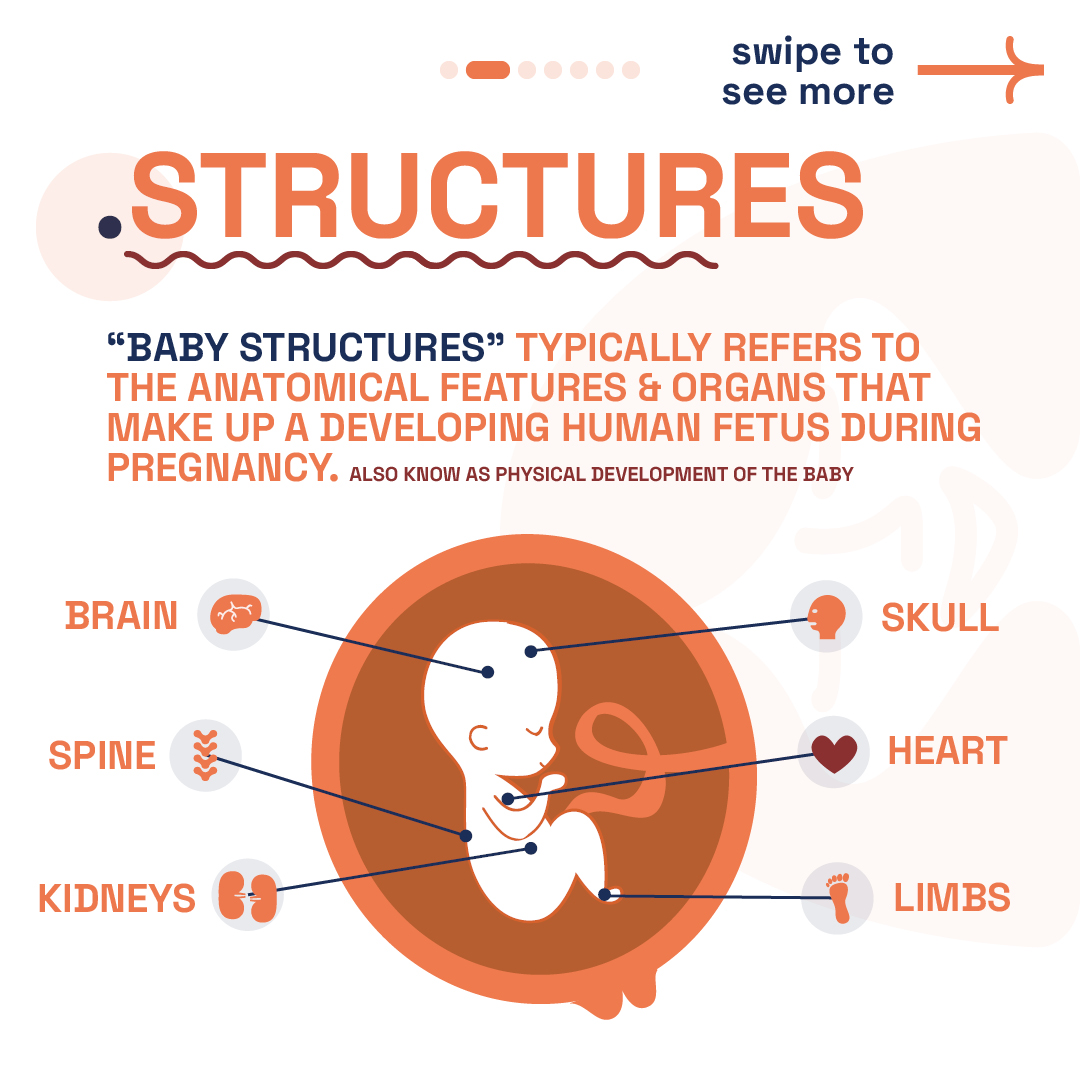
Developmental Milestones: Week 9
Embryonic Growth: At this stage, your baby measures between 23 to 31 mm from crown to rump (CRL), which is around the size of an olive. The embryonic shape evolves, with fingers and toes becoming more defined, moving away from their initial webbed appearance.
Gestational and Yolk Sac aDevelopment: According to Nature, By week 9, the gestational sac typically measures between 35-40 mm, with the yolk sac around 3.6 mm.
Heart Development: The fetal heart rate continues to slightly increase to an average of 140-170 beats per minute (BPM) and will gradually stabilise around 12 weeks. These statistics vary from person to person that’s why the range is so large.
Brain + Neural Development: By week 9, the neural tube closes, a vital step in the baby’s brain and spinal cord development. This lays the groundwork for the central nervous system. The brain’s rapid growth sees specific areas forming, enhancing its structure and complexity. Electrical activity starts by week 6, with significant development continuing into the first trimester.
