Happy Holidays for 2023!

Happy Holidays for 2023!
Our warmest wishes to those pregnant during the holidays!
Published
Tags
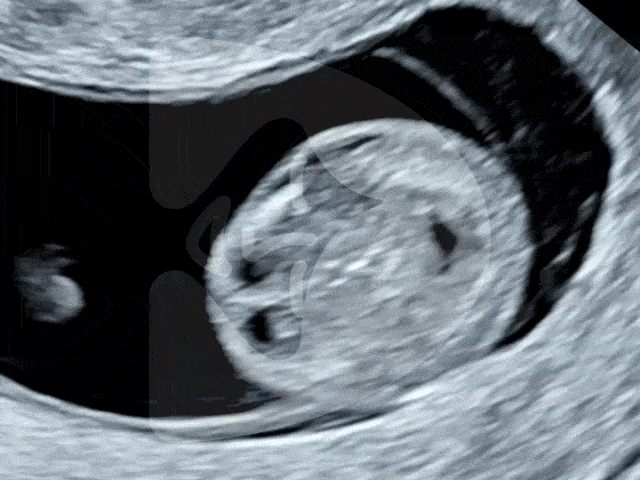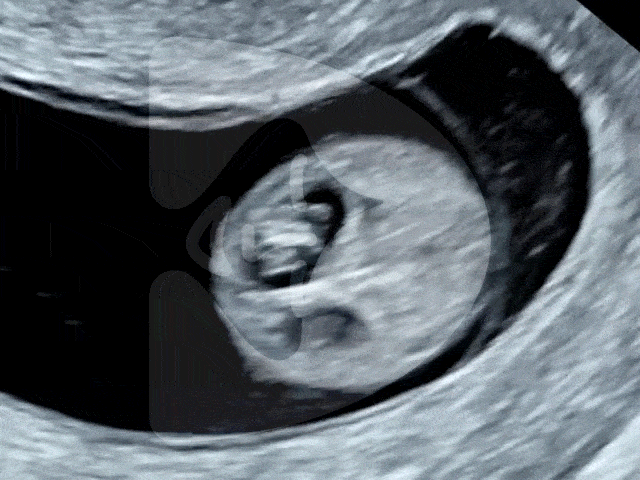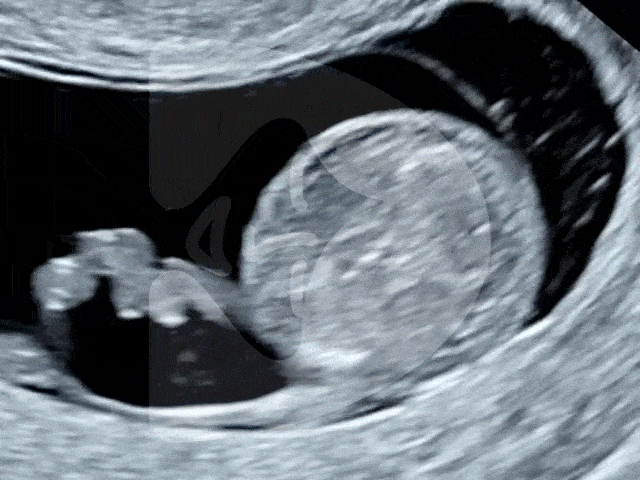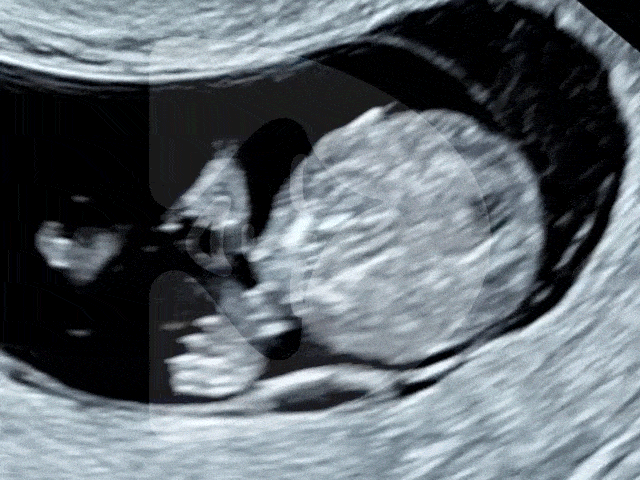
As the year draws to a close, London Pregnancy Clinic extends the warmest holiday greetings to all. Join us in reflecting on the year past and looking forward to a new beginning, filled with hope and health. Discover the warmth of being pregnant during the holidays and look ahead to a New Year brimming with health, happiness, and vital early pregnancy scans.
Ho Ho Ho! As the holiday season wraps us in a big, cheerful hug, we at London Pregnancy Clinic are bubbling with excitement to spread some festive cheer and a sprinkle of spectacular news! It’s time to jingle all the way into the holidays with heartfelt wishes and exciting updates.
Double the Joy, Double the Care
2023 has been a remarkable year for us – we’ve grown from a cozy team to a bustling family of 8 clinicians! That’s right, we’ve doubled our capacity, all thanks to the trust and support from wonderful people like you. This growth means more laughter, more stories, and most importantly, more expert hands to ensure you receive the best care on your pregnancy journey.
The London Pregnancy Clinic team embraced festive creativity by designing a unique LEGO Group Ultrasound Set, introducing a maternity care theme to the LEGO City world. This charming set features a pregnant mini-figure, a doctor, and a nurse, celebrating the journey of motherhood and the care surrounding expectant mothers. While not an official LEGO product, it’s been a delightful symbol of joy and imagination at the clinic, with everyone thoroughly enjoying and expressing admiration for the playful concept. The clinic has been abuzz with favorite picks from the set, truly making this festive period more memorable and fun!
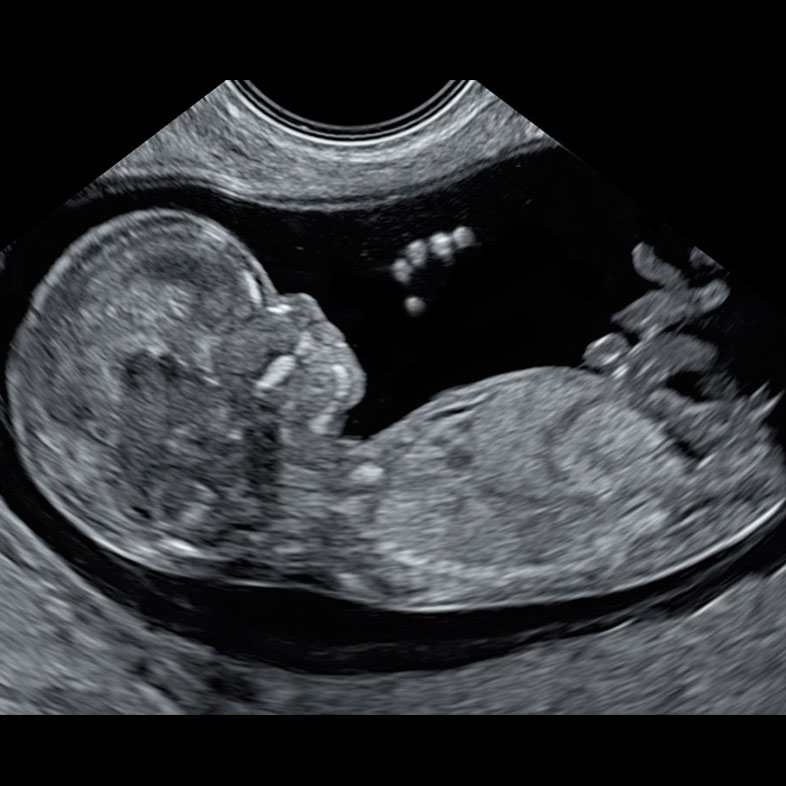
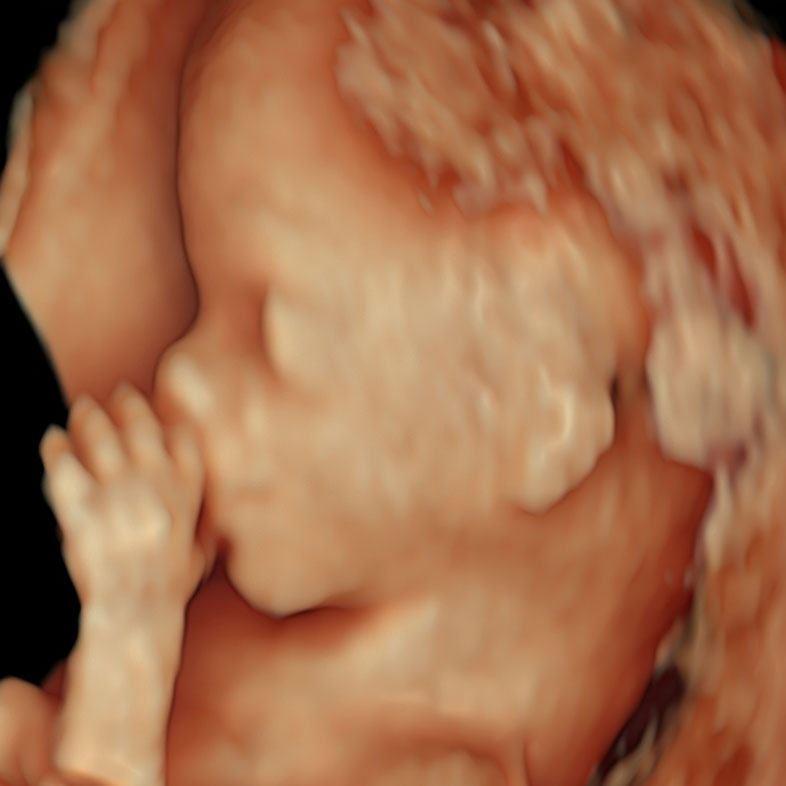
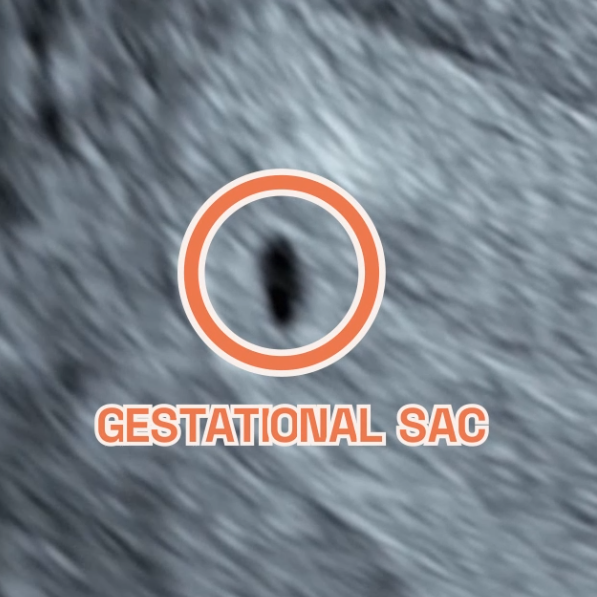
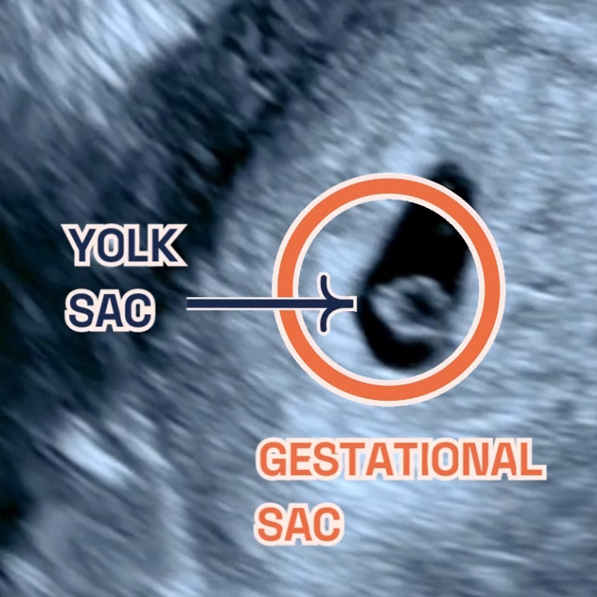
The Magic of Early Pregnancy Scans
As we gather round the festive season, it’s not just the holiday cheer we’re celebrating at London Pregnancy Clinic, but also the leaps we’ve made in pregnancy care. Our joy doubles as we reflect on the innovations and advancements we’ve embraced this year, which you can explore in-depth at London Pregnancy Clinic’s Innovations in Pregnancy Care.
Our commitment to staying at the forefront of prenatal care has led us to double our team of clinicians and embrace state-of-the-art technology for early pregnancy scans, including the critical 10 Week Scan. It’s been a year of growing, learning, and most importantly, enhancing the care we provide to you.