Other Development: Your baby’s facial features, like closed eyes, mouth, tongue with taste buds, and ear lobes, are shaping up. The liver starts making blood cells, and blood vessels form under the skin. The genital tubercle, visible in all embryos, indicates a key point in gender development, observable in both 2D and 3D ultrasounds.
Umbilical cord: In week 9 of pregnancy, the umbilical cord becomes the baby’s vital connection to the placenta. It comprises one vein and two arteries, twined together, that transport crucial nutrients and oxygen to support the baby’s growth. The umbilical cord’s formation starts around week 3 from a connecting stalk, evolving into the mature cord by week 7. This structure, with its gelatinous coating, ensures the efficient exchange between mother and baby.
What is seen on the Ultrasound: Week 9?
As you enter week 9 of your pregnancy journey, an early pregnancy scan offers an enriched, detailed view of your baby’s development, a process both miraculous and fascinating. This period marks a significant milestone in your little one’s growth, as the ultrasound reveals the intricate formation of their tiny body, from the rhythm of the heartbeat to the delicate shaping of limbs and facial features. Perhaps most heartwarming is the possibility of observing movements, especially in the torso, as your baby starts to stretch and wriggle.
A week prior, black spots within your baby’s head signalled the initial stages of brain development. Now, these spaces are filled by the choroid plexus, visible as white spots on the ultrasound. This transition is vital for the growth of the brain’s primary divisions—forebrain (prosencephalon), midbrain (mesencephalon), and hindbrain (rhombencephalon)—laying the foundation for future cognitive and motor skills, emotions, and memories.
Also captured in the ultrasound is the growth of the placenta, depicted as two white lines framing the gestational sac. This organ is indispensable, serving as the lifeline that supplies essential nutrients and oxygen to your baby via the umbilical cord. Its presence and development are reassuring indicators of the pregnancy’s health and progression.
By week 9, the genital tubercle is visible in all embryos, signifying a key phase in gender development. Visible via 2D or 3D ultrasound, its clarity improves with transvaginal scans. This method provides high-resolution images, offering a clear glimpse of early baby movements. While each pregnancy is unique, ultrasound scans follow a similar process. As time goes on, the genital tubercle evolves into either a penis or a clitoris, marking the baby’s gender.
-
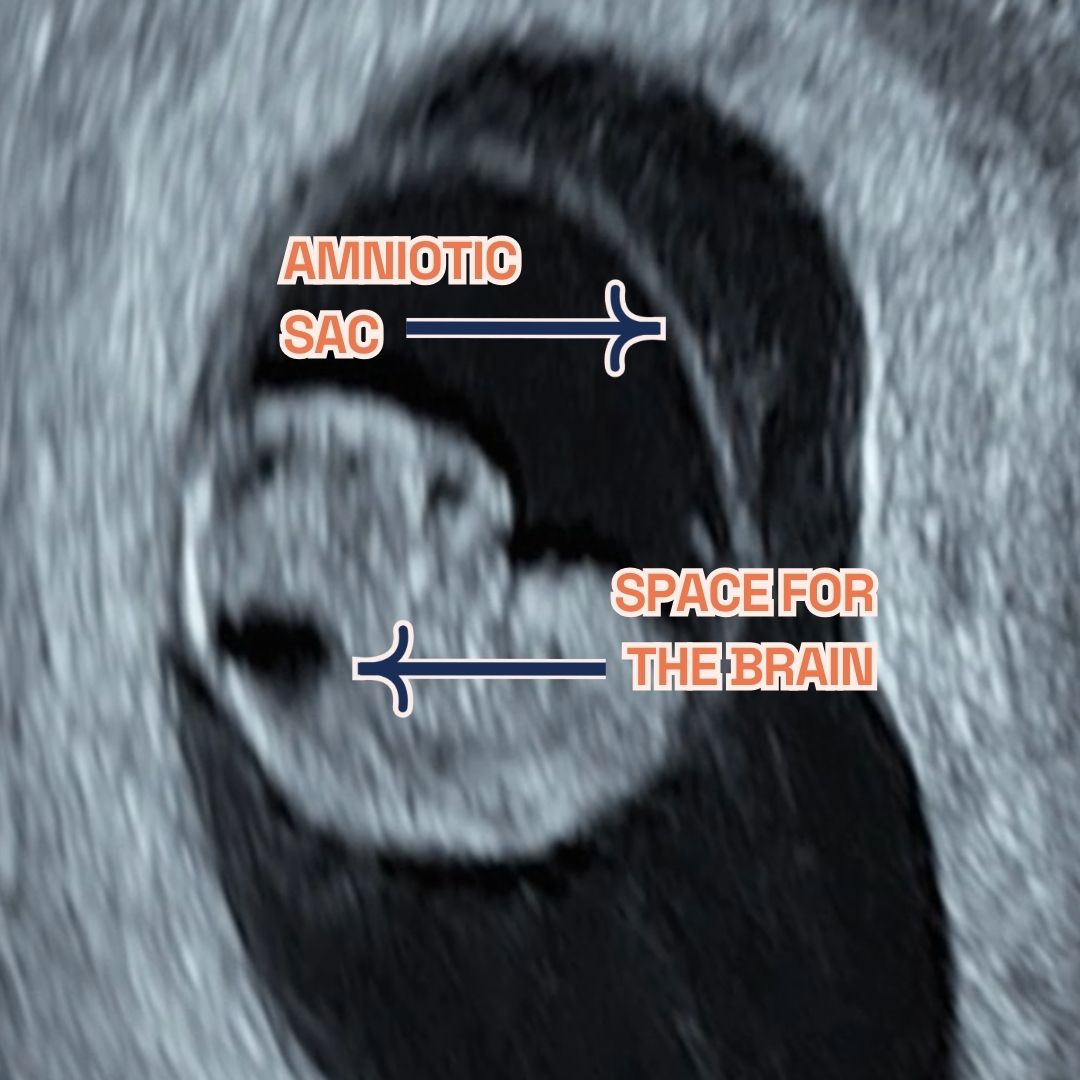
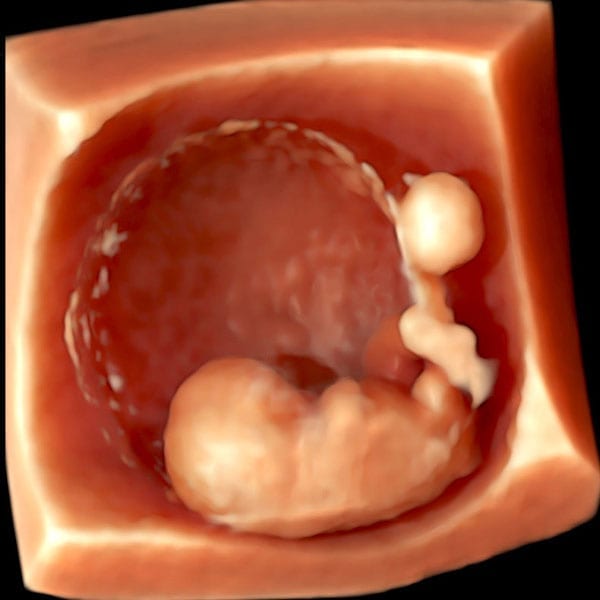
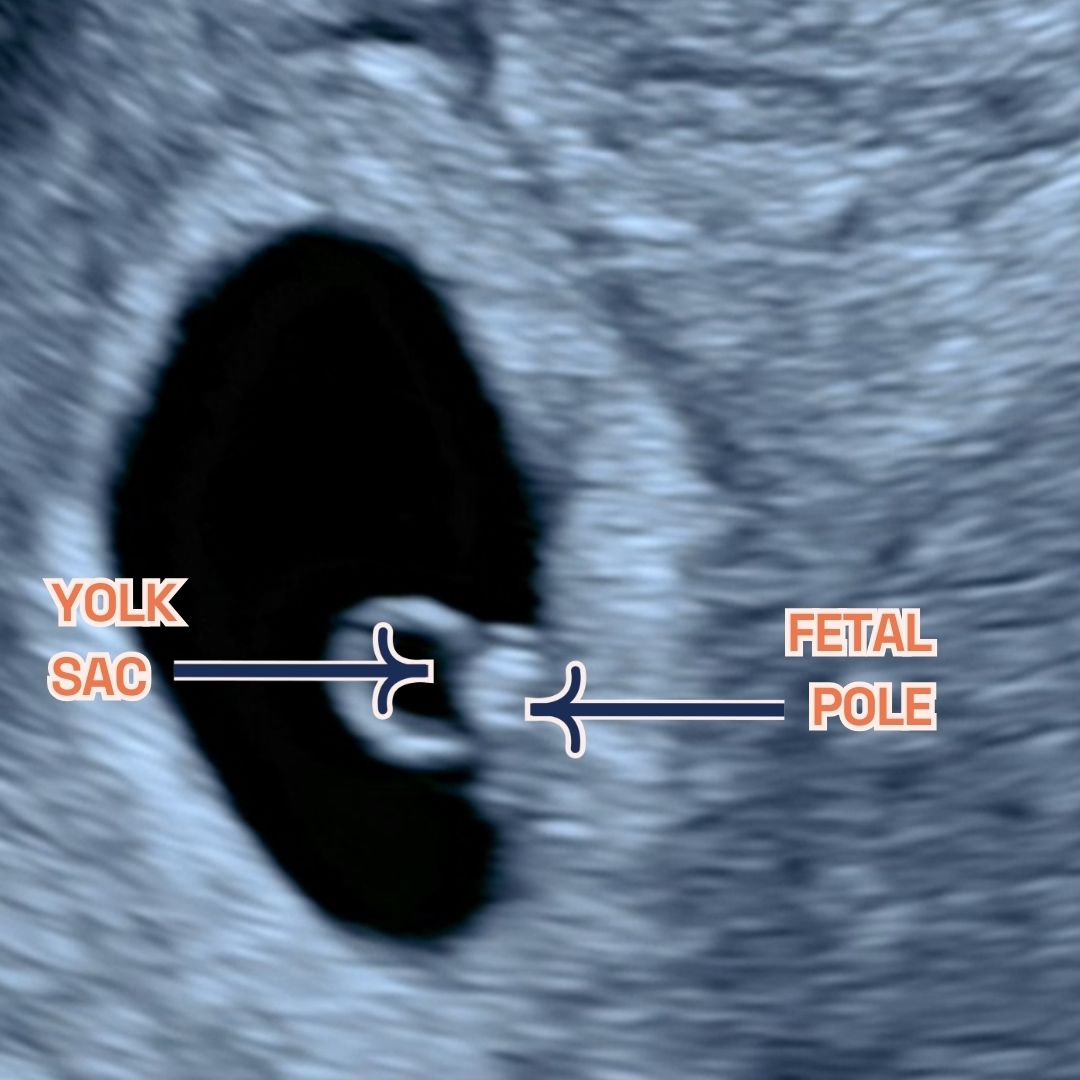
Gestational sac, fetal pole and amniotic sac at 8 weeks of pregnancy as seen on ultrasound scan.
-
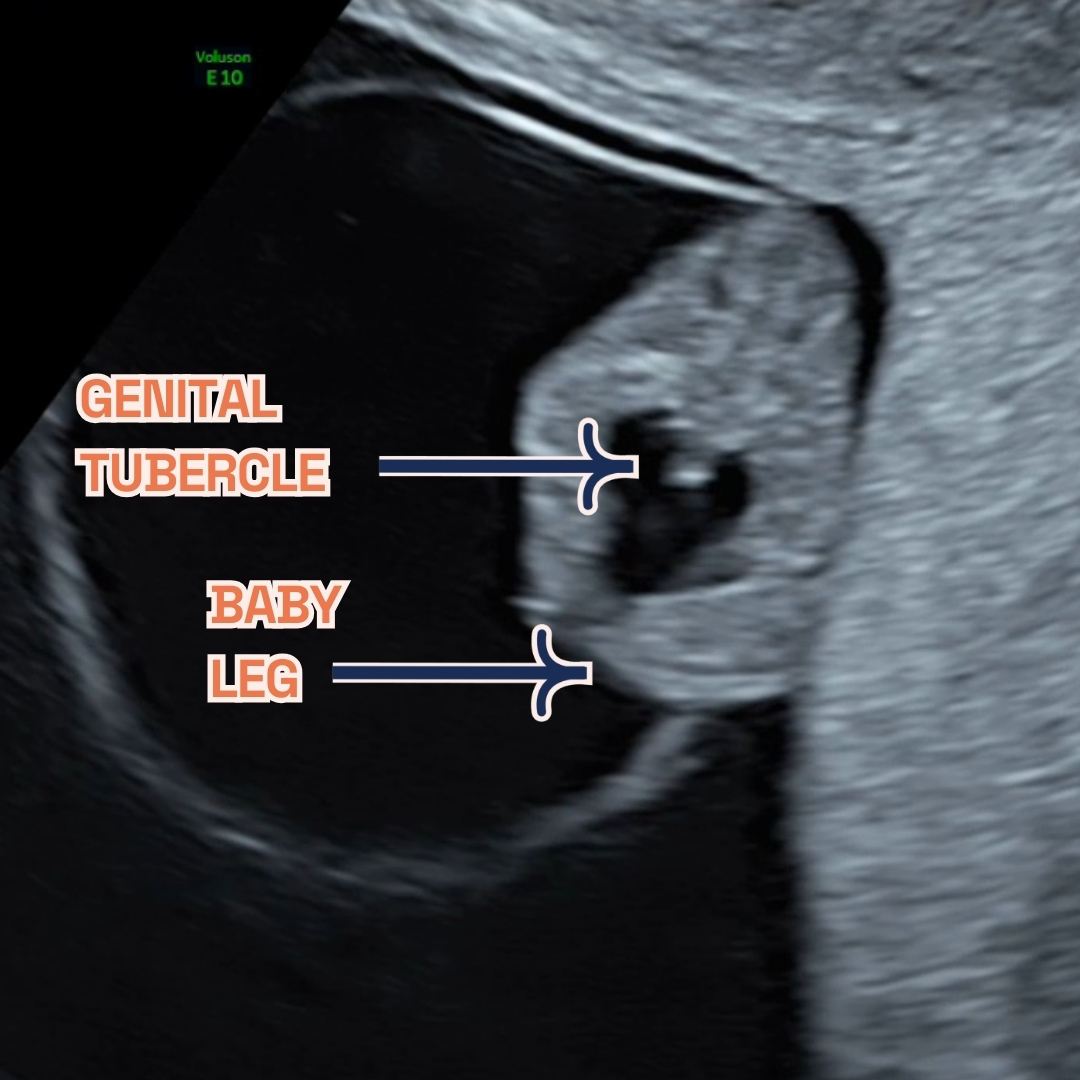
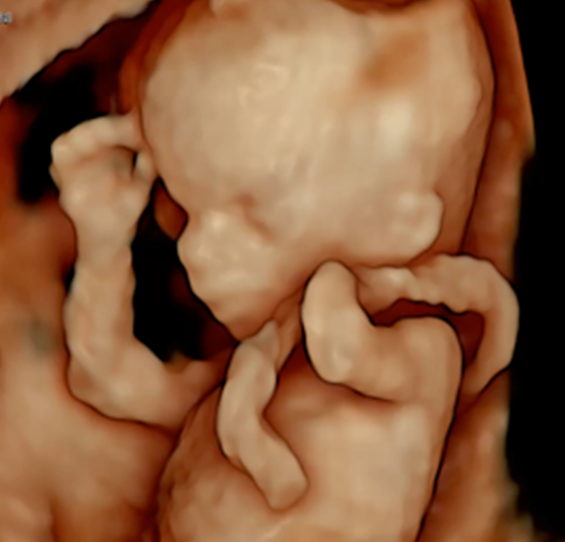