We celebrated each milestone, big and small, with the same enthusiasm as preparing for the holiday season. From integrating the latest ultrasound technology to training our team in the most compassionate and effective care techniques, every step forward has been aimed at ensuring your journey through pregnancy is supported, safe, and filled with joy.
Being Pregnant During The Holidays
Imagine the twinkle of Christmas lights reflected in your eyes as you envision the future with your growing family. Being pregnant during the holidaysadds an extra layer of excitement and emotion to the festive season. It’s a time filled with dreams of future Christmases, the first of many with your new addition.
You might find yourself humming lullabies instead of carols, or maybe you’re nesting with even more enthusiasm, preparing your home for both the holidays and your bundle of joy. The season’s spirit of hope and joy mirrors your own hopes and dreams for your little one.
Of course, it’s not without its challenges – navigating holiday feasts with a discerning palate or finding that perfect comfortable spot by the fireplace. Thankfully, Associates In Women’s Healthcare has come up with a list of 5 things to avoid when pregnant during the holidays. But amidst it all, there’s a unique magic to being pregnant during Christmas – a celebration of life, love, and new beginnings.
Conclusion
From heartwarming early scans to the joyous growth of our team, this holiday season is a beacon of celebration and hope. We’re geared up to enter the New Year with even more passion and dedication to your care. Remember, our doors are always open, and our team is ever-ready to support your journey with expertise and empathy.
So, here’s raising a toast to the past, present, and future – filled with health, happiness, and countless reasons to smile. Cheers to a fantastic holiday season!