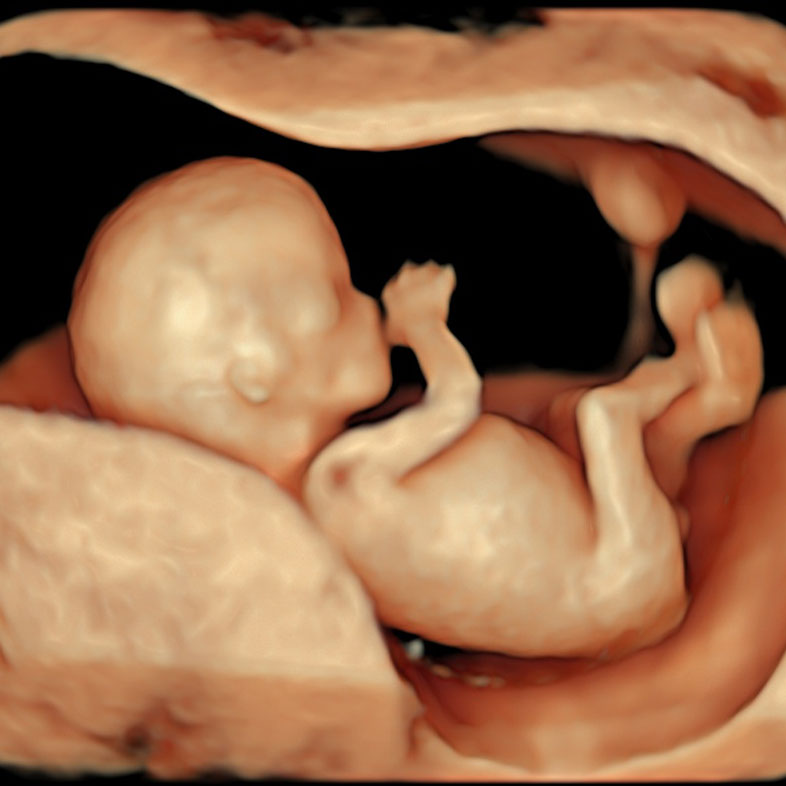
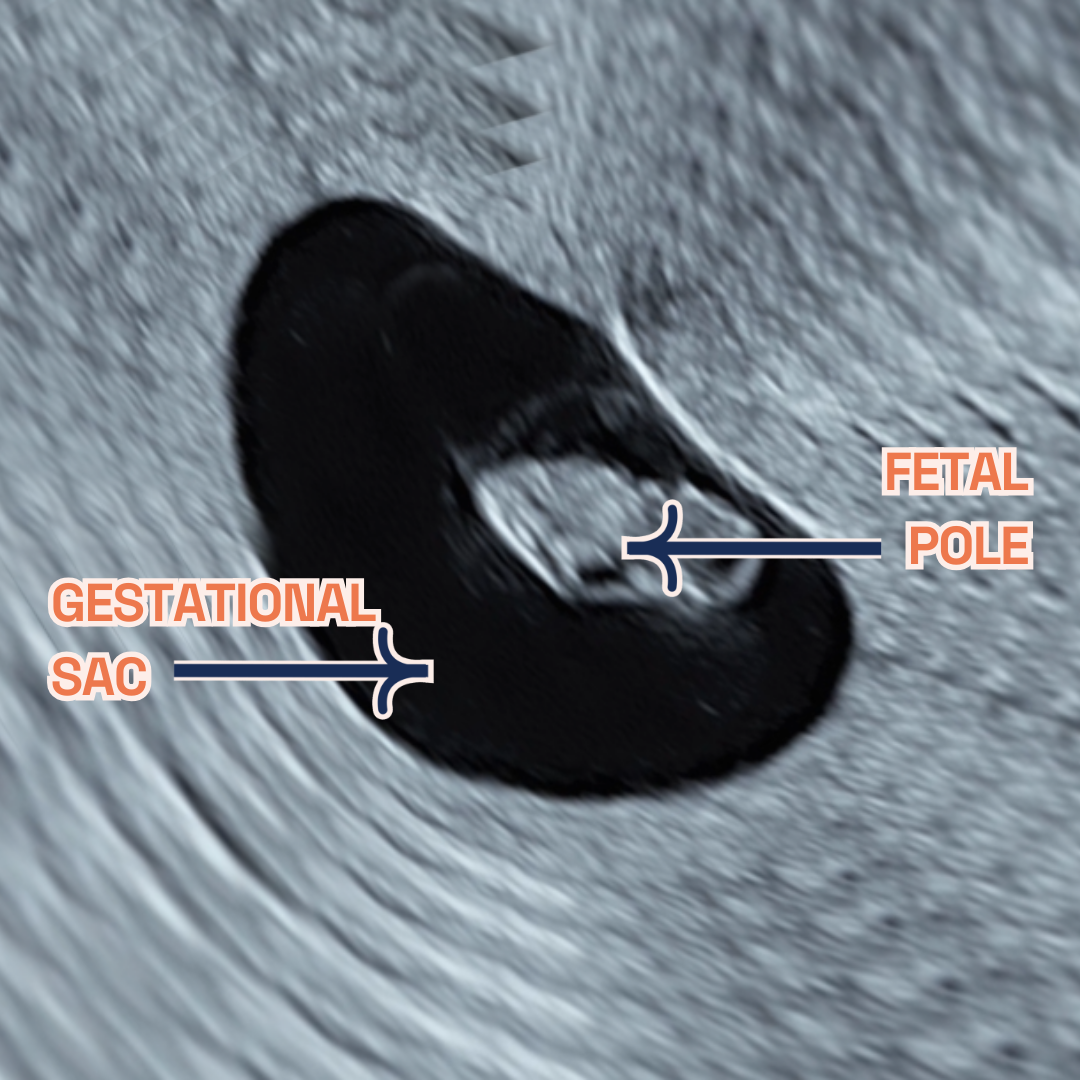
Gestational sac, fetal legs and Genital Tubercle at 9 weeks of pregnancy as seen on ultrasound scan.
Thinking ahead: Week 10?
Around 10 weeks into pregnancy, some women might had their initial ultrasound scan already. This scan helps confirm the due date by measuring the baby’s size and checks for multiple births or genetic conditions like Down’s syndrome risk. It’s crucial to keep regular prenatal check-ups and share any concerns with healthcare professionals for proper advice during pregnancy. Discuss the option of a NIPT with your doctor. Available from week 10, this test screens for chromosomal abnormalities and can reveal the baby’s sex.
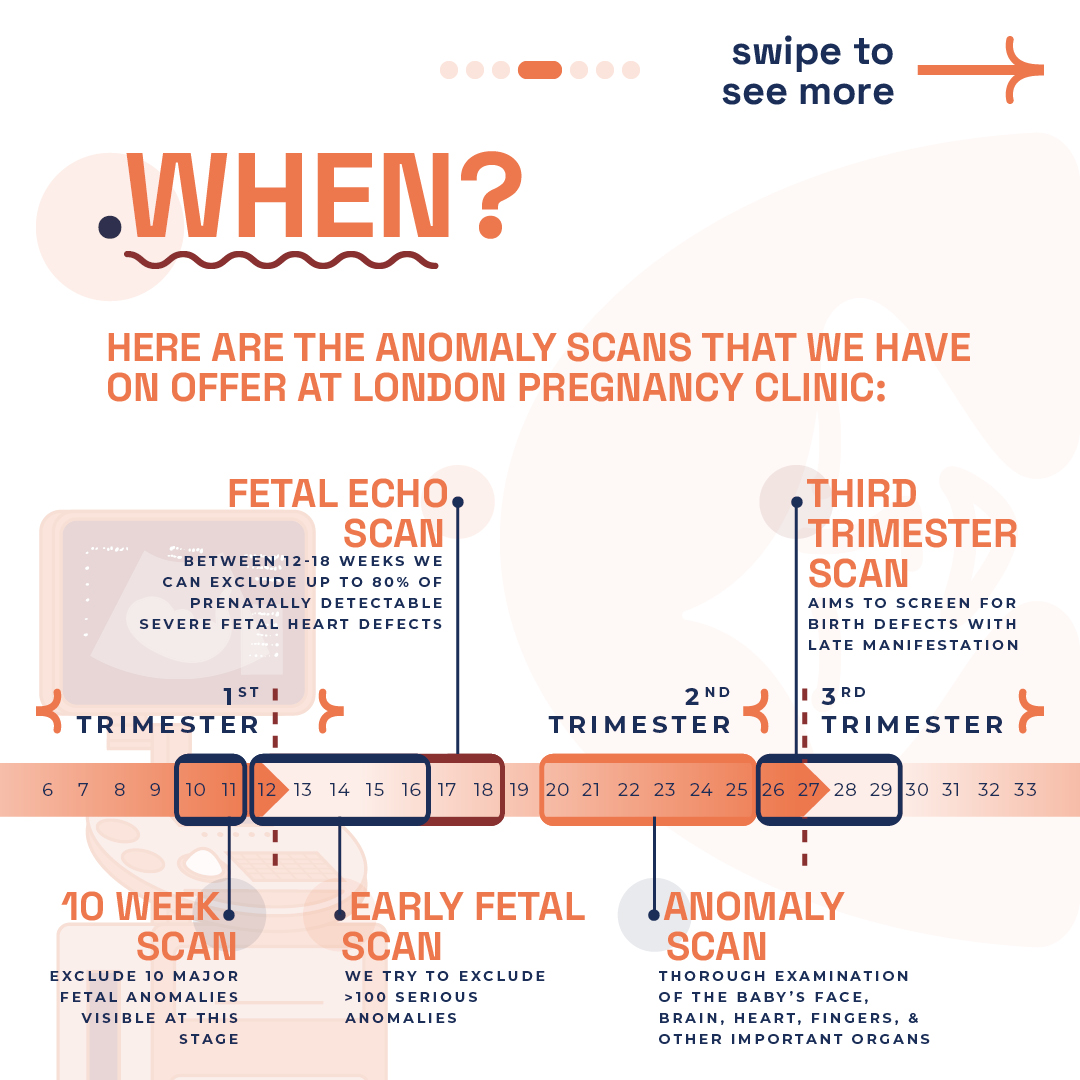
You may be considering our innovative 10 Week Scan, it’s important to note that this is distinct from the usual viability or dating scans you might be familiar with. Specifically designed for 10-11 weeks of pregnancy, this scan acts as the earliest anomaly check, providing parents with early reassurance by screening for significant physical abnormalities. It marks the first opportunity for a structural examination of the baby, at the earliest stage possible. This timing also makes it the optimal period for non-invasive prenatal testing (NIPT), leveraging our blend of professional expertise and the latest in ultrasound technology to deliver results with unmatched clarity. Compared to the standard NHS 12 week scan, our 10-week scan offers a more comprehensive checklist, ensuring nothing is overlooked.
Remember, NIPT indicates the likelihood of certain conditions, unlike amniocentesis or chorionic villus sampling (CVS), which provide definitive results but are invasive. Always check if your insurance covers NIPT. For those over 35 or with a family history of genetic conditions, consider NIPT, CVS (done between 10 and 13 weeks), and amniocentesis (usually between weeks 15 to 20). The likelihood of a baby having a chromosomal condition, such as aneuploidy, rises with maternal age, notably after 35 years, termed “advanced maternal age.”
Week 9: Your body?
Alongside fetal developments, maternal changes may be observed during the ultrasound. Increased blood volume and fluid retention can lead to frequent urination. Hormonal fluctuations may cause symptoms like headaches, low blood pressure, constipation, and fatigue. These changes reflect the body’s adaptation to support the growing fetus during pregnancy.
Keep hydrated by drinking plenty of water, aiming to drink more in the morning to avoid nighttime trips to the loo. At 9 weeks, you might struggle to fasten your jeans as your uterus expands, doubling in size to accommodate your growing baby. You may even start to show a little. As the weeks progress, your uterus will grow beyond your pelvis. Gaining weight now is not just normal—it’s advisable. Your ideal weight gain during pregnancy depends on your pre-pregnancy BMI. Generally, with a normal BMI, you’d be expected to gain 25 to 35 pounds throughout, with one to five pounds in the first trimester.
However, morning sickness and food aversions may lead to weight loss instead of gain at this stage. Discuss any weight concerns, gain or loss, especially if changes are sudden or severe, with your obstetrician or midwife. Minor weight loss is often seen as acceptable early on. As your appetite returns, there’ll be chances to get your weight gain on track. Severe nausea may require medical intervention. Many under-report nausea and vomiting, but numerous safe Over-The-Counter and prescription options can manage symptoms.
Week 9 of Pregnancy FAQs
-
what happens during week 9 of pregnancy?
At 9 weeks pregnant, your body and baby undergo significant changes. Not everyone experiences the same symptoms, ranging from hair thickening—due to reduced shedding and possibly healthier lifestyles including prenatal vitamins—to bloating, caused by increased progesterone slowing digestion.
An early scan reveals your baby’s rapid growth, from forming hands and feet to facial features developing, and even early movements. The scan also shows the brain’s development, the steady heartbeat indicating a strong cardiovascular system, and the placenta’s vital role in providing nutrients. The genital tubercle’s visibility marks the beginning of gender development, becoming clearer with transvaginal scans.
-
spotting during week 9 of pregnancy?
Spotting in week 9 of pregnancy is commonly seen and typically isn’t a cause for concern. Light bleeding or spotting can be normal in the first trimester. Nonetheless, consulting your midwife or healthcare provider for a check-up is always wise to dismiss any potential issues.
Usually, spotting isn’t alarming, but monitoring the situation and getting medical advice if the bleeding gets heavy or continuous is vital. Keeping in contact with your healthcare provider during your pregnancy is crucial to quickly address concerns and safeguard the health of you and your baby.
Every pregnancy is distinct, and although spotting can be standard, consulting your healthcare provider for tailored advice and reassurance is always recommended.
-
why is week 9 of pregnancy the worst?
Week 9 of pregnancy might bring challenges due to physical and hormonal changes. Your breasts may enlarge and your waist could thicken as your uterus grows. High levels of pregnancy hormones may cause discomfort and morning sickness. These symptoms are often temporary and improve by the second trimester. Nausea and vomiting, known as “morning sickness,” can happen any time. This is often due to the rise in human chorionic gonadotropin (hCG), peaking around week 10. So, the most intense nausea might occur between now and next week. Additionally, increased progesterone can make your breasts larger or swollen.
-
Common symptoms during nine weeks pregnant
Feeling early flutters at 8 weeks? Expect:
- Fatigue: Your body is working hard, so tiredness is typical. Make rest a priority.
- Frequent urination: Your expanding uterus presses on the bladder, meaning more loo visits.
- Morning sickness: Nausea and vomiting might strike any time. Keep hydrated and seek relief methods.
- Enhanced senses: You may experience metallic tastes or strong smells. It’s all part of the journey!
- Mood swings: Hormonal changes may affect your emotions. Treat yourself gently.
- Sore breasts: Hormones are prepping for breastfeeding, causing discomfort.
- Bloating and cramping: These are signs of your growing uterus.
- Light spotting: It’s rare but can occur. Contact your doctor if worried.
- Other signs: Thicker hair, skin changes, or milky discharge are normal during pregnancy.
Each pregnancy differs. Some women get many symptoms; others have few. Always consult your healthcare provider with concerns. Consider a private midwife consultation for worries.
-
Can I do NIPT at 9 weeks of pregnancy?
Non-invasive prenatal testing (NIPT)
can start at 9 weeks into pregnancy. It’s a safe, accurate way to screen for chromosomal abnormalities like Down’s, Edwards’, and Patau’s syndromes. By analysing the mother’s blood for cell-free DNA, NIPT gauges the fetus’s risk for specific genetic conditions without miscarriage risks, ensuring early detection and reassurance. We advise waiting until week 10 for NIPT, allowing it to coincide with our 10-week scan for optimal results.
NIPT stands out for its precise detection of chromosomal disorders, showing high sensitivity for conditions such as Down’s syndrome. Early testing allows for informed decisions and tailored prenatal care. Discussing NIPT with your healthcare provider is crucial to see if it suits your needs and to understand test implications.
Benefits of NIPT include:
- Non-invasive with no risk to the baby.
- High accuracy for peace of mind.
- Early detection for proactive decision-making.
- Optional sex determination for early family planning.
Remember: NIPT is a screening test, not a definitive diagnosis. Consult your healthcare provider for further information and personalised guidance. We at LPC offer multiple NIPTs (PrenatalSafe, Panorama, Unity, SMART TEST, Illumina,
Harmony) and out specialists will help you choose the best option for you!
Final Thoughts
Week 9 is a time of remarkable progress, and London Pregnancy Clinic is here to guide and support you through every step. With each visit, you’ll gain deeper insights into your baby’s development, reinforcing the bond you share. Embrace this journey with confidence, knowing we’re by your side.
Stay informed and excited about what each new week will reveal about your baby’s growth on our blog